Thyroid Cancer Symptoms in Women
Table of contents
Thyroid cancer is an irregular cell growth that begins in the thyroid gland. The thyroid gland is a butterfly-shaped gland that is located at the base of the throat, close to the trachea. It has a right and a left lobe which is joined by an isthmus, a thin section of tissue. A normal thyroid is a small organ and is not detectable through the skin. The thyroid produces hormones that regulate the body’s metabolism, body weight, heart rate, blood flow and pressure, and body temperature, among other things.
What is the cause of thyroid cancer?
The exact cause of thyroid cancer is unclear. It is, however, known that thyroid cancer starts when some cells become mutated. That is, they develop changes in their DNA. These changes cause the rapid and often uncontrolled growth and multiplication of the affected thyroid cells. These cells also continue to survive when normal cells must have died. They then accumulate into a mass called a tumor, which can grow to invade nearby tissues and spread to the nearby lymph node. When untreated, the cancer further spreads beyond the neck to other parts of the body, like the bones, lungs, etc.
What are the risk factors of thyroid cancer?

Some factors can increase the risk of an individual to thyroid cancer. Some of the factors include:
- Being female.
- Family history of thyroid disease.
- Exposure to radiation.
- Goiter.
- Inflammation of the thyroid.
- Low intake of iodine.
- Obesity.
- Radiation therapy of the head and neck regions, especially during childhood.
- Gene mutations that cause endocrine disease.
What are the types of thyroid cancer?
Thyroid cancer classification is based on the type of cell from which the cancer grows; they include:
- Papillary – the majority of all thyroid cancers (about 80%) are papillary. This cancer type is slow growing; it also responds very well to treatment. Even though they often spread to the lymph nodes of the neck, they are rarely fatal and are often curable.
- Follicular: Follicular thyroid cancer accounts for about 15% of all thyroid cancer diagnoses. This type is very likely to spread to the bones and organs like the lungs.
- Medullary: this represents about 2% of thyroid cancers. This is more likely to occur in individuals with a family history of the disease. It may be ascribed to a heritable genetic mutation.
- Anaplastic – this is the hardest type of thyroid cancer to treat. It is very aggressive and can grow quickly, and often spreads to other organs and tissues. It is a rare form of thyroid cancer.
What are the stages of thyroid cancer?
The staging system is used to determine the extent of the spread of thyroid cancer. Generally, when cancer cells in the thyroid metastasize, they first spread to the nearby structures and lymph nodes. Then they further spread to the distant lymph nodes, bones, and even organs. The staging system ranges from I-IV; the higher the ascribed number, the more the cancer has spread.
What are the signs that thyroid cancer has spread?
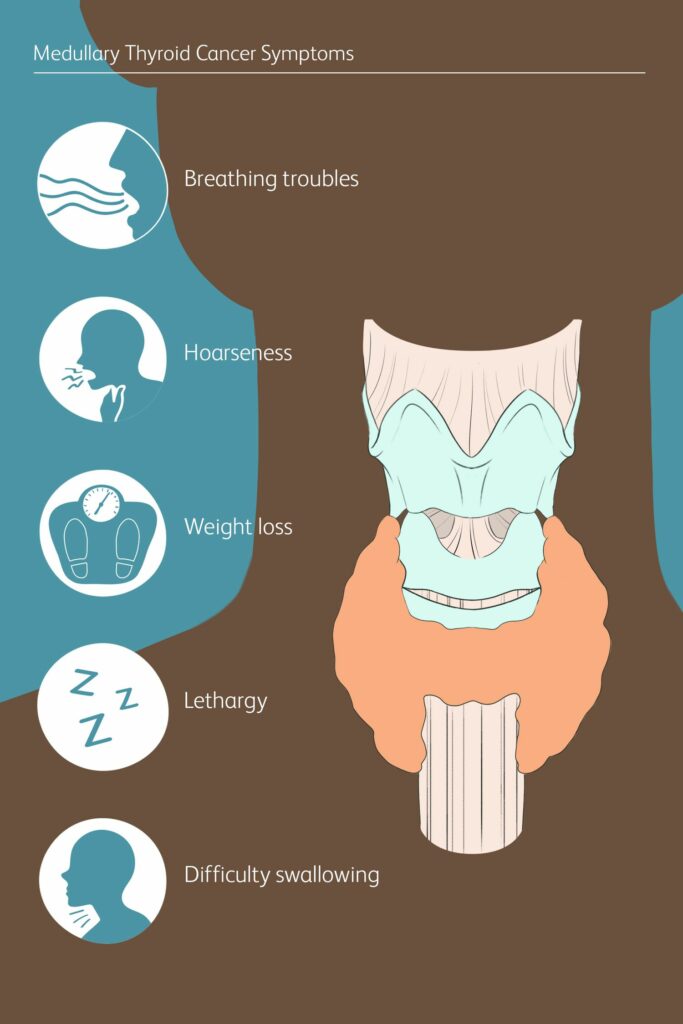
The symptoms start slowly in women, and the most common symptom is fatigue. There may be changes in the hair, nails, or skin and other complaints that may be attributed to stress, diet, aging, or various other factors. The typical thyroid cancer patients are most often women between the ages of 30 and 60, and as such, they do not notice their symptoms or may write them off and are always surprised when their condition is diagnosed as an underactive thyroid due to cancer. Thyroid disorders are more common in women than in men, most likely due to the roles of hormones which play different roles in men and women. The main signs that thyroid cancer has spread to other areas of the body may include symptoms like:
- Unexpected weight loss.
- Nausea and vomiting.
- Anorexia.
- Tiredness.
- A lump that can be felt through the neck.
- Changes to the voice, including becoming hoarser.
- Difficulty in swallowing.
- Pain in the neck and throat.
How is thyroid cancer diagnosed?
If an enlarged thyroid gland or any other symptom of thyroid cancer presents in an individual, the doctor may order one or more of the following tests:
- Physical examination – this is when the doctor examines the individual’s neck to feel for changes in the thyroid gland, like a lump. A detailed medical history, family history, and risk factor evaluation are also done.
- Blood tests – the blood test is done to check the levels of the thyroid hormones and determine if the thyroid is functioning properly.
- Biopsy – this can be done through fine needle aspiration biopsy. The doctor extracts some of the thyroid cells in order to examine for signs of cancer. A sentinel node biopsy can also determine if cancer has spread to the lymph node.
- Ultrasound imaging – this is where high-frequency sound waves are used to create pictures of body structures. The ultrasound transducer is placed on the lower neck. The appearance of the thyroid nodule on ultrasound imaging will help to determine if it is cancerous. The lymph nodes may also be examined to look for signs of cancer.
- Radioactive tracer imaging – this test uses radioactive iodine and a special camera to detect thyroid cancer cells in the body. It is usually used in surgery to find any remnant cancer cells. It is also very helpful in papillary and follicular types of thyroid cancer.
- Other imaging tests – tests like MRI and CT scans may also be used to detect signs of cancer in an individual.
- Genetic testing – a portion of medullary thyroid cancer is caused by inherited genes. The doctor might recommend genetic testing when an individual is diagnosed with medullary thyroid cancer. Knowledge of the particular inherited gene might help the individual to understand the risk of other types of cancer and how it may affect the individual’s offspring.
The information provided in this blog is for educational purposes only and should not be considered as medical advice. It is not intended to replace professional medical consultation, diagnosis, or treatment. Always consult with a qualified healthcare provider before making any decisions regarding your health. Read more


