Endometrial Cancer Staging
Endometrial cancer can also be referred to as uterine cancer, one of the commonest types of cancer affecting the uterus. Endometrial cancer is usually detected early because it frequently causes abnormal bleeding from the vagina. Surgical removal of the uterus (hysterectomy) often resolves the cancer when detected early. Read More
Top Doctors For Endometrial Cancer Staging Treatments
Top Hospitals For Endometrial Cancer Staging Treatments
Endometrial Cancer Staging
Table of contents
- What is Endometrial Cancer?
- What are the symptoms of endometrial cancer?
- What causes endometrial cancer?
- What are the types of endometrial cancers?
- What factors increase an individual’s risk for this cancer?
- What is Endometrial Cancer Staging?
- How is endometrial cancer diagnosed?
- What is the treatment for endometrial cancer?
- How can this cancer be prevented?
Endometrial cancer staging is a method used in grouping the severity of endometrial cancer. Trying to understand how doctors do this can take a lot of work. So, in this article, we will discuss endometrial cancer, its meaning, the symptoms, the diagnosis, and its staging and treatment options.
What is Endometrial Cancer?
This type of cancer originates in the uterus, in the endometrium, to be precise. The uterus is a hollow organ housed in the lower abdomen, responsible for fetal housing and development. The endometrium is the inner lining of the uterus, and cancer begins in the cells that form this lining (the endometrial cells). Endometrial cancer can also be referred to as uterine cancer, one of the commonest types of cancer affecting the uterus. Endometrial cancer is usually detected early because it frequently causes abnormal bleeding from the vagina. Surgical removal of the uterus (hysterectomy) often resolves the cancer when detected early.
What are the symptoms of endometrial cancer?
The most common symptom seen in endometrial cancer is abnormal vaginal bleeding. Some of the irregularities include:
- Bleeding between menstrual cycles
- Bleeding after menopause
- Changes in heaviness or length of menstrual periods
Some of the other symptoms noticed are:
- Unexplained weight loss
- Painful intercourse
- Lower abdominal or pelvic pain
- Blood-tinged vaginal discharge
When one notices these symptoms, the individual must see a doctor for a proper examination and diagnosis.
What causes endometrial cancer?
While the exact cause of this cancer is unknown, it is believed that there arise mutations in the DNA of the endometrial cells, which then turns normal healthy cells abnormal. These abnormal cells begin to grow and multiply in an uncontrolled manner, and they do not die as normal cells do. They accumulate and eventually form a mass or tumor. These tumor cells invade nearby cells and can break off and travel or metastasize to other parts of the body. Some experts believe that changes in the level of hormones like estrogen and progesterone in the body play a role in this issue. They believe that the fluctuation of these hormones affects the endometrium. For example, an increase in estrogen levels causes increased division and multiplication of the endometrial cells.
What are the types of endometrial cancers?
Endometrial cancers can be classified based on their look under a microscope (histologic types). These classifications include:
- Adenocarcinoma
- Uterine carcinoma
- Squamous cell carcinoma
- Small cell carcinoma
- Transitional carcinoma
- Serous carcinoma
What factors increase an individual’s risk for this cancer?
Some of the factors that increase the risk of endometrial cancer include:
- Hormonal imbalance – fluctuations in the balance of progesterone and estrogen elicit changes in the endometrium. Any condition or situation that causes an increase in estrogen level and not progesterone can increase the risk of endometrial cancer. Examples are hormonal medications after menopause, irregular ovulation patterns, which can happen in PCOS (polycystic ovarian syndrome), a type of ovarian tumor that secretes estrogen, etc.
- Older age – the risk of endometrial cancer increases with age, and it most often occurs after menopause.
- Obesity – Endometrial cancer is more common in obese women. Excess fat can cause a disruption in the body’s hormonal equilibrium.
- Never been pregnant – an individual that has never been pregnant has an increased risk of endometrial cancer than others that have had at least one pregnancy.
- More menstruation years – starting menstruation at an earlier age or beginning menopause at a later age increases the risk of endometrial cancer; this is due to the more exposure the endometrium has to estrogen.
- Diabetes – the link between diabetes to endometrial cancer is not clear. However, type 2 diabetes is common in overweight or obese individuals, and obesity is a factor that increases cancer risk.
- History of cancer – a family history of cancer also makes an individual more at risk of developing endometrial cancer. Also, an individual that has had ovarian or breast cancer has more risk of developing ovarian cancer.
- Lynch syndrome – also called hereditary nonpolyposis colorectal cancer (HNPCC). It is caused by a hereditary gene mutation. This syndrome generally increases an individual’s chances of developing cancer.
What is Endometrial Cancer Staging?
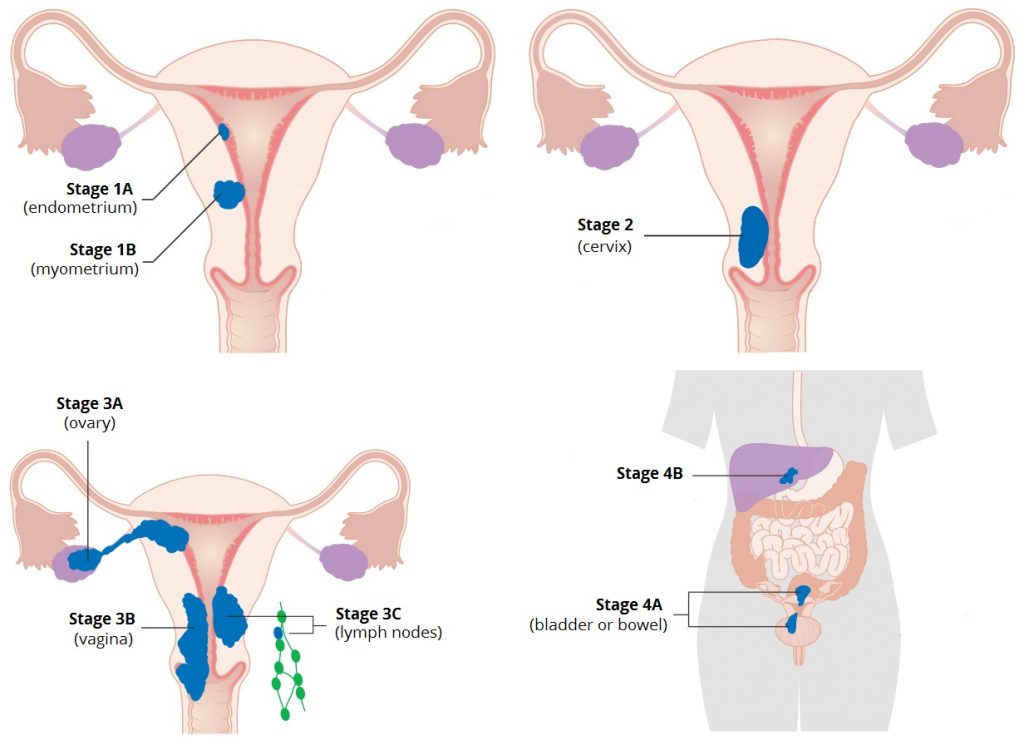
This is a system used to determine the seriousness of the spread of endometrial cancer because, over time, cancer has a tendency to spread to other parts of the body. The cancer is classified into four stages based on its spread. These stages are:
- Stage 1 – this is when the cancer is only located in the uterus.
- Stage 2 – this is when the cancer is found in both the uterus and cervix
- Stage 3 – This is when cancer has spread outside the uterus but not as far as the rectum or bladder. It might be spread to the ovaries, the vagina, the fallopian tubes, and the nearby lymph nodes.
- Stage 4 – This is where cancer has spread further than the pelvic area. It may be seen in the bladder, the rectum, and other distant organs.
The stage of cancer also is considered when a treatment plan is being prepared; the prognosis or long-term outcome is also determined by the staging of cancer. Like most other cancers, endometrial cancer is easier to manage and treat when it is caught or detected early.
How is endometrial cancer diagnosed?
When individuals notice any of the symptoms mentioned above, they are advised to seek medical attention immediately. The doctor will then inquire about the individual’s medical history, ask about the symptoms experienced, and conduct a physical examination. A pelvic exam is also done to identify any abnormalities in the reproductive organs. A transvaginal exam may also be done to rule out any vaginal abnormalities. Diagnostic imaging like ultrasound may be used for the transvaginal examination, after which one or more of the following tests may be ordered:
- Endometrial biopsy
- Hysteroscopy
- Dilation and curettage
The collected endometrial tissue is then sent to a lab for further tests. If the tests are positive for endometrial cancer, other tests like blood tests, x-ray, and other imaging tests may be done to determine the cancer stage.
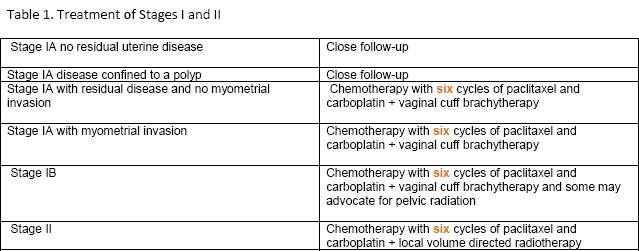
What is the treatment for endometrial cancer?
Different treatment courses may be employed depending on the staging and type of endometrial cancer. The general health and preferences of the patient are also considered in deciding an appropriate plan. Some of the therapies include:
- Surgery – also known as hysterectomy, this is the surgical removal of the uterus. The removal is usually carried out at the same time. The ovaries and fallopian tubes may also be removed as well, known as bilateral salpingo-oophorectomy (BSO). Depending on the spread of cancer, additional surgeries may be done.
- Radiation therapy – this is the use of high-energy beams to kill the cancer cells. Two types of radiation therapy can be used; external beam therapy, which focuses the energy beams on the uterus from the outside, and internal radiation therapy, whereby radioactive materials are placed in the vagina or uterus. This is also known as brachytherapy. Radiation therapy may be done before or after the surgery.
- Chemotherapy – this is the use of drugs to kill cancer cells. It can be one drug or a combination of drugs. The drug/drugs can also be administered via an IV infusion or oral medication. This method of treatment is suitable for endometrial cancers that have spread to other body parts.
- Targeted therapy and Immunotherapy – targeted therapy is when drugs are administered in order to target specific changes in cancer cells. This method of therapy is relatively new and still undergoing clinical trials. Immunotherapy is treatment with drugs that boosts the immune system in order for them to recognize and eliminate the cancer cells. Both targeted therapy and immunotherapy are occasionally used together or combined with chemotherapy.
- Hormone therapy – this is the use of hormones or hormone-blocking medication to alter the body’s hormone levels. This can help in slowing down the growth of endometrial cancer cells. This method might be used for cancers that are in stage 3 or stage 4 or reoccurring cancers. It is usually combined with chemotherapy.
How can this cancer be prevented?
- Consult a doctor about risks in hormone therapy after menopause – Hormone therapy after menopause increases the risk of endometrial cancer unless the person has undergone a hysterectomy, so it should be discussed with a doctor before an individual goes ahead with it. A way to reduce the risk might be a combination of estrogen with progestin.
- Maintaining a healthy weight – since obesity increases the risk of endometrial cancer, working hard to maintain a healthy weight is imperative in its prevention. Improving the physical activity level and reducing calorie intake are ways to maintain a healthy weight.
































































































