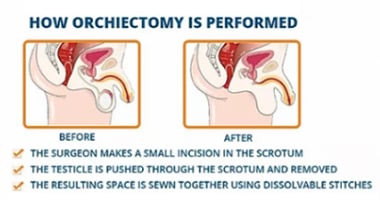
What are the Orchiectomy types and technique?
[lwptoc]
Orchidectomy is the surgical removal of one or both (surgical castration) testicles for medical reasons or at the patient’s request (voluntary castration). Operations can be of varying degrees of complexity, depending on the type of pathology. Serious health consequences arise only after the total removal of both testicles. In other cases, a man does not feel any changes in his lifestyle. If you are worried about a cosmetic defect, then it can be eliminated.
Prostate cancer continues to occupy a leading position among the severe diseases that men are susceptible to today. One of the most commonly used treatments for prostate cancer is orchidectomy. It can be performed at any stage of the disease.
Orchidectomy indications and contraindications
The main reasons for orchidectomy are:
- Purulent inflammation of the scrotum, affecting the testicle;
- Inflammation of the testicle (orchitis)
- Tuberculous tumor
- Injuries, extensive wounds
- Cancer tumor (testicular carcinoma, seminoma)
Orchidectomy is used when testicular torsion is not treated in time (when the spermatic cord is pinched). The organ is deprived of nutrition, as a result of which hypoxia (oxygen starvation of tissues) and necrosis (cell death) develop quickly.
Orchidectomy is performed for hormone-sensitive forms of prostate cancer. It has been proven that the prostate tumor grows under the influence of testosterone castration is an effective method of slowing down its development without antiandrogen therapy.
Bilateral (bilateral) Orchidectomy for prostate cancer is called androgen deprivation. Testosterone levels drop quickly (after 6-8 hours) and significantly, unlike drug methods. However, after two years, in more than half of the patients, the tumor develops again. It is because cancer develops into a castration-resistant form and becomes insensitive to testosterone.
In children, Orchidectomy is used for cryptorchidism (undescended testicle into the scrotum). In some cases, it is possible to lower it into place by building up the vessel (orchiopexy). The success of the operation does not yet guarantee the engraftment and functioning of the organ. For an abdominal form of cryptorchidism, the removal of the testicle is performed immediately. Orchidectomy is not performed at stage 4 cancer with extensive metastasis. The operation is not performed in case of severe cardiovascular pathologies, renal failure, decompensated diabetes mellitus.
Orchidectomy types and technique
Orchidectomy is performed under general, spinal, or local anesthesia. The patient is placed on his back, and the operating area is freed from hair, covered with sterile sheets, treated with antiseptics. Orchidectomy tactics depend on the severity of the condition.
- Subcapsular Orchidectomy:- Only the glandular tissue of the testicle is removed, preserving its tunica albuginea and the epididymis. Access is through an incision in the scrotum (2-3 cm); it is possible to use a laparoscopic technique. For 2-3 days, drainage is left in the empty tunica, and a pressure bandage is applied. The advantage of the method is that a palpable testicle remains in the scrotum. That is, the cosmetic defect is not as pronounced as with complete removal. The operation is suitable for the exfoliation of intracapsular T1 cancers. In this case, they must take a piece of tissue around the bed (the place where the tumor was) for histology.
- Simple orchidectomy:- through an incision along the seam of the scrotum (in the middle), the testicle and part of the spermatic cord are removed. At its end, a stump is formed and tucked back into the scrotum.
- Radical orchidectomy:- complete removal of the testicle, spermatic cord, adjacent inguinal lymph nodes. It is used when abnormal cells are found in the tunica albuginea, prostate cancer. Access is made through an incision in the groin (length 6-7 cm).
Subcapsular and simple orchidectomy can be performed under local anesthesia. The operation takes an average of 30 minutes. Radical orchidectomy is complex. It is done under general anesthesia, and the process takes at least an hour.
Postoperative period
After orchidectomy, in the first seven days, daily treatment of sutures with antiseptics, taking antibiotics, and wearing a bandage is necessary. The stitches are removed after a week. The swelling of the scrotum can last up to 2 weeks. It is normal, but it mustn’t become purple and hot at the same time. The recovery period lasts three weeks. At this time, one should not be exposed to physical stress, vibrations, visit the bathhouse, and actively move.
Complications after orchidectomy are rare. In some cases, a scrotal hematoma may occur. The use of tight bandages and timely pacing helps avoid such development.
Long term consequences
- Cosmetic defect
Some men are worried about the asymmetry resulting from a unilateral orchidectomy or complete emptying of the scrotum after bilateral. In the latter case, the so-called sail (a hanging fold of skin) remains first, which will soon shrink, pull up to the penis and dry out. It is possible to eliminate a cosmetic defect with the help of implants. They are lightweight, soft, fit in size. Usually, the implantation is performed immediately during the orchidectomy- it’s cheaper. A condition is that there must be a sufficient amount of connective tissue in the scrotum; otherwise, the prosthesis cannot be installed.
- Hormonal background
The testes produce most of the testosterone, and adrenal glands produce a small portion. After bilateral orchidectomy, the androgen level drops to a critical level for endocrine balance. Then the absence of both testicles threatens a fertile man:
- Decreased libido, deterioration of potency
- Breast augmentation (at first, the nipples will start to itch, increase in size), weight gain (on average by 4-7 kg)
- Hot flashes
- Bad sleep
- Fatigue, depression, mood swings, and tantrums
- Bone loss, development of osteoporosis
- Amyotrophy
- Excessive sweating
- Periodic attacks of shortness of breath, chills, and dizziness
- Loss of skin tone, the appearance of stretch marks due to a decrease in the secretion of the sebaceous glands, and the extinction of anabolic processes in the connective tissue
After a total orchidectomy, a man may lose vitality. There will be no strength either for going to the gym or for intimate relationships. The whole complex of disorders after orchidectomy is called “post-traction syndrome.” There are medical and physiotherapy methods to combat it.
If only one testicle is removed, then there are much fewer problems. A man can have children. The loss of one of the testicles does not necessarily affect libido, mood, and appearance since the body shifts the load to another (compensation effect). However, doctors strongly recommend not to delay conceiving a child since there is a risk of atrophy of the second testicle. Young men suffer the most from total prostatectomy. In old age, this operation has less pronounced consequences. It even reduces the symptoms of adenoma or prostatitis.
Takeaway
Orchidectomy is a simple procedure, but its consequences can be very dire. Some men deliberately want to have this operation to change their sex or as a contraception method. Doctors categorically do not recommend experimenting with your body in this way. If a complete orchidectomy was performed according to indications, then for a full life, you will have to select methods of drug support.
The information provided in this blog is for educational purposes only and should not be considered as medical advice. It is not intended to replace professional medical consultation, diagnosis, or treatment. Always consult with a qualified healthcare provider before making any decisions regarding your health. Read more