Basal Cell Carcinoma (BCC) on the Face)
Basal cell carcinoma BCC (on the face) is a type of cancer that grows on the parts of the skin that are constantly exposed to a lot of sunlight. They originate from the basal cells, which are a type of cell within the skin that is for producing new skin as the old one is shed. Basal cell carcinoma often appears as slightly transparent bumps or a scaly flat patch on the skin, usually on the face or any other parts of the body like the trunk, arms, or legs. Individuals with fairer skin are more at risk of developing this type of cancer. Basal cell carcinoma usually grows slowly and often does not show up until after years of intense ultraviolet light exposure. Read More
Top Doctors For Basal Cell Carcinoma (BCC) on the Face) Treatments
Top Hospitals For Basal Cell Carcinoma (BCC) on the Face) Treatments
Basal Cell Carcinoma (BCC) on the Face)
Basal cell carcinoma BCC (on the face) is a type of cancer that grows on the parts of the skin that are constantly exposed to a lot of sunlight. They originate from the basal cells, which are a type of cell within the skin that is for producing new skin as the old one is shed. Basal cell carcinoma often appears as slightly transparent bumps or a scaly flat patch on the skin, usually on the face or any other parts of the body like the trunk, arms, or legs. Individuals with fairer skin are more at risk of developing this type of cancer. Basal cell carcinoma usually grows slowly and often does not show up until after years of intense ultraviolet light exposure.
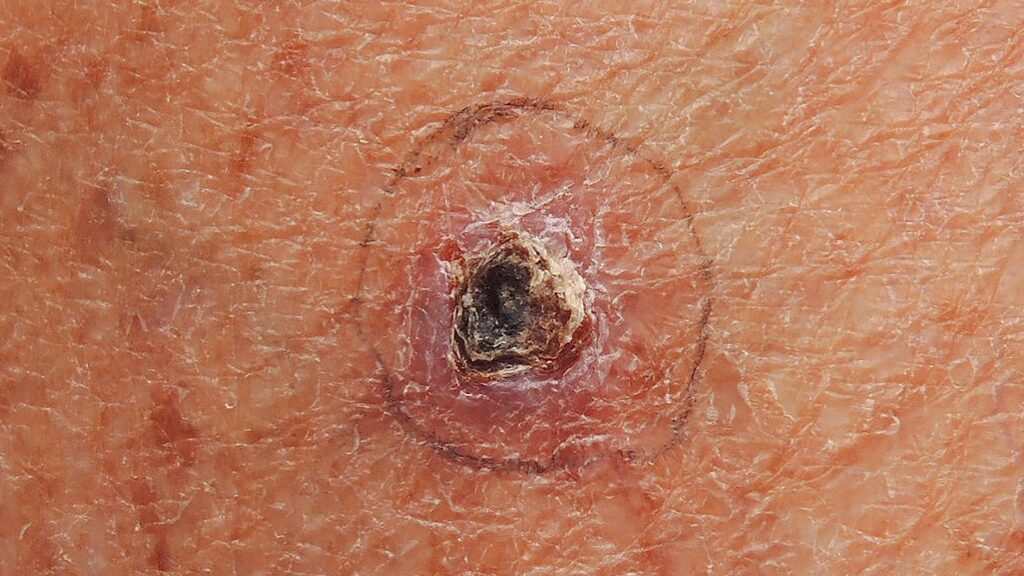
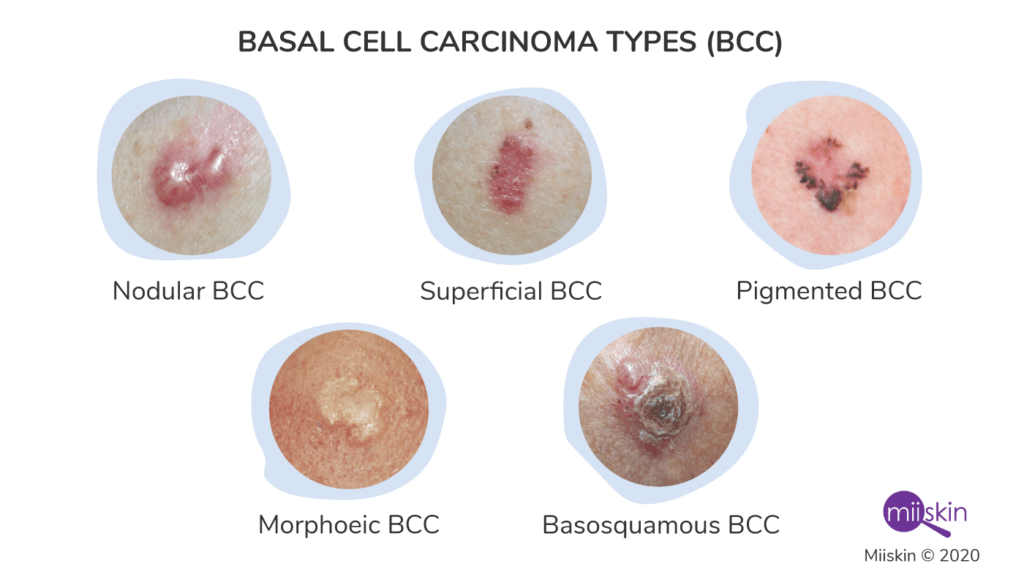
What are the types of basal cell carcinoma BCC?
There are four major kinds of Basal Cell Carcinoma. These include:
- Nodular – This is the most common form of basal cell carcinoma. They look like pimples that are round with blood capillaries around them.
- Superficial spreading – This type causes lesions that look like small yellow marks which are slightly lighter in color than the surrounding skin. They may form on the trunk, arms, and legs.
- Scelorising – These types look like scars that spread over time; it is mainly common in the face. They can also take on the form of small red dots on the skin.
- Pigmented – This type is a rare form of basal cell carcinoma, which causes hyperpigmentation.
Other types include
- Morphoeic BCC
- Basosquamous BCC
What is the cause of basal cell carcinoma?
BCC occurs when a mutation develops in the DNA of the skin’s basal cell. Basal cells are cells that are found in the epidermis of the skin, and they are responsible for the replacement of dead skin cells. The process of generating fresh skin cells can be controlled via the DNA of the basal cells. When a mutation occurs, the orderly replication is distorted. The basal cells multiply rapidly and in an uncontrolled manner and do not die when they are supposed to, causing an accumulation of cells. These accumulating cells eventually form a cancerous tumor.
What are the risk factors of basal cell carcinoma?
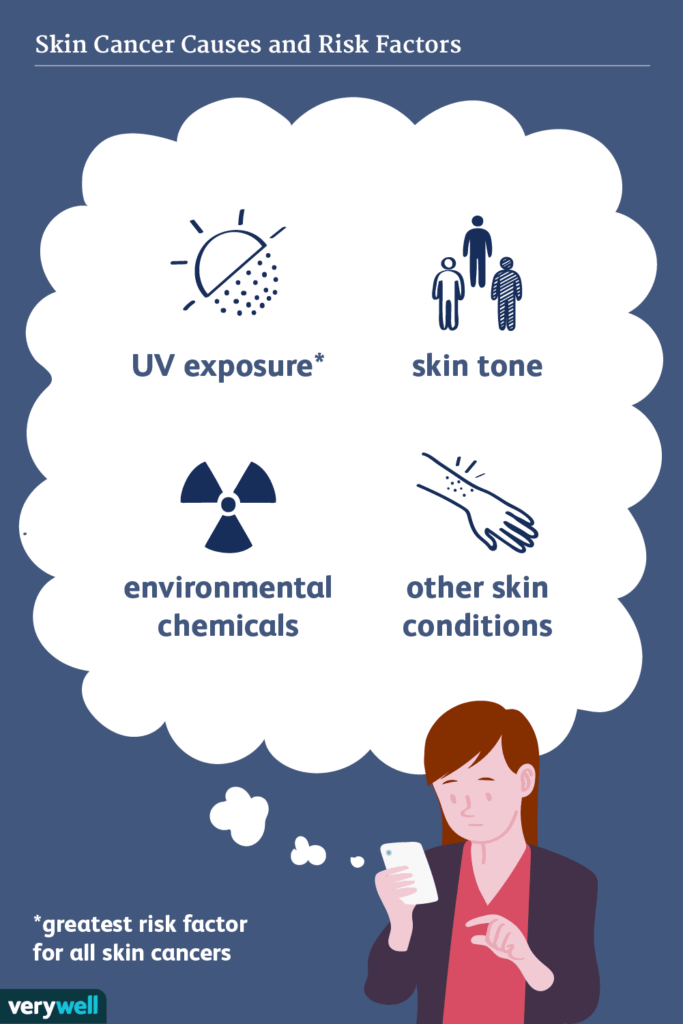
Certain factors that increase the odds of a person having basal cell carcinoma are:
- Old age – the majority of cases of basal cell carcinoma happen in old age. This is because it takes years for the cancer to develop.
- Fair skin – the risk of developing BCC is higher in people with skin types that get burnt easily, and this is common with individuals with lighter skin types.
- Chronic exposure to harsh sunlight – A lot of exposure to intense sunlight or commercial tanning beds significantly increases the risk of basal cell carcinoma. Severe sunburns increase the risk as well.
- Radiation therapy – Radiation therapy used to treat some skin conditions may increase the risk of basal cell carcinoma in previous areas of the disease.
- Immune-suppressing drugs – Some medications that can depress the immune system, like drugs used after an organ transplant, can increase the risk of this cancer.
- Exposure to arsenic – Increased intake of arsenic, a toxic metal found in the environment, can significantly increase the risk of basal cell carcinomas and other cancers. Increased intake can be through contaminated water or working in an environment with constant exposure to arsenic.
- Family or personal history of cancer – Individuals that have had and successfully treated basal cell carcinoma one or more times stand a higher risk of it happening again. If there is a history of cancer in a family, people in that family also have a higher risk of developing the disease.
How is basal cell carcinoma diagnosed?
This depends on the skin presentation of the disease. The healthcare provider might immediately suspect it based on the skin outlook of the patient. Confirmation, however, requires a detailed personal and medical history as well as a thorough physical examination. Tests are also carried out after the physical examination to aid in the confirmation of the disease; some of these tests include:
- Skin biopsy – this is where a piece of the affected skin area is removed in order to examine it under a microscope to check for signs of the disease.
- Diagnostic imaging – this is done when the health care provider suspects that the basal cell carcinoma has spread to other areas of the body; this is extremely rare, though. An MRI or a CT scan can be done to detect signs of cancer in the lymph nodes or internal organs of the individual.
These tests not only confirm the disease but also determine the stage of the disease and the best course of treatment. Some of the markers used to mark the stage of the disease include:
- Identifying the size and the extent of growth of the lesion, that is, determining if the growth is deeper into the tissue.
- Checking for signs of cancer in the lymph nodes.
- Checking for signs of cancer in the internal organs to determine if metastasis has occurred.
- Recording the speed of growth of the lesion as well as its shape and location.
How is basal cell carcinoma treated?
The main treatment of basal cell carcinoma involves its removal from the skin. For example, removing it might involve one of the following ways:
- Surgery – this involves removing the cancerous lump or lesion with a scalpel (excision or Mohs surgery)
- Electrodesiccation and curettage – this involves scrapping off the cancerous lump with a curette before burning it with a specially designed electrical needle.
- Cryosurgery – this is where the lump is frozen before being removed.
- Chemotherapy – this is where some drugs are used to target and kill the cancer cells.
- Laser therapy – this is where high-energy beams are used to remove the cancerous lump instead of a scalpel.
The cancer treatment option used will depend on the health provider after factoring in the peculiarities of the case, like the age and overall health of the individual, the location, the size, and the spread of the basal cell carcinoma.
What are the ways of preventing basal cell carcinoma (BCC)?
Some of the ways that the risk of basal cell carcinoma is reduced include:
- Avoiding the harsh sunlight during the middle of the day
- Use of sunscreen
- Wearing of protective clothing
- Avoiding frequent use of tanning beds
- Regular examination of the skin and regular appointments with a doctor
































































































