Functional Dyspepsia
Functional dyspepsia is a term that can be classified as a “non-ulcer dyspepsia” or “Indigestion” but possess similar symptoms which are mostly intermittent with ulcer pain. Functional dyspepsia indicates signs and symptoms associated with the upper digestive tract consisting of the esophagus, small intestine, and stomach. Functional dyspepsia can also be called “Pyloro-duodenal Irritability“, “Nervous […] Read More
Top Doctors For Functional Dyspepsia Treatments
Top Hospitals For Functional Dyspepsia Treatments
Functional Dyspepsia
Table of contents
What is functional dyspepsia?
Functional dyspepsia is a term that can be classified as “non-ulcer dyspepsia” or “Indigestion” but possess similar symptoms, which are mostly intermittent with ulcer pain. It indicates signs and symptoms associated with the upper digestive tract, including the esophagus, small intestine, and stomach. Functional dyspepsia can also be called “Pyloro-duodenal Irritability,” “Nervous dyspepsia,” “Pseudo-ulcer syndrome,” or “Gastritis.”
It can be categorized into two syndromes. They are epigastric pain syndrome, which involves stomach pain and discomfort, and postprandial distress syndrome, which involves the stomach’s capacity when eating and ingestion. The meaning of dyspepsia is a pathological disorder involving indigestion that results in pain in the stomach associated with nausea feeling and possibly heartburn.
Functional dyspepsia is said to be common and persistent. Therefore, it is said to be functional due to the inability to determine the cause and describe the symptoms involved. This chronic disorder does not have any specific cause regardless of the fact the signs and symptoms can be mistaken for an ulcer due to the discomfort and stomach ache associated with excess belching and bloating. A term described as “Peristalsis” influences functional dyspepsia as it affects the sensibility and mobility in the digestive tract. The peristalsis involves pumping and contracting the upper digestive tract when eating. The female gender is more susceptible to functional dyspepsia or patients that smoke and take non-steroidal anti-inflammatory drugs (NSAIDs). Multiple tests such as Computed tomography, Upper endoscopy, and gastric emptying study are conducted to diagnose the condition.

What are the Types of Functional Dyspepsia?
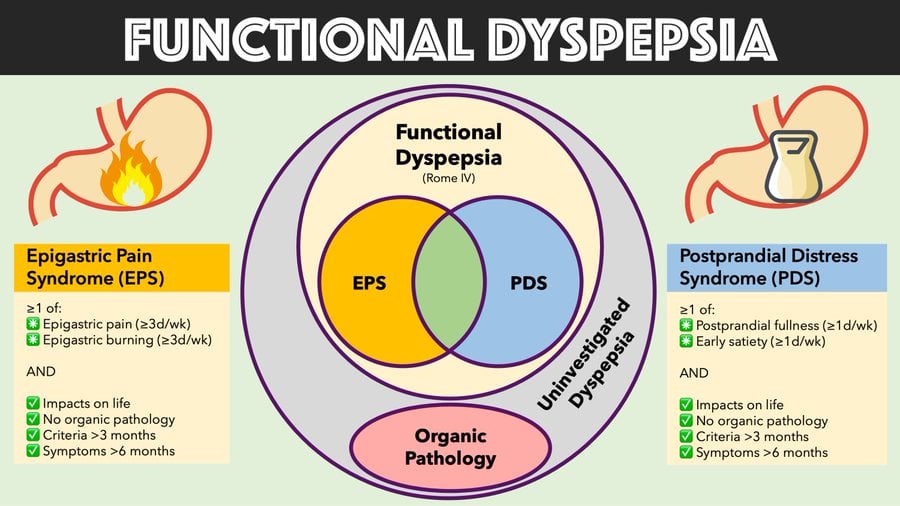
There are two types and they are:
- Epigastric pain syndrome (EPS)- Refers to symptoms associated with upper abdominal pain and burning sensation.
- Postprandial distress syndrome (PDS)- Refers to symptoms that occur after eating, such as early fullness, bloating, and nausea.
Causes
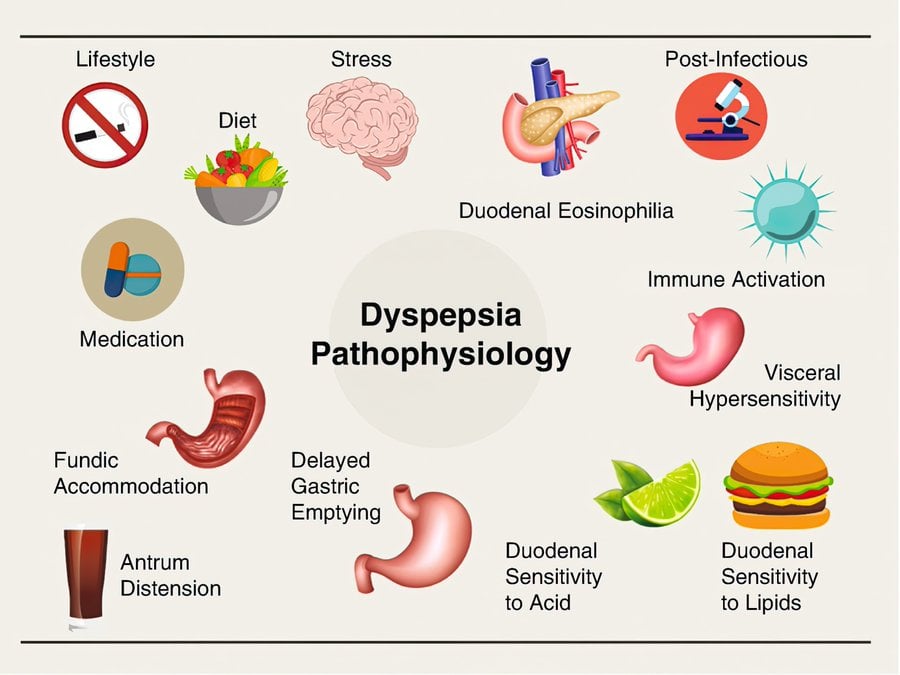
The possible causes of functional dyspepsia are listed below:
- Excess secretion of acid in the digestive tract.
- Allergies.
- Inflammation.
- Smoking.
- Psychological issues.
- Side effects from medications like non-steroidal anti-inflammatory drugs, i.e., aspirin, naproxen, or ibuprofen.
- Infection.
- Obesity.
- Diet.
- Bacteria are known as Helicobacter pylori.
- Lifestyle.
- Disorder in food digestion in the stomach.
- Changes in the microbiome in the intestine.
- Depression.
- Childhood sexual abuse.
What are the risk factors for Functional Dyspepsia?
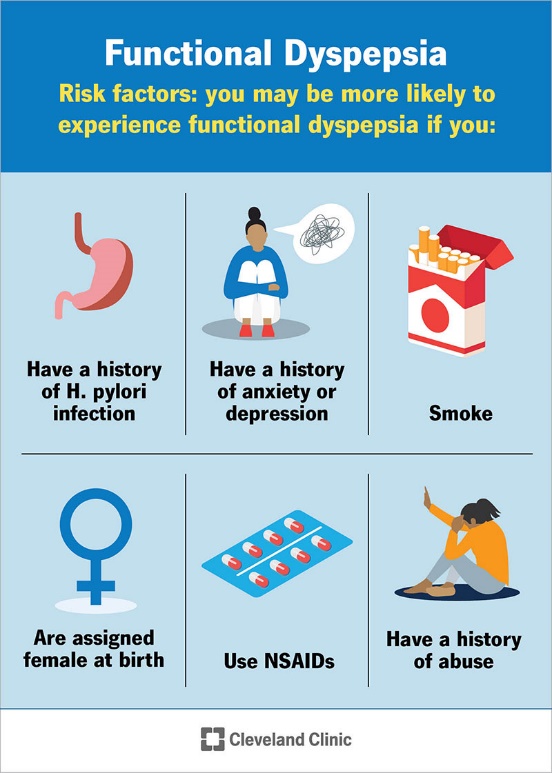
- History of anxiety and depression
- History of H. pylori infection
- Use of NSAIDs
- History of abuse
- History of smoking or tobacco chewing
- Assigned female at birth.
Symptoms
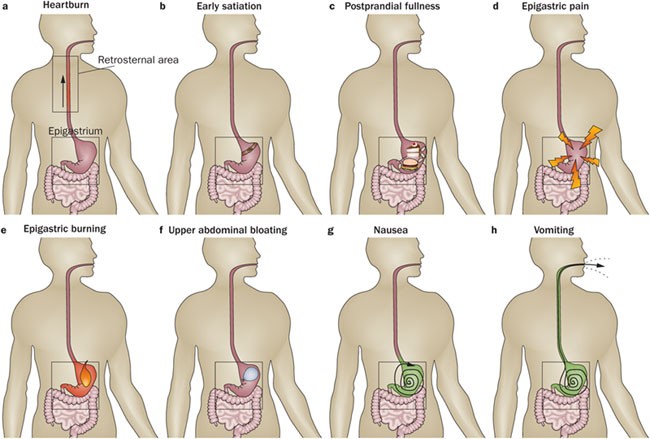
Common symptoms that can be experienced for functional dyspepsia are listed below:
- Immediate satisfaction during a meal.
- Stomach pain.
- Burning sensation in the digestive tract.
- Bloating.
- Belching excessively and nauseous feeling.
Other symptoms that can be experienced that require the immediate attention of medical personnel include:
- Weight loss.
- Vomiting blood.
- Shortage of breath.
- Jaw, neck, or arm pain.
- Tarry and dark stools.
These symptoms need to be persistent, lasting for more than a month before the patient can be diagnosed with functional dyspepsia as it is intermittent.
Diagnosis
Functional dyspepsia is always the last option considered for diagnosis after exterminating all other possible causes of the current symptoms experienced in the patient. Therefore, functional dyspepsia is not initially diagnosed as an indigestion disorder and can be mistaken for various gastrointestinal problems. Possible gastrointestinal problems that can be mistaken for functional dyspepsia are listed below:
- Gastroparesis.
- Abdominal cancer.
- Peptic Ulcer.
- Gastroesophageal Reflux Disease (GERD).
- Irritable Bowel Syndrome (IBS).
The doctor will advise the patient to undergo several tests to confirm the diagnosis. They are listed below:
- X-ray utilizing barium.
- Upper endoscopy.
- Blood tests.
- Test for bacteria.
- Monitoring the pH of the esophageal.
- Urea breath test- To detect H. pylori infection.
How is Functional Dyspepsia treated?
There is no cure available for functional dyspepsia though the symptoms present can be controlled, which will be explained below:
Lifestyle:
Lifestyle might not be directly linked to functional dyspepsia, but it can influence the treatment. Stress is said to affect it indirectly. Therefore, limiting stress to a certain level can influence control over the chronic disorder. Also, managing anxiety can play an important role in the recovery process of indigestion. Frequently consuming little food is preferable to consuming larger amounts at once when diagnosed with functional dyspepsia, which in turn influences weight loss if the patient feels overweight.
Avoiding smoking and drinking alcohol can prove effective in minimizing the disorder. Caffeinated drinks and fatty food should be avoided as they aggravate the symptoms. Placing the head above the body when lying down can aid the management of the symptoms. Six inches of elevation of the mattress is adequate. It should be noted that using a pillow for this elevation is not advisable as the bed frame can also be used as an alternative, as pillows can result in backache and compress the stomach, thereby worsening the symptoms of functional dyspepsia.
Diet:
As stated previously, one should avoid fatty foods. Therefore, changing the patient’s diet might successfully control functional dyspepsia. Eating manners, too, can prompt indigestion. Beverages, citrus, mints, tomatoes, and caffeine can also trigger it. Eating meals in small quantities and resisting high-fat foods may be efficient too.
Psychology:
Controlling the patient’s mental state can effectively manage the disorder as symptoms such as nausea and pain can affect daily activities. A therapy known as hypnotherapy can be used to improve symptoms. Also, other behavioral therapy may prove successful in minimizing the symptoms.
Medication:
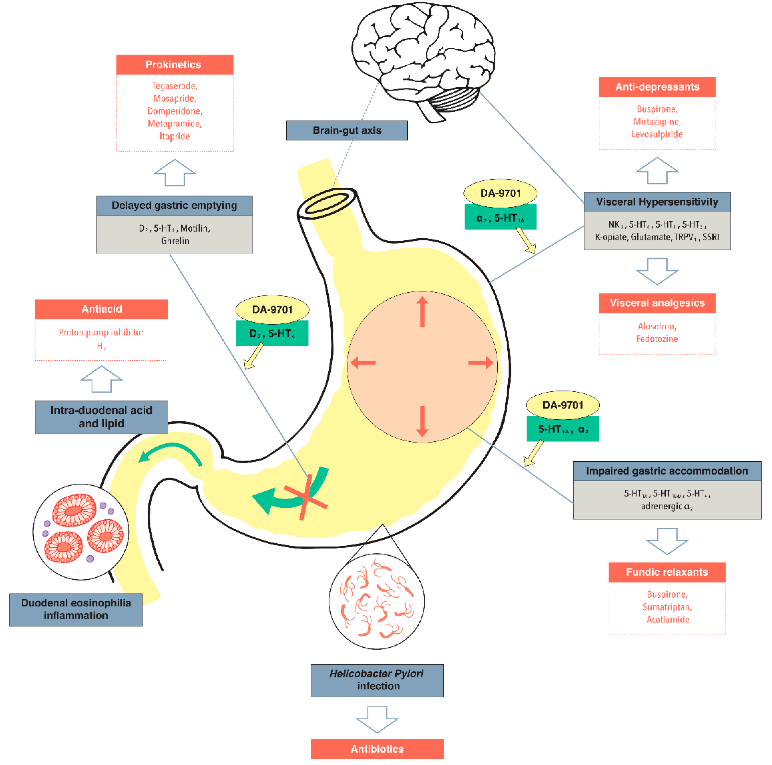
The most common method for minimizing functional dyspepsia is through medication. Two methods are involved in this treatment plan:
Acid Neutralization:
The acid in the upper digestive tract can be neutralized with the aid of a medication known as Gaviscon, which prevents acid migration into the esophagus. Over-the-counter drugs like Pepto-Bismol, Maalox, and tums may reduce symptoms’ effects. Also, antacids can result in temporary or partial ease but can -not stop heartburn from occurring. The secretion of acid can be suppressed by two types of medications which are the “Proton Pump Inhibitors (PPIs)” and “Histamine-2 Receptors Antagonists (H2RAs)”.
Blocking Acid Production:
In this case, the compound responsible for stimulating gastric acid secretion is known as histamine. An allergic reaction triggers histamine. Therefore, the Histamine-2 Receptors Antagonists (H2RAs) are used to create a barrier to null the effect of the histamine. The H2RAs involve medications like Tagamet, axid, Pepcid, and Zantac, and these prescriptions are accessible.
The Proton Pump Inhibitors (PPI) create a barrier to prevent the secretion of enzymes. It is more efficient when the medication is taken without eating, preferably one hour before the first meal. These medications include esomeprazole, omeprazole, pantoprazole magnesium, pantoprazole sodium, lansoprazole, and rabeprazole. PPIs are said to be the most effective for minimizing symptoms, thereby upgrading the quality of the patient’s life. They also affect the esophagus positively and heal sores present.
Also, medications like the domperidone maleate and metoclopramide proffer solutions by modifying the Lower Esophageal Sphincter (LES) to reduce the reflux while the iberogast aids in the regulation of the motility of the digestive tract, thereby controlling symptoms. A combination of methods can also optimize the control of the symptoms of the reflux in the acid.
What is the Recovery Rate and Mortality Rate?
There are no proven recovery rates, nor are there any mortality rates recorded for functional dyspepsia, as the disorder can last a lifetime or intermittently, and there is no cure for this disorder.
FAQ
Functional dyspepsia is liable to anyone of any age. Therefore, children can experience symptoms of this disorder equivalent to that of adults. Still, children are at a disadvantage as they cannot take specific medications required for suppressing the symptoms. In this case, the physician recommends special medications.
Functional dyspepsia has no cause; therefore, it has no specific treatment, but some methods are recommended to minimize the symptoms, such as psychological intervention, lifestyle and diet, and medications.
No further complications are directly involved for patients with possible functional dyspepsia. Also, it cannot lead to cancer in the stomach.
Idiopathic dyspepsia means the exact cause for causing functional dyspepsia is not known.
Functional dyspepsia is an intermittent chronic disorder, meaning the symptoms can come and go. For some patients, it can be there for a lifetime or on and off symptoms, while for some patients, the symptoms disappear completely.
It is considered to be one of the most common functional disorders. It is estimated that about 10-20% of the people who seek medical care for their symptoms have functional dyspepsia.



























































































