Celiac Disease Treatment
Celiac disease, often referred to as celiac-sprue or gluten-sensitive enteropathy, is an immune response to gluten, which is a protein that can be found in barley, wheat, and rye. If a person is diagnosed with celiac disease, eating gluten triggers an immune response in the small intestine. Read More
Top Doctors For Celiac Disease Treatment Treatments
Top Hospitals For Celiac Disease Treatment Treatments
Celiac Disease Treatment
Table of contents
What is Celiac Disease?
Celiac disease, often referred to as celiac-sprue or gluten-sensitive enteropathy, is an immune response to gluten, which is a protein that can be found in barley, wheat, and rye. If a person is diagnosed with celiac disease, eating gluten triggers an immune response in the small intestine. As time passes, this process can damage the lining of the small intestine and stops it from absorption of certain nutritional substances (malabsorption). The intestinal damage often causes diarrhea, fatigue, weight loss, bloating, and anemia and can lead to severe complications. Malabsorption may affect the growth and development of children, as well as causing symptoms that are seen in adults. There is no cure for celiac disease. However, for the majority of people, adhering to a gluten-free diet will assist in managing symptoms and aid in the healing of the intestinal tract.
Causes
The inherited genes combined with eating foods with gluten and other factors can contribute to celiac disease, but the precise cause isn’t known. Infant-feeding practices, gastrointestinal infections, and gut bacteria might also contribute. Celiac disease may become active following the birth of a child, surgery, pregnancy, viral infection, or extreme emotional stress.
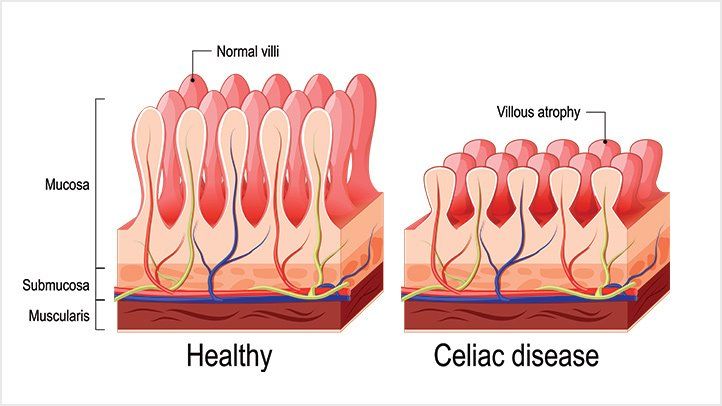
The body’s immune system reacts too strongly to gluten-containing foods. This reaction causes damage to the tiny hairy projections (villi), which are found in the small intestine. Villi absorb minerals, vitamins, and other nutrients through the meals we consume. If the villi are damaged, one can’t get enough nutrients, no matter how much one eats.
What are the risk factors for celiac disease?
Celiac disease is more prevalent in those who with the following risk factors:
- Heredity
- Type 1 diabetes mellitus people
- Autoimmune thyroid disease
- Addison’s disease
- Down syndrome
- Turner syndrome
- Microscopic colitis
- Irritable bowel syndrome
- Primary biliary cirrhosis, etc.
Symptoms
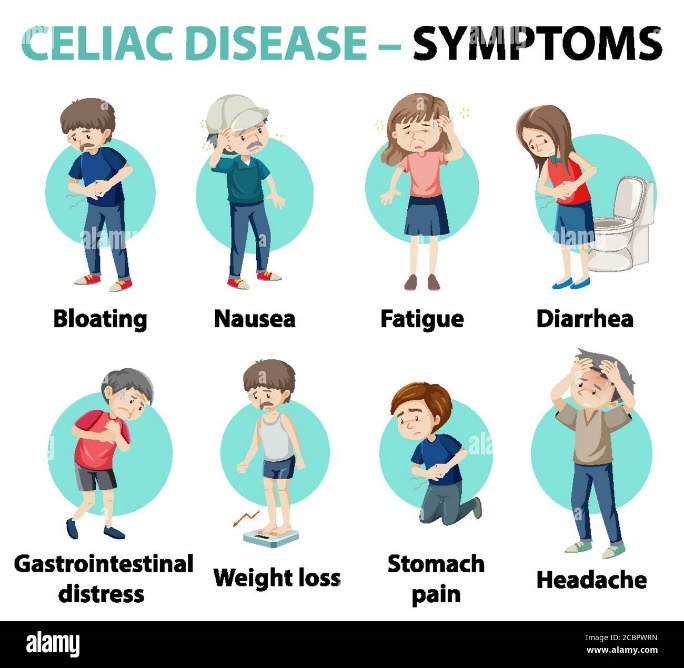
The symptoms and signs of celiac disease are quite different and vary between adults and children. Digestive signs and symptoms for adults include:
- Diarrhea
- Fatigue
- Weight loss
- Bloating and gas
- Abdominal pain
- Nausea and vomiting
- Constipation
How is celiac disease diagnosed?

These tests make the diagnosis of the disease. They include:
- Laboratory tests: They include a complete blood test done to check for immune system abnormality, liver function test, kidney function test, alkaline phosphate level test, serum albumin level, and cholesterol test.
- Serological test: This test looks for antibodies in the blood. The elevated levels of specific antibodies in blood suggest an immune reaction to gluten.
- Genetic testing: HLA-DQ2 and HLA-DQ8 are done to rule out celiac disease.
- Stool test
- Oral tolerance test: This test (oral D-xylose tolerance test) can help to reveal carbohydrate malabsorption.
- Imaging test: They include small bowel barium studies, which help diagnose the untreated condition.
- Endoscopy and capsule endoscopy: During this procedure, a small thin, flexible tube along with a camera is inserted through the mouth, into the esophagus, stomach, and first part of the small intestine (duodenum) to look for any signs of abnormalities in the upper GI area.
- Biopsy: During this procedure, a small sample of abnormal tissue is taken out while doing endoscopy and later send the sample for histopathological studies.
How is celiac disease treated?
There is no permanent cure for it. Change in our lifestyle and diet management can help in minimizing the complications associated with celiac disease. Treatment plans for the condition are listed below:
- A long-term, strict gluten-free diet is the best method to treat it. A few of the food that contains gluten are- wheat, rye, barley, malt, graham flour, semolina, etc. All these should be avoided.

- By removing gluten from the diet will automatically reduce the inflammation of the intestine.
- Vitamin and mineral supplement
- Medications to control inflammation of the intestine are:
- Steroids to control inflammation. It can ease severe signs and symptoms associated with the disease.
- Other drugs include- budesonide, azathioprine, etc.
What are the most common complications associated with celiac disease?
Complications associated with the condition are:
- Malnutrition
- Infertility and miscarriage
- Bone weakening
- Nervous-related problem
- Lactose intolerance
- Pancreatic disease
- Cancer, etc.
FAQ
Non-refractive celiac disease is often due to contamination of the diet with gluten. People diagnosed with this disease don’t respond to the gluten-free diet. They generally might have irritable bowel disease, bacterial overgrowth in the intestine, poor pancreas function, refractory celiac disease, and microscopic colitis.
In rare cases, the intestinal injury of the disease doesn’t respond to a strict gluten-free diet. In such cases, it is known as refractory celiac disease. There is no cure for this disease. However, research studies are going on regarding the cure of this disease.
The other health issues that can accompany celiac disease are:
1) Malnutrition
2) Osteoporosis
3) Cancer of the intestine (very rarely)
4) Autoimmune diseases include- thyroid or liver diseases, type 1 diabetes, rheumatoid arthritis, Sjogren’s syndrome, and autoimmune liver disorder.
It cannot be prevented entirely. However, a change in diet plan and following a healthy lifestyle can help in minimizing the complications associated with the disease.
The prognosis of the disease varies from person to person. Early diagnosis and early treatment, and regular follow-up with the doctor will result in an excellent prognosis for this disease. People, if left untreated, can result in causing severe complications associated with the disease. However, the disease can rarely be fatal.



























































































