Heart Blockage Treatment
Heart blockage is a term used to describe the main problem in coronary artery disease, which is the blood flow restriction to the heart. Coronary artery disease (CAD) is the narrowing or complete obstruction of the coronary arteries, which supply the heart with oxygenated blood. The block is usually caused by a buildup of plaque in these arteries. Read More
Top Doctors For Heart Blockage Treatment Treatments
Top Hospitals For Heart Blockage Treatment Treatments
Heart Blockage Treatment
Table of contents
- What is heart blockage?
- What are the symptoms?
- What are the types of coronary artery disease?
- What causes coronary artery disease?
- What are the risk factors that predispose an individual to coronary artery disease?
- How is coronary heart disease diagnosed?
- What are the therapies for coronary artery disease?
- How can CAD be prevented ?
What is heart blockage?
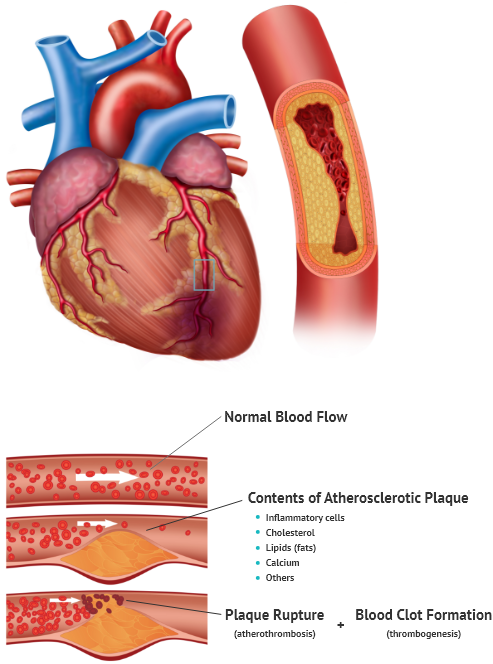
Heart blockage treatment is the same as coronary artery disease treatment. Heart blockage is a term used to describe the main problem in coronary artery disease, which is the blood flow restriction to the heart. Coronary artery disease (CAD) is the narrowing or complete obstruction of the coronary arteries, which supply the heart with oxygenated blood. The block is usually caused by a buildup of plaque in these arteries. Coronary artery disease may exist without causing any noticeable symptoms until the plaque triggers a blood clot in these arteries. This clot blocks the arterial blood flow to the heart; this can trigger a heart attack. This is why CAD is also referred to as the silent killer; it can also be called ischemic heart disease or coronary heart disease.
What are the symptoms?
The symptoms are usually not noticed or might be seen when the heart is put under stressful activities like vigorous exercise. As the coronary arteries narrow, the signs become more apparent due to less blood getting to the heart muscles. Some symptoms include:
- Chest pain – can be experienced as pressure or tightness in the chest. The pain is usually felt on the left side of the center of the chest. The pain can be triggered by physical or emotional stress and usually goes away after some minutes when the stress is removed.
- Breathlessness – this feels like when an individual cannot catch their breath.
- Fatigue and tiredness
- Heart attack – signs of which include chest pain or pressure, arm pain, sweating, and breathlessness.
- Irregular heart rhythm – also known as arrhythmia, is caused by too little blood reaching the heart muscles. This alters the normal signaling of the heart, causing irregular heartbeats.
- Nausea and vomiting
- Feeling lightheaded or dizzy.
- Heart palpitations
What are the types of coronary artery disease?
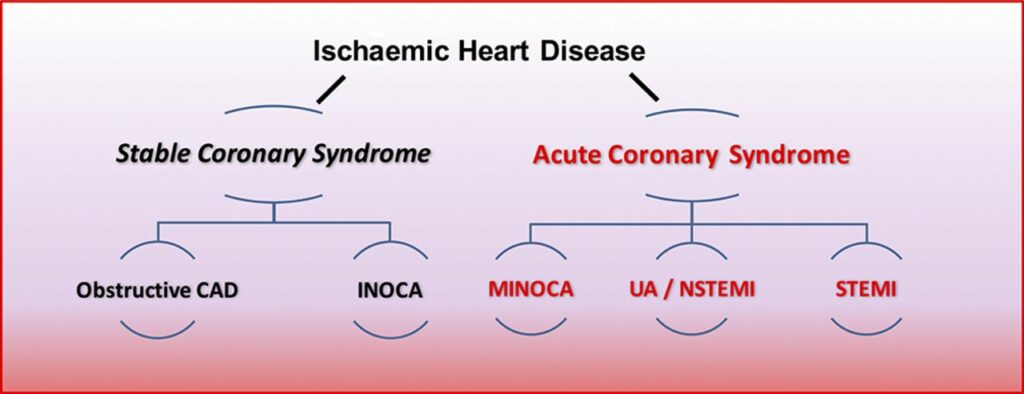
The two main forms that exist include:
- Stable ischemic heart disease – this happens over a long period, and the coronary artery gradually narrows over many years. This leads to the heart getting less and less blood. This form does not present obvious symptoms and can be lived with
- Acute coronary syndrome – this is the sudden form that causes a medical emergency. The plaque buildup ruptures, forming a blood clot that blocks the blood flow to the heart. This blockage causes a heart attack.
What causes coronary artery disease?
It starts with the slow buildup of fats, cholesterol, and other substances in the inner lining of the coronary arteries. This buildup (plaque) narrows the arteries, leading to restricted blood flow to the heart; they can also cause blood clots when rupturing, further blocking the blood supply to the heart. Other causes of damage to the coronary arteries include:
- High blood pressure
- Sedentary lifestyle
- Smoking
- Diabetes
What are the risk factors that predispose an individual to coronary artery disease?
The risk factors include:
- Age– aging increases the risk of damage and restriction to the arteries.
- Sex – men are usually more at risk. The risk for women, however, increases after menopause.
- Genetics – a family history of heart disease makes an individual more likely to get CAD. The risk increases significantly if a father or brother has previously suffered from the disease.
- Smoking – smokers have a high risk of developing CAD. Secondhand smoke also increases an individual’s risk.
- Alcohol – heavy use of alcohol leads to heart muscle damage.
- Unhealthy diet – eating food that has a lot of saturated fat, salt, and processed sugar increases an individual’s risk of developing CAD.
- Diabetes – this increases the risk of CAD, especially type 2 diabetes.
- Unhealthy sleeping habits – getting too little sleep has been linked to an increased risk of heart disease.
- Chronic kidney disease – this increases the risk of CAD.
- High blood pressure can cause the arteries’ stiffness, especially when they are uncontrolled. This causes the narrowing of the affected arteries.
- Obesity – this can lead to diabetes which increases the risk of CAD.
- High cholesterol – too much consumption of low-density lipoprotein and not enough high-density lipoprotein may increase the risk of CAD.
- Stress – stress damages the arteries and worsens the risk factors of CAD.
Risk factors are not mutually exclusive; more than one can occur in an individual. One risk factor may even trigger another.
How is coronary heart disease diagnosed?
When an individual experiences any of the above-mentioned symptoms, it is advised that the person seek medical attention. The doctor will then carry out a thorough physical examination; also, the medical history and lifestyle information are noted. This will provide the doctor with enough information to determine the individual’s risk of the disease. Further tests are then done to get a definite diagnosis, some of which include the following:
- Blood tests
- Cardiac catheterization (standard gold test for diagnosing CAD)
- CT coronary angiogram
- Echocardiogram (echo)
- Electrocardiogram (ECG)
- Exercise stress test
- Coronary calcium scan
What are the therapies for coronary artery disease?
The main therapies for CAD are lifestyle changes, management of risk factors, and medication. The doctor discusses with the individual which treatment plan best suits them. Some individuals require surgery due to the severity of the disease.
Lifestyle changes – this plays a significant role in managing CAD. Some of these changes include:
- Avoiding or quitting smoking and alcoholism
- Exercising
- Healthy diets
Risk factor management – this can help slow down the progression of CAD. Some of the factors that can be managed with the help of a medical practitioner include the following:
- Diabetes
- High blood pressure
- High cholesterol
- Obesity
Medication – there are some medications that help manage the risk factors and also help in the treatment of the symptoms of CAD. The doctor may prescribe any of the following medications:
- Drugs for blood pressure lowering
- Medicines to help lower the cholesterol levels
- Drugs for chest pain
- Treatments to reduce the risk of blood clots
Surgeries – some of the surgeries used to manage CAD include:
- Percutaneous coronary intervention (PCI)
- Coronary artery bypass grafting (CABG)
EECP therapy – stands for enhanced external counterpulsation. It is used to treat chest pain or pressure that does not respond to other treatments. EECP is also used for patients that need blood flow restoration to their heart but is not eligible for surgery. It is a therapy that uses pressure to increase blood flow; it is non-invasive and does not need hospitalization. The treatment is done over seven weeks and reduces the need for medication while improving the individual’s activity levels without experiencing symptoms. It has little or minor side effects.
How does EECP therapy work?
The treatment applies pressure to the blood vessels in the lower limbs, which then increases the blood flow to the heart. This therapy can also encourage the blood vessels to find new pathways to the heart. These new pathways then become natural bypass vessels to help relieve symptoms of CAD.
Who needs EECP?
An individual may be eligible for EECP therapy if they:
- Have long-term chest pain or pressure
- Do not qualify for surgery or other invasive procedures
- Are no longer sensitive to medication
- Experienced reoccurring symptoms after invasive procedures
What is the procedure for EECP?
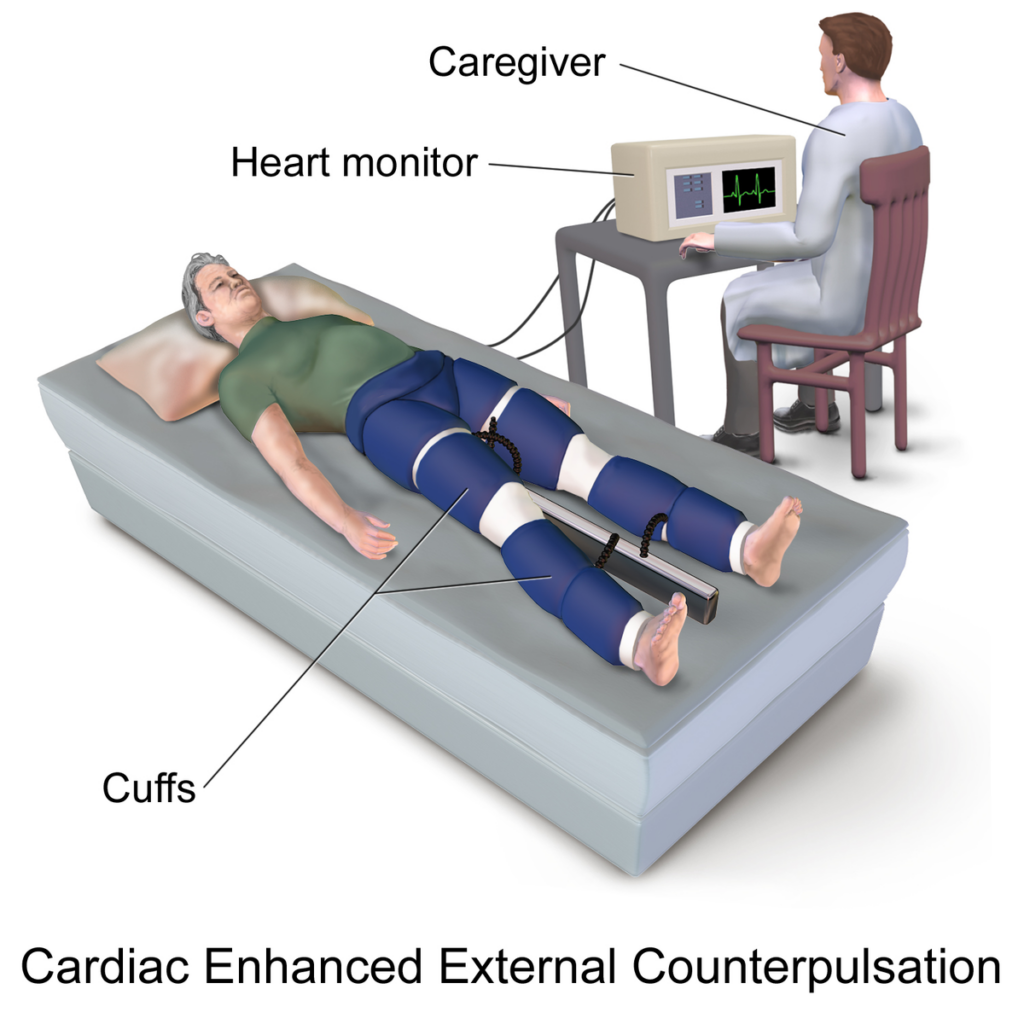
During EECP, the individual is placed on a padded table and told to relax; air-filled cuffs are set around the lower limbs. The cuffs are then inflated, and they tighten around the legs until they reach full treatment pressure. The cuffs inflate when the heart rests, increasing blood supply to the heart through the coronary arteries. Then the cuffs are quickly deflated to lessen the load on the heart. EKG and blood pressure monitors synchronize inflation and deflation with the individual’s heartbeat. This therapy does not cause much pain or discomfort, but it does take some time to get used to it.
How long does EECP last?
It is a therapy that does not require the individual to be hospitalized. EECP is done one hour a day, five days a week, for about seven weeks. It can also be done twice a day for three and a half weeks. An hour session is done, then the individual goes on a break then another session is done. The cumulative time of treatment is usually 35 hours.
How can CAD be prevented?
A healthy lifestyle goes a long way in preventing damage to the coronary arteries, keeping them strong and free of plaques. Some of the health tips include:
- Eating healthy
- Exercising often
- Maintaining a healthy weight
- Reducing stress
- Quitting smoking and alcoholism
- Control of high blood pressure, high cholesterol, and diabetes