Atrial Fibrillation Symptoms at Night
Atrial fibrillation is an abnormal or very rapid heart rate or rhythm, and this disorder can result in blood clots in the heart. It is also referred to as Afib or AF, and it begins in the atrium interrupting the normal cycle of electrical impulses in the heart. This interruption leads to a fast and uncoordinated heart rhythm that is out of synchrony with the heart’s lower chambers (ventricles). This results in the poor movement of blood from the atria to the ventricles. Read More
Top Doctors For Atrial Fibrillation Symptoms at Night Treatments
Top Hospitals For Atrial Fibrillation Symptoms at Night Treatments
Atrial Fibrillation Symptoms at Night
Table of contents
- What are the types of atrial fibrillation?
- What are the symptoms of atrial fibrillation?
- What is the cause of atrial fibrillation?
- What are the risk factors of atrial fibrillation?
- What are the complications of atrial fibrillation?
- How is atrial fibrillation diagnosed?
- What are the treatments for atrial fibrillation?
- What are the ways of preventing atrial fibrillation?
Atrial fibrillation is an abnormal or very rapid heart rate or rhythm, and this disorder can result in blood clots in the heart. It is also referred to as Afib or AF, and it begins in the atrium interrupting the normal cycle of electrical impulses in the heart. This interruption leads to a fast and uncoordinated heart rhythm that is out of synchrony with the heart’s lower chambers (ventricles). This results in the poor movement of blood from the atria to the ventricles. Episodes of atrial fibrillation may be persistent, or they may be intermittent. It is a serious medical condition that, even though it may not directly lead to death, may lead to stroke and other medical complications.

What are the types of atrial fibrillation?

Atrial fibrillation may be:
- Paroxysmal – this is where the symptoms of atrial fibrillation come and go, usually lasting from a few minutes to some hours. The symptoms may occur for as long as a week, and the episodes may occur repeatedly and may go away on their own. Some individuals with occasional atrial fibrillation need treatment.
- Persistent – in this type of atrial fibrillation, the symptoms do not go away, and the heart rhythm does not return to normal on its own. Individuals with this type of atrial fibrillation usually require medication or cardioversion in order to restore and maintain a normal heart rhythm.
- Long-standing persistent – this is a continuous type of atrial fibrillation and usually lasts longer than 12 months.
- Permanent – this type of atrial fibrillation is where the normal heart rhythm cannot be restored. Medication is required to control the heart rate and prevent blood clots.
What are the symptoms of atrial fibrillation?
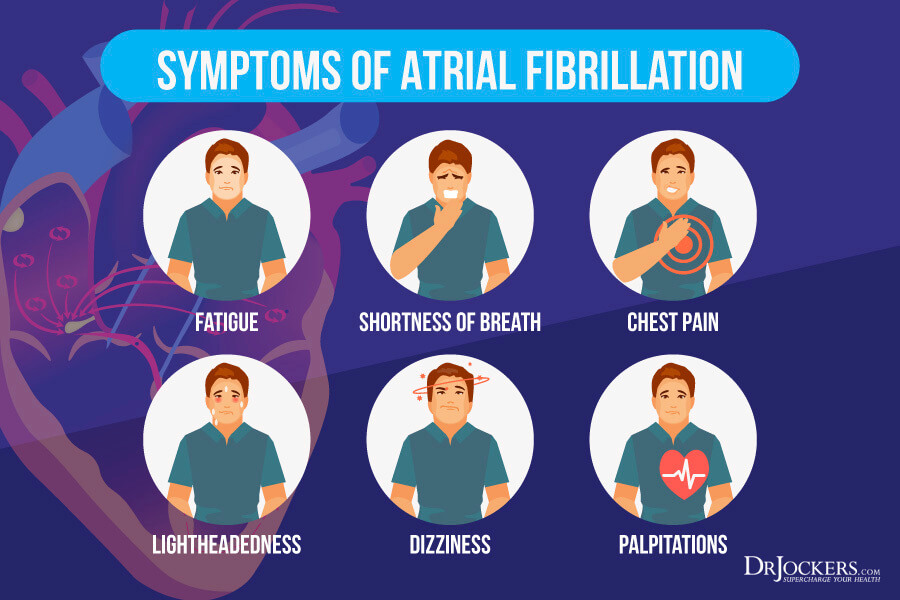
Some individuals with atrial fibrillation do not have any symptoms. The presentation of symptoms usually depends on how fast the ventricles are beating. The faster the ventricles beat, the more pronounced the symptoms of atrial fibrillation are. These symptoms can include:
- A very irregular heartbeat.
- Extreme fatigue.
- Shortness of breath.
- Heart palpitations.
- Chest pain.
- Dizziness or a feeling of lightheadedness.
- Syncope
- Reduced tolerance to exercise.
- Weakness.
What is the cause of atrial fibrillation?
The normal heart is comprised of four chambers, namely two upper atria and two ventricles in the lower. In the upper right atria, there are a group of cells called the sinus node. The sinus node is the natural pacemaker of the heart. That is, it is responsible for producing the signal that starts each heartbeat. The signal comes from the sinus node, which then travels to the upper two atria. The signal then passes through a pathway between the upper and lower chambers called the atrioventricular (AV) node.
The movement of this signal causes the heart to beat (contract), forcing blood into the heart and around the body. In atrial fibrillation, the signals in the upper atria are quite chaotic. This results in the quivering of the upper atria, leading to the crowding of the AV node with signals that are trying to make their way to the lower chambers. This leads to a fast and irregular heart rhythm. While the normal heart rate is 60-100 beats per minute, in atrial fibrillation, the heart rate may get to 175 beats per minute. The most common causes for this atrial fibrillation are issues with the structures of the heart. Though some people with A-FIB have no known heart defect or damage, some of these possible issues include:
- High blood pressure
- Coronary heart disease
- Lung disease
- Previous heart surgery
- Use of stimulants like coffee, alcohol, etc
- Viral infections
- Stress
- Heart attack
- Heart valve issues
- Congenital heart defects
- Metabolic imbalances
- Thyroid diseases
What are the risk factors of atrial fibrillation?
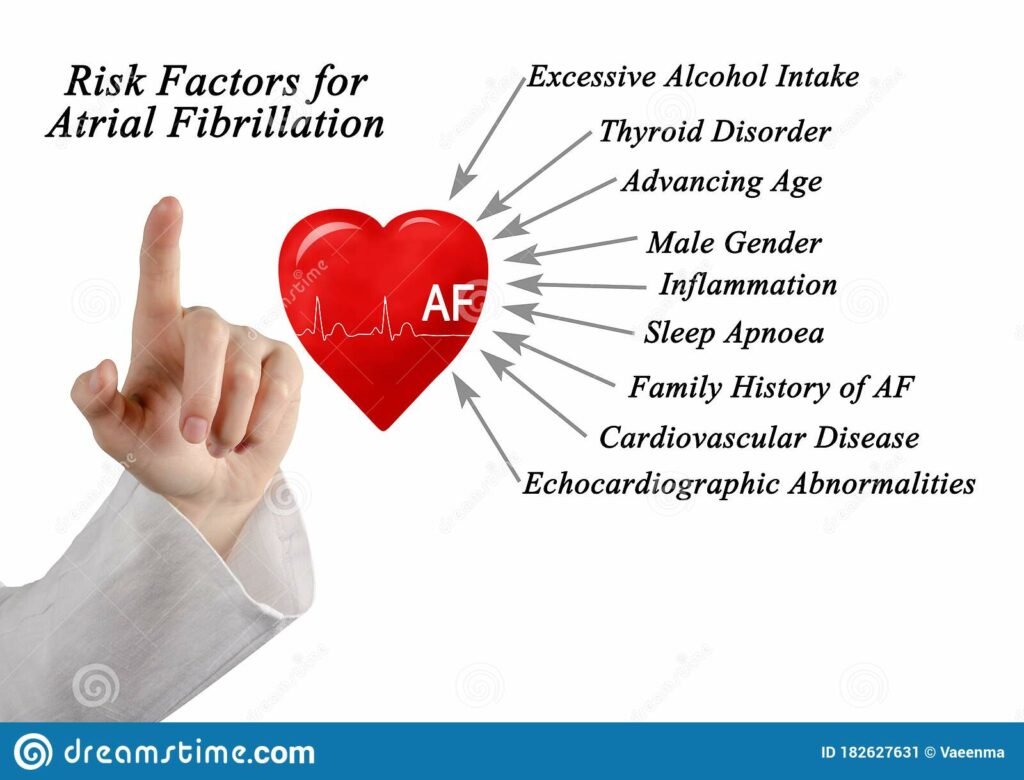
Some factors that can increase the risk of atrial fibrillation include:
- Family history – in some families, there exists an increased risk of atrial fibrillation.
- Obesity – obese individuals have a higher risk of developing atrial fibrillation.
- Age – the older an individual is, the more at risk they are of developing atrial fibrillation.
- High blood pressure – individuals with high blood pressure are at a higher risk of developing atrial fibrillation, especially in instances where the high blood pressure is not controlled with medication or changes in lifestyle.
- Thyroid disease – thyroid issues may trigger atrial fibrillation.
- Alcohol abuse – alcohol abuse may trigger atrial fibrillation in some individuals.
- Heart disease – individuals with heart disease like coronary artery issues, valve problems, congenital defects, etc., are at an increased risk of developing atrial fibrillation.
What are the complications of atrial fibrillation?
A very dangerous complication of atrial fibrillation is blood clots, and this can lead to strokes. How this occurs is that the chaotic rhythm in atrial fibrillation can cause blood to accumulate in the upper atria of the heart and form clots there. If a piece of this clot breaks free, it can travel to the brain and cause a stroke. The risk of stroke in atrial fibrillation increases when an individual gets older, other conditions like diabetes and high blood pressure may also increase the risk of stroke in atrial fibrillation. Blood thinners are usually prescribed to prevent blood clots and resulting strokes in individuals with atrial fibrillation.
How is atrial fibrillation diagnosed?
In diagnosing atrial fibrillation, the doctor gets a detailed medical history and activities of the individual, with any symptoms being experienced and any predisposing risk factors. A physical examination is also done; this may include the following:
- Checking the heart rhythm with a stethoscope.
- Checking the pulse and blood pressure.
- Checking the lungs for any signs of infection or disorder.
- Checking the thyroid gland for any issues.
- Checking for any signs of heart failure.
In addition to physical examination, some tests are done in order to diagnose atrial fibrillation. They include:
- Electrocardiogram – this is usually the first test done. It measures and records the heart’s electrical signals and allows the doctor to determine if the heart is beating normally.
- Echocardiogram – this test uses ultrasound to visualize the movement of the heart. It can show problems with heart contractions and blood flow.
- Blood tests – a blood sample test can reveal any imbalance in the blood that may be contributing to atrial fibrillation, like the levels of potassium or thyroid hormone levels.
What are the treatments for atrial fibrillation?
Atrial fibrillation therapy is aimed at controlling the heart rate, restoring the normal heart rhythm, and reducing the individual’s risk of having a stroke. Based on the severity of the symptoms, the doctor may recommend medications firs, some medications that can be prescribed for atrial fibrillation include:
- Blood thinners – these drugs reduce the risk of blood clots and a resulting stroke. Some examples are warfarin, aspirin, etc.
- Rhythm-controlling medication – these help the heartbeat in a normal sinus rhythm. Some examples include propafenone, dofetilide, sotalol, etc.
- Rate-controlling medication – these medications are prescribed to help prevent the ventricles from beating too fast. Some examples are digoxin, metoprolol, verapamil, etc.
These medications have side effects like rate control medication may make the arrhythmia worse, blood thinners may cause bleeding, heart attack, etc. However, the benefits of the medication are considered more than the risk of the side effects. Surgery may be prescribed if medications do not manage the symptoms of atrial fibrillation. Some procedures or surgeries that are done to manage atrial fibrillation include:
- Permanent pacemaker insertion – this may be placed if the individual has a slower-than-normal heart rate. This is usually done if another arrhythmia exists along with atrial fibrillation.
- Electrical cardioversion – this is the use of low-energy shocks to reset the heart rhythm electrically. This, however, may only be a temporary solution.
- Pulmonary vein ablation – this is where a catheter is used to deliver energy outside and around the pulmonary veins. This procedure is aimed at helping an individual respond better to atrial fibrillation medication.
- Left atrial appendage closure – this procedure is aimed at reducing the risk of blood clots and the resulting stroke.
- MAZE procedure – this surgery creates scar tissue that helps the heart’s electrical impulses travel in the right path.
What are the ways of preventing atrial fibrillation?
Healthy lifestyle choices can reduce an individual’s risk of heart disease, thereby preventing atrial fibrillation. Some of these choices include:
- Regular exercises
- Avoiding smoking and alcohol abuse
- Limiting caffeine intake
- Eating nutritious food
- Maintaining a healthy weight
- Managing stress and situations that can lead to stress.
“Medical Advice Disclaimer:
DISCLAIMER: THIS SITE DOES NOT PROVIDE MEDICAL ADVICE OR OPINION:
The information provided in this article or website by way of text, illustration, graphics, Images or any other form in this article or website is provided for informational purposes only. No information or material provided on this site is meant to be a substitute for a professional medical advice. Please refer to your family doctor or specialist in that field for any medical condition, diagnosis and treatment. Do not delay in contacting a professional on account of something you have read in this article or on this website.”