Eosinophilic Granulomatosis with Polyangiitis
What is Eosinophilic granulomatosis with polyangiitis? Eosinophilic granulomatosis with polyangiitis is abbreviated as EGPA and can also be referred to as “Churg-Strauss Syndrome“, “Allergic Granulomatosis“, and “Allergic Angiitis“. Eosinophilic granulomatosis with polyangiitis is a defect resulting in the inflammation of the blood vessels in the system. This case is detrimental as it impedes blood flow […] Read More
Top Doctors For Eosinophilic Granulomatosis with Polyangiitis Treatments
Top Hospitals For Eosinophilic Granulomatosis with Polyangiitis Treatments
Eosinophilic Granulomatosis with Polyangiitis
What is Eosinophilic granulomatosis with polyangiitis?
Eosinophilic granulomatosis with polyangiitis is abbreviated as EGPA and can also be referred to as “Churg-Strauss Syndrome“, “Allergic Granulomatosis“, and “Allergic Angiitis“. Eosinophilic granulomatosis with polyangiitis is a defect resulting in the inflammation of the blood vessels in the system. This case is detrimental as it impedes blood flow into certain tissues and organs. This obstruction of flow affects the organs and tissues badly as it can damage the system. Though, it is not contagious.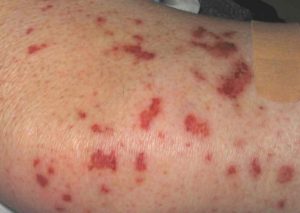 Picture Courtesy: emedicine
Eosinophilic granulomatosis with polyangiitis is a rare case with minimal occurrences, though it is said to have no cure, and a common symptom indicating a possible presence of the EGPA is asthma. Other problems like rashes, pain, gastrointestinal bleeding, hay fever, and numbness can all be experienced.
Allergic granulomatosis is also known to be an autoimmune disorder affecting blood vessels of small and medium-sized diameter in people majorly. Also, this occurs in people with previous cases of airway allergic hypersensitivity.
Patients with the EGPA have heightened allergic-type blood cells known as eosinophils. Eosinophils are white blood cells that account for 5% or less of the whole white blood cell present in the body. When the Churg-Strauss syndrome is present, the eosinophils become responsible for more than 10% of the white blood cells in the body.
The inflammation of the blood vessels is known as “Vasculitis“. Vasculitis results in unusual weakness of the vessels, and they tend to stretch. This case is known as an “Aneurysm“. The blood vessel walls become thinner, which can make them rupture, leading to leakage of blood into the tissues.
Picture Courtesy: emedicine
Eosinophilic granulomatosis with polyangiitis is a rare case with minimal occurrences, though it is said to have no cure, and a common symptom indicating a possible presence of the EGPA is asthma. Other problems like rashes, pain, gastrointestinal bleeding, hay fever, and numbness can all be experienced.
Allergic granulomatosis is also known to be an autoimmune disorder affecting blood vessels of small and medium-sized diameter in people majorly. Also, this occurs in people with previous cases of airway allergic hypersensitivity.
Patients with the EGPA have heightened allergic-type blood cells known as eosinophils. Eosinophils are white blood cells that account for 5% or less of the whole white blood cell present in the body. When the Churg-Strauss syndrome is present, the eosinophils become responsible for more than 10% of the white blood cells in the body.
The inflammation of the blood vessels is known as “Vasculitis“. Vasculitis results in unusual weakness of the vessels, and they tend to stretch. This case is known as an “Aneurysm“. The blood vessel walls become thinner, which can make them rupture, leading to leakage of blood into the tissues.
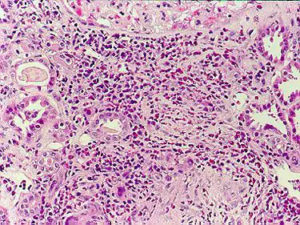 Picture Courtesy: emedicine
Eosinophilic granulomatosis with polyangiitis affects the lungs, skin, joints, sinuses, nose, gastrointestinal tract, brain, kidney, or heart.
EGPA affects all age groups ranging from children to adults. . Though the average age of diagnosis ranges from 35 to 50 years of age, it generally affects men and women. Therefore, it is not gender-specific.
Picture Courtesy: emedicine
Eosinophilic granulomatosis with polyangiitis affects the lungs, skin, joints, sinuses, nose, gastrointestinal tract, brain, kidney, or heart.
EGPA affects all age groups ranging from children to adults. . Though the average age of diagnosis ranges from 35 to 50 years of age, it generally affects men and women. Therefore, it is not gender-specific.
What are the risk factors associated with EGPA?
The risk factors that are associated with the EGPA are listed below:-
-
- Asthma or airway problem:
-
-
-
- Age
-
What are the complications associated with EGPA?
Many organs are affected, such as the kidneys, heart, joints, lungs, gastrointestinal tract, etc. This disease can be fatal if not treated. Complications that could occur vary depending on the affected organ. Complications are explained below:-
-
- Skin Scarring
-
-
-
- Kidney Damage
-
-
-
- Heart Disease
-
-
-
- Peripheral Nerve Damage
-
How is EGPA diagnosed?
The diagnosis of the EGPA can be made through the following:-
-
- Physical Examination
-
-
-
- Medical History
-
-
-
- Urinalysis
-
-
-
- Blood Test
-
-
-
- Imaging Test
-
Eosinophilic granulomatosis with polyangiitis Prevention
There is no specific cause for the EGPA. Therefore, there is no way of preventing the disease from occurring.Eosinophilic granulomatosis with polyangiitis Treatment
Medications like immunosuppressive drugs that suppress the activation rate of the immune system are the best for the treatment of the EGPA. The drugs administered are based on the patients and affected organs. The drugs are:-
-
- Glucocorticoids
-
-
-
- Corticosteroids
-
-
-
- Biologic Medications
-
What is the recovery rate of EGPA?
The duration of the intake of the medications administered can depend on the patient. Though, recovery of the patient ranges from a year to two years. The mortality rate without treatment is placed at 25% after 5 years.Symptoms
EGPA symptoms can vary from person to person.
EGPA symptoms occur in three phases that may overlap.
- Prodromal
In this phase, the disease might be persistent over a long period whereby patients develop nasal polyposis, allergic rhinitis, asthma, or even a combination of a few symptoms.
- Second Phase
In this phase, the peripheral blood and tissue eosinophilia come to play, and the situation can almost be regarded as a Loffer syndrome which involves eosinophilic gastroenteritis and eosinophilic pneumonia.
- Third Phase
This phase is severe and life-threatening as the vasculitis (inflammation) develops and the organs begin to fail. Symptoms like fatigue, weight loss, e.t.c, are excessive in this state.
These phases may not occur serially, and the timing before each of them varies.
Other symptoms that may present themselves are:
- Fever.
- Hay fever.
- Fatigue.
- Loss of appetite.
- Joint pain.
- Pain in the muscle.
- Scars on the skin.
- Cough.
- Numbness.
- Pain in the abdomen.
- Bleeding in the gastrointestinal tract.
- Blood in stools and urine.
- Shortage of breath.
Causes
The specific cause of Eosinophilic granulomatosis with polyangiitis is not known. The human immune system contributes to the presence of EGPA. In an allergy mechanism where the tissues in the body are injured by the white blood cell, eosinophils’ products can also be responsible.
The major responsibility of the immune system is to fight invaders like germs, bacteria, and viruses responsible for diseases, infections, and other related problems. When this immune system becomes hyperactive, it can result in inflammation.
T lymphocytes in the body can be activated, therefore, increasing the inflammation of the vessels. Patients with a history of nasal polyposis, asthma, or allergic rhinitis are liable to have the EGPA.
Overview of EGPA
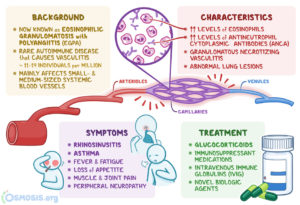
Picture Courtesy: Osmosis
FAQ
-
-
- How common is the Eosinophilic granulomatosis with polyangiitis?
-
The EGPA is a rare condition as it is said to occur in 3 people per 1 million people in a year.
-
-
- Who is affected by EGPA?
-
The EGPA can occur in anyone of any age range, but statistics show that the EGPA occurs in men and women between the ages of 35 to 50 years.
-
-
- Is EGPA a type of cancer or autoimmune disorder?
-
The eosinophilic granulomatosis with polyangiitis is not a type of cancer, and it is not associated with any autoimmune disorder.
-
-
- Does EGPA run in the family?
-
Even though the EGPA is associated with hereditary asthma, the EGPA can be passed through the genes.
-
-
- Are there side effects of treatment?
-
Immunosuppressive drugs can have side effects, so it is mandatory to visit the clinic for close monitoring regularly.










































