Biliary Drainage and Stenting
Percutaneous transhepatic biliary drainage (PTCD) is the placement of a drain into bile ducts using needles inserted through the skin. Biliary stenting is performed after biliary drainage if the blockage is … Read More
Top Doctors For Biliary Drainage and Stenting Treatments
Top Hospitals For Biliary Drainage and Stenting Treatments
Biliary Drainage and Stenting
Table of contents
- What is a Biliary Drainage?
- How is the biliary drainage procedure done?
- Why Do Bile Duct Blockages Occur?
- What are the causes of biliary duct blockage?
- What are the most common symptoms associated with biliary blockage?
- What Is a the Biliary Stent?
- Biliary Drainage Stent Guidelines
- Post-Surgical Guidelines
- Flushing the Biliary Drain
- FAQ
What is a Biliary Drainage?
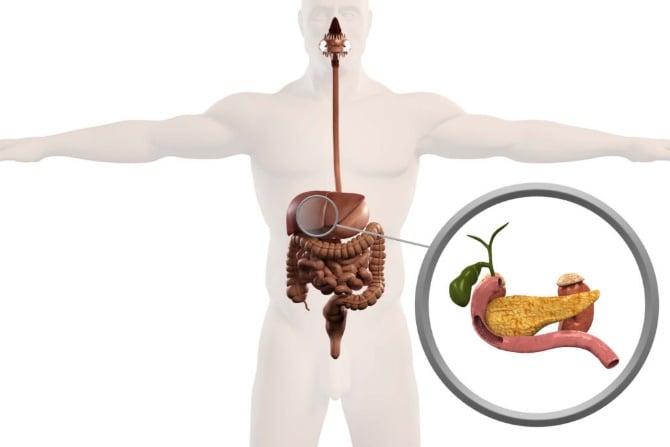
For the human body to function normally, the digestive system must break down the food we eat and absorb the necessary nutrients directly into the bloodstream. Many organs participate in this process, such as the liver producing bile juice, which helps break down the fats that enter the small intestines. The bile juice produced by the liver passes through the bile ducts and into the small intestine. However, similar to arteries and blood vessels, these bile ducts can sometimes develop blockages due to gallbladder stones or cancer.
Due to the bile duct blockage, these bile salts slowly start building up in the liver and blood. This often results in severe pain, high fever, and jaundice symptoms such as yellow eyes, dark yellow-colored urine, and pale stools. Also, fluids may accumulate in the upper and lower abdomen, causing the subject to feel bloated and restless at all times. If not treated on time, this situation can lead to severe infections, resulting in liver failure. The blockages have to be treated correctly and just in time. If the subject fails to do so, this condition eventually leads to life-threatening infection and can even result in liver failure. But biliary drainage is a procedure used to remove the built-up bile juices and other bodily attractions by using a biliary drainage tube.
How is the biliary drainage procedure done?
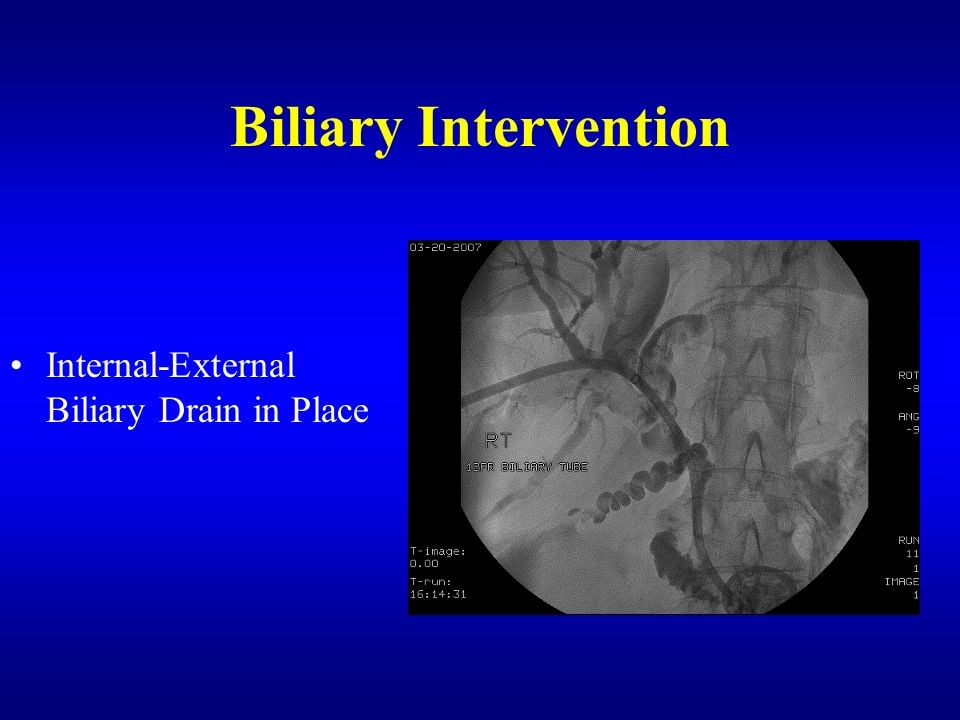
A doctor carries out the Biliary Drainage Procedure, and an interventional radiologist does this procedure using local anesthesia. With the help of an X-Ray scan or ultrasound, the radiologist inserts a tube through the liver directly into the bile duct. A guidewire placed through the tube allows direct passage of the guidewire and places the drainage stent into the desired location and position. Once the procedure is complete, the tube allows the bile juice to drain away externally into a bile bag. However, if good internal drainage can be achieved through the small intestine, then there is no need for a bile bag. Doctors often apply a low-profile device to the outer end (body) to make the tube comfortable and appear discreet. If the biliary drainage tube is inserted successfully and the blockages/obstructions are removed/relieved, the liver’s functioning improves, making the patient feel much better.
Percutaneous transhepatic biliary drain (PTCD) refers to the procedure of placing drainage into the bile ducts with needles that are inserted via the skin. Biliary stenting is done following the biliary drainage when the blockage can be considered cancerous (malignant) in order to ensure that the bile duct is patent and also to allow the drain for PTCD to be cleared.
Why Do Bile Duct Blockages Occur?
The liver secretes bile juice, which is stored in the gallbladder during meals. When we eat, the gallbladder pushes this juice into small tubes called the bile ducts. As the name suggests, Bile duct blockages are the obstructions that appear in any of the bile ducts that carry bile secreted by the liver and stored in the gallbladder to the intestine. The bile duct starts as small ductules within the liver, which carry the liver cells’ secretions. These bile ducts combine to form two major and one minor duct, which then drains the bile juice through the bile ducts into the small intestine to break down fats. A blockage of this duct prevents the bile from flowing from the liver to reach the small intestine.
What are the causes of biliary duct blockage?
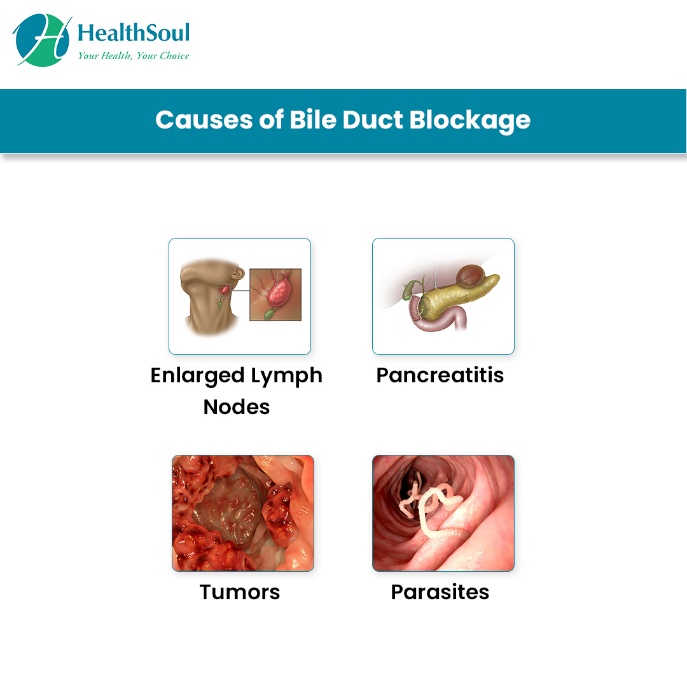
- Primary sclerosing cholangitis. This condition causes scarring and hardening of the bile ducts.
- Chronic liver disease.
- Bile duct problems present at birth.
- A liver parasite.
- Older age.
- Smoking.
- Gallstones
- Primary biliary cholangitis.
What are the most common symptoms associated with biliary blockage?

- Jaundice. Normally, bile is produced by the liver before being released into the intestinal tract.
- Itching. The presence of bilirubin in excess on the skin may cause itching.
- Light-colored/greasy stools
- Dark urine.
- Abdominal (belly) pain.
- Loss of appetite/weight loss.
- Fever.
- Nausea and vomiting
What Is a the Biliary Stent?
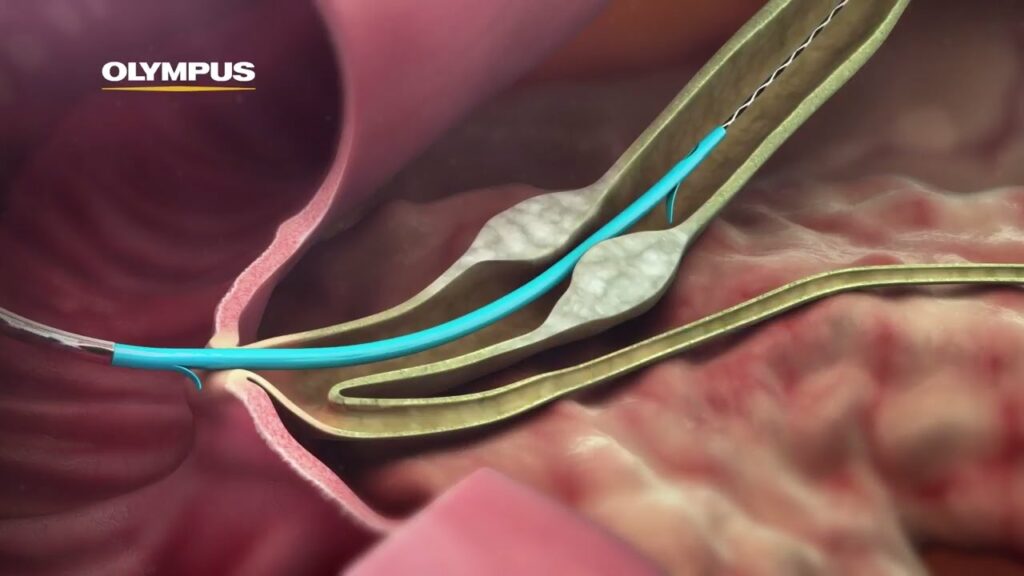
The biliary stent is a thin hollow flexible tube that has multiple small holes along the edges. This tube/stent’s primary function is to ensure that the bile from the liver flows into the intestines when the bile duct is blocked. Depending upon the type of biliary stent inserted inside the body, it may either be connected to a bile/drainage bag outside the body.
Biliary Drainage Stent Guidelines
It is imperative that one should take care of their biliary stent after placement to keep functioning and prevent further infections. Always keep the dressing/bandaged portion over the tube clean and dry. There will be a stitch holding the stent in place. However, if the stitch is ruptured, tape the stent to the skin using doctored tape and contact the concerned Radiologists at once. The Biliary Drainage Stent has a lock keeping it in place from the inside. Do NOT open the lock.
Change the dressing/bandage every day without fail. Similarly, it should be changed at once if it becomes wet or soiled or unless advised otherwise. Seek help from the doctor in case the bandage or dressing has to be changed. Always keep the drainage bag below the stent site to drain properly and ensure that the biliary stent remains in a proper position, doesn’t become twisted, and the holes along the stent do not get blocked. Use a safety pin/elastic band, yoyo, to attach the drainage bag to the clothes. NEVER let the drainage bag hang off the body as it may create tension along with the stitches, causing the accidental removal of the biliary stent.
Post-Surgical Guidelines
The patient is forbidden from driving any vehicle post-surgery because of the medications they receive during the procedure. Similarly, the patient is advised to eat minimally on the day of the surgery but can return to their original diet the next day. Our body loses lots of fluids to the drainage bag. Therefore, the subject is advised to drink lots of electrolytes to compensate for the lost fluids (for example, Gatorade, coconut water, milk, and Pedialyte).
The patient is advised to drink at least ten water glasses daily when the tube is in place. The doctor will recommend to the patient what to drink to replace the fluids lost by the drainage bag. Do NOT sleep or lie on the same side to keep the drainage tube from twisting. The patient can resume their everyday activities 24 hours post the procedure. However, patients should not lift anything heavier than 8 pounds unless advised against it. All the prescribed medications should be taken as and when scheduled unless advised against doing so. Patients can take a lukewarm shower two days after the procedure. No swimming or soaking in water is permitted as long as the tube is in place.
Flushing the Biliary Drain
The biliary drainage tube must be flushed every time the patient applies the new dressing. Since bile is a thick fluid, they will need to flush the tube to ensure proper drainage gently. The tubes’ holes must not be blocked. The doctors and caregivers will advise the patient on how often the biliary drainage tube should be flushed. To flush the biliary drain, the patient needs a prefilled 10mm sodium chloride-filled syringe and some alcohol pads. If the tube is capped and unattached to the drainage bag, use the alcohol pad to wipe the end of the tube. Slowly take the white cap off the syringe and twist this syringe onto the end of the cap. Slowly push the contents of the syringe into the biliary drain. Always remember that the fluid enters quickly when we apply gentle pressure.
FAQ
After the procedure, the doctor will schedule a follow-up with the patient regarding whether the patient’s condition has improved enough to proceed with further treatments such as chemotherapy, radiation, and surgery.
The average Biliary Drainage and Stenting Cost in India starts from USD 2000.
Here are some of the signs and symptoms post which one should immediately call the doctor:
1) Redness,
2) Swelling,
3) Foul Odor,
4) Drainage,
5) Abdominal Pain
6) Nausea
7) Vomiting
8) Light Colored Stools
9) Shaking Chills
10) High Fever
11) Yellowing of the Skin/Eyes
12) Dark Urine
If any of the above signs and symptoms develop around the skin, one must immediately consult the doctor. If the stent is capped, uncap it and attach it to the drainage bag. Always ensure that the biliary drainage bag is below the level of the tube site. However, if the stent tube is already attached to the drainage bag, gently remove the dressing, check whether the stent is twisted, and straighten the tube if it is twisted. Even if the fluid does not start flowing once you straighten it, the patient must flush the tube gently. But if all these steps fail to relieve the symptoms, one should immediately call the doctor or visit the nearest hospital/emergency room.
The biliary drainage tube must be changed from time to time to reduce the risk of infection and ensure it drains properly. If the patient does not have a follow-up visit scheduled, call the doctor or the hospital to arrange for one.
Picture Courtesy: healthsoul
The risks associated with the biliary drainage procedure are:
1) Infection
2) Bleeding
3) Bile leak
4) Injury (puncturing) to the gallbladder or intestine causing bile to leak into the abdomen.
5) Sepsis
The stent placement can cause pain or discomfort initially for a few days, which might disappear later. However, very rarely the stent placement can cause inflammation of the pancreas, which can result in back pain.
A biliary stent must be replaced every three to six months to avoid inflammation of the biliary ducts. In case we leave the stent in the body for a longer duration. It can result in causing foreign body reaction around the stent, infection, stent blockage, displacement of the stent (movement of the stent from its inserted position), and pancreatitis (inflammation of the pancreas).



























































































