Gestational Diabetes Mellitus (GDM)
What is Gestational diabetes? Gestational diabetes mellitus, also called GDM, is a form of diabetes a woman develops during pregnancy. A woman affected by high blood sugar during pregnancy is at a high risk of developing type2 diabetes in the future. Read More
Top Doctors For Gestational Diabetes Mellitus (GDM) Treatments
Top Hospitals For Gestational Diabetes Mellitus (GDM) Treatments
Gestational Diabetes Mellitus (GDM)
Table of contents
What is gestational diabetes mellitus?
Gestational diabetes mellitus, also called GDM, is a form of diabetes a woman develops during pregnancy. A woman affected by high blood sugar during pregnancy is at a high risk of developing type2 diabetes in the future.

Causes
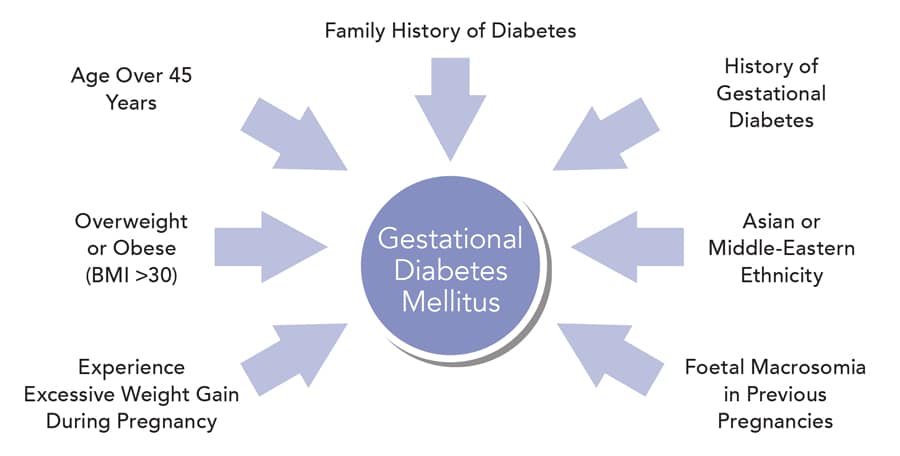
Pregnant women who cannot make enough insulin during late pregnancy may stand the risk of gestational diabetes. Other causes of gestational diabetes may be overweight and genetic transfer.
Symptoms

The symptoms of gestational diabetes include:
- Sugar in the urine
- Unusual thirst
- Excessive hunger
- Fatigue
- Blurred vision
- Vaginal, bladder, and skin infection
How is gestational diabetes mellitus diagnosed?
The following tests can be performed to diagnose gestational diabetes.
- Initial glucose challenge test:
A blood sugar level of 190mg/dl, (10.6mml/l) indicates gestational diabetes. A blood sugar level below 140mg/dl (7.8mml/l) is considered normal.
- Glucose tolerance test (a follow-up test).
How is gestational diabetes mellitus treated?
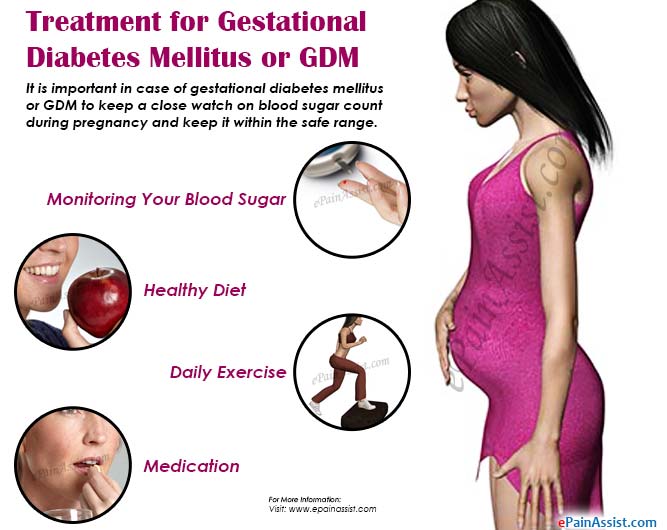
Treatment includes:
- Lifestyle changes: how a pregnant female eats and moves.
- Blood sugar monitoring: by glucose level testing.
- Medication (if necessary): insulin injection, oral drugs.
Life Changes Healthy diets:
The mother is advised to take food that is high in nutrition and fiber and low in fat and calories, such as fruit, vegetables, whole grains, and lean protein. Avoid highly refined carbohydrates, including sweets.
Exercise:
Housework, gardening, walking, and light exercise.
FAQ
Gestational diabetes usually does not occur until late in pregnancy, when the placenta produces more of the hormones that interfere with the mother’s insulin. Screening for diabetes in pregnant women takes place between weeks 24 to 28, but women at high risk are likely to be screened in the first 3months
Symptoms of gestational diabetes, in most cases, are not prominent. Most cases are only detected when the blood sugar level is tested during screening for gestational diabetes.
Gestational diabetes increases the risk of high blood pressure and preeclampsia, a serious complication of pregnancy that causes high blood pressure and other symptoms that can threaten the lives of both mother and baby.
Warning signs of GDM are:
a) Sugar in the urine
b) Unusual thirst
c) Frequent urination
d) Nausea
e) Blurred vision
f) Fatigue
g) Vaginal, bladder, and skin infection.
Best low sugar fruit is:
1) Lemon and limes
2) Raspberry
3) Strawberries
4) Blackberries
5) Kiwis
6) Grapefruit
7) Avocado
8) Watermelon
9) Cantaloupe
10) Orange
11) Peaches
The risk factors associated with GDM are listed below:
1) Being overweight or obese
2) Having prediabetes
3) Race: American Indians, Hispanics, Asian Americans, African
4) Hereditary
5) History of GDM during a previous pregnancy
6) Medical illnesses such as PCOS (polycystic ovarian syndrome) or other health conditions are linked to problems with insulin.
7) Large weight babies (macrosomia)
8) Chances of miscarriage are high.
9) Females who conceive at a late age (>35years)
10) Give birth to babies who are stillborn, dead, or born with birth defects.
The neonatal complications are:
1) Macrosomia (large-size baby)
2) Hypoglycemia which is a low blood sugar level in the baby within a few hours of delivery.
3) Respiratory distress syndrome
4) Early birth of the child (preterm baby)
5) Stillbirth
6) Obesity and type 2 diabetes mellitus later in life. 
Picture Courtesy: slideshare
There is no guarantee when it comes to preventing gestational diabetes. However, there are a few measures that a mother can follow to minimize the risk of developing type 2 DM or having GDM in future pregnancies. They are listed below:
1) Avoid being obese or overweight before pregnancy
2) Maintain a healthy lifestyle and diet plan
3) Exercise regularly
4) Eat healthy food
5) Maintain the weight throughout pregnancy
6) Don’t gain more weight than recommended
The incidence of GDM is becoming high over time due to a lack of maintenance of healthy life or living a poor quality of life. It is estimated that about 7-10% of all pregnancies are affected by GDM worldwide [1].
In most cases, the blood glucose level comes down on its own after delivery. However, 50% of the women diagnosed with GDM might develop type 2 DM later in life. Maintaining a healthy diet and weight and exercising daily can help in decreasing the risk of developing DM in the future.
The recovery period of GDM varies from person to person, their severity, and depends on the type of treatment adopted.
References

























































