Insulinoma
Insulinoma refers to a pancreatic tumor that is caused by beta cells secreting insulin. This condition develops in the neuroendocrine cells of the pancreas and spreads to other parts of the body. Insulinoma, a pancreatic neuroendocrine tumor with unknown causes, has many risk factors. These symptoms/signs can be difficult to spot and may vary depending on severity. Diagnosis is often made through blood tests, and there are several treatment options. Read More
Top Doctors For Insulinoma Treatments
Top Hospitals For Insulinoma Treatments
Insulinoma
Table of contents
What is an Insulinoma?
Insulinoma refers to a pancreatic tumor that is caused by beta cells secreting insulin. This condition develops in the neuroendocrine cells of the pancreas and spreads to other parts of the body. Insulinoma, a pancreatic neuroendocrine tumor with unknown causes, has many risk factors. These symptoms/signs can be difficult to spot and may vary depending on severity. Diagnosis is often made through blood tests, and there are several treatment options.
Insulin is made by the pancreas, which regulates blood sugar levels. Insulin tumors can also produce more insulin than the body can use. The pancreas will stop producing insulin if it detects low blood sugar levels. This allows the blood sugar level to return to normal. But when insulinomas are formed in the pancreas, the tumor continues to produce insulin even when the blood sugar is low, hindering the blood sugar regulation function of the pancreas cells. This condition, therefore, leads to low blood sugar levels–hypoglycemia.
Insulinoma is a rare form of neuroendocrine tumor. Contrary to the characteristics of the tumor, which are mostly malignant, most insulinomas are benign. That is, they grow exclusively at their origin within the pancreas, but the minority is metastasized (spread to other parts of the body).
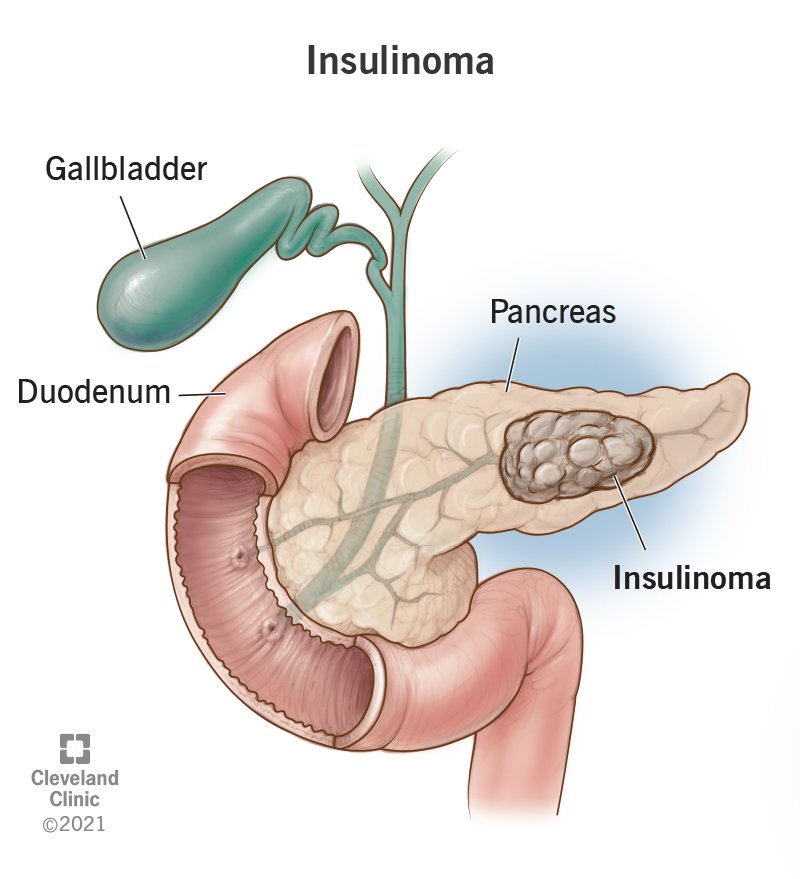
Causes
The exact cause of insulinoma is not known. The tumor typically shows up without warning. However, some factors have been associated with its development.
Such risk factors include:
- Multiple endocrine neoplasia type 1, which is an abnormal tissue growth in the endocrine system
- Von Hippel-Lindau syndrome; is a genetic disease that causes the growth of tumors and cyst all through the body.
- Other generic diseases such as neurofibromatosis type 1, tuberous sclerosis, etc.
Symptoms
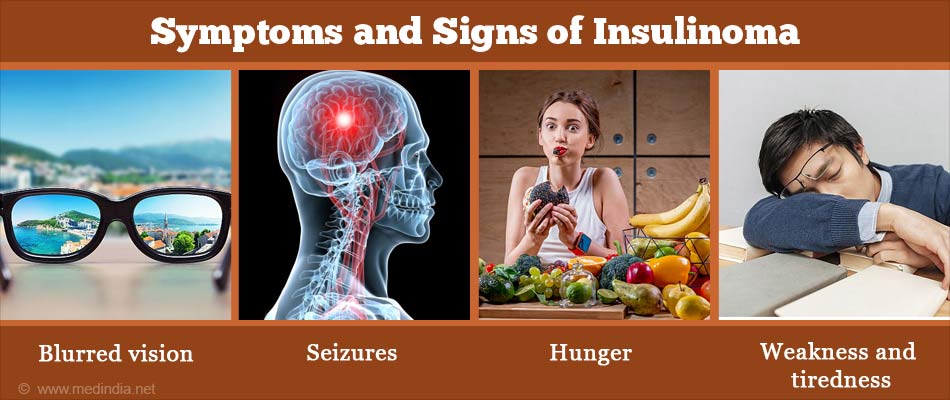
Insulinomas do not often bring up noticeable symptoms, and even when symptoms occur, they vary depending on the severity. More severe symptoms can affect the brain, as well as adrenal glands, which regulate stress response and heart rate.
Signs may include:
- Weakness and fatigue
- Excessive and profuse sweating
- Frequent hunger
- Dizziness
- Back and abdominal pains
- Blurry vision
- Diarrhea
- Seizures and convulsions
- Rapid heart rate
- Jaundice
- Mood changes and swings such as anxiety, depression, fear, etc.
- Non-concentration and confusion
- Loss of consciousness/coma.
How are insulinomas diagnosed?
In order to diagnose insulinomas, the doctor goes through the medical history to check for risk factors and underlying conditions that can cause the development of the tumor.
Tests to perform may include:
- Blood tests through a suppression test
The suppression test is done after a 72-hour fast to see if insulin fails to suppress. If it fails to suppress, it is an indication that there is a presence of an insulin-secreting tumor.
When this is determined, blood is drawn to test for:
- Serum glucose
- Insulin
- C-peptide levels
- Imagery Tests such as:
- Endoscopic ultrasound; to detect tumors in the pancreas–insulinomas.
- CT scans, MRI, and X-rays to view the inside of the pancreas for abnormal growth
- Intraoperative ultrasonography.
- Biopsy: During this procedure, a small sample of the pancreatic tissue is taken through a fine needle and sent for histopathological studies.
- Pancreatic arteriography: During this procedure, a special dye is used to view the arteries of the pancreas.
- Pancreatic venous sampling for insulin: this test is used to locate the exact site of the tumor.
- Selective intra-arterial calcium stimulation (SACS): a highly sensitive method for localization of the tumor [2].
How are insulinomas treated?
Most insulinomas are not cancerous. However, treatments can include the following:
- Surgery
The most preferred treatment for insulinoma is surgery. The position of the tumor is known using diagnostic testing or surgical examination. Insulinomas can be removed through endoscopic, laparoscopic, and other surgical procedures.
- Octreotide/lanreotide Injections to reduce the production of insulin and glucagon.
- Radiofrequency Ablation is a non-surgical, minimally invasive procedure that uses high-frequency radiation to reduce or stop the transmission of pain signals to the brain.
- Embolization Process; a minimally invasive treatment that blocks blood vessels to prevent blood flow to the tumor.
- Liver-directed therapy
- Targeted therapy
- Chemotherapy
- Peptide receptor radionucleotide therapy (PRRT)- During this procedure, the doctor injects drugs into the bloodstream. The drugs combine radioactive atoms and amino acids to target and kill insulinoma cells.
- Enucleation,
- Partial pancreatectomy: during this procedure, a portion of the pancreas is removed where an insulinoma is located.
- Whipple’s surgery, during this procedure, resection of the part of the pancreas along with the gallbladder, near the lymph nodes, and part of the small intestine, stomach, and bile duct is done. Whipple’s surgery is done in case of malignant insulinoma, where the tumor has spread outside the pancreas [1].
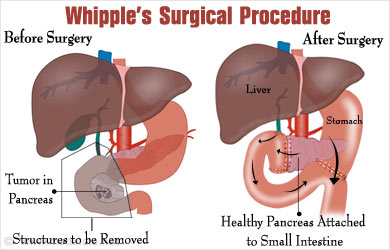
What are the most common complications of insulinoma?
Complications that may occur as a result of the pancreatic tumor/insulinoma include:
- Intestinal obstruction.
- Permanent diabetes mellitus.
- Spread of cancer cells.
- Seizures.
- Coma.
- Death.
Complications that can arise as a result of its treatments include:
- Pancreatic fistula, which is the damage or wound in the pancreas. This can result from the removal of the pancreatic tumor.
- Pseudocyst; a false (usually damaged) cyst that may appear as a cyst on scans but does not have any endothelial or epithelial cells.
- Pancreatic leakage of fluids.
- Abscess; pus collection in body tissues.
- Pancreatitis; pancreas inflammation.
- Hemorrhage
What is the mortality rate of an insulinoma?
A mortality rate of 7.7% has been reported for insulinomas, with a median survival time of 12.7 years.
FAQ
Insulinoma is the most common neuroendocrine tumor of the pancreatic system. It can be seen in every age but is mostly seen in people above 50 years and is more common in women than in men. About 90% of insulinomas are benign (not cancerous) and solitary, and only 10% are malignant (cancerous)
Insulinoma is often diagnosed biochemically using low blood glucose, high insulin, and C-peptide levels. This is done by locating the tumor using medical imaging tests or angiography. For diagnosis, the following blood tests can be performed:
1) Glucose
2) Insulin
3) C-peptide.
Although most islet cell tumors have malignant characteristics, insulinoma is usually benign, with a very low percentage of them being cancerous. Studies state that about 10% of insulinomas are malignant.
Insulinoma is a rare pancreatic endocrine tumor whose incidence is rated to occur in about 3 to 10 cases per a million people per year. This makes up 55% of neuroendocrine tumors.
The majority of insulinoma patients have not inherited the condition. According to the study, for 1 in every 14 patients, insulinoma may be part of an inherited syndrome called multiple endocrine neoplasia type 1.
In a bid to stop blood sugar levels from falling, glucagon is released. Low blood glucose, high-quality protein, adrenaline stimulate the release of glucagon. However, insulin is released when blood sugar levels rise to lower them.
If the blood sugar level drops below 20mg/dL, then the patient may lose consciousness and go into a coma.
If the patient has symptoms of severe low blood sugar (dizziness, excessive sweating, blurred vision, confusion, mood swings, seizures, etc.), seek immediate medical care.
There are no known ways where insulinomas can be prevented. However, one can reduce the risk of developing hypoglycemia by exercising regularly, maintaining a healthy diet, quit drinking and smoking. The diet should consist of fruits, green leafy vegetables, and lean proteins.
The incidence of insulinomas is approximately seen in 4 in 1 million population. It is most commonly seen in people around 40-50years of age.
References
- https://my.clevelandclinic.org/health/diseases/22217-insulinoma
- https://www.medindia.net/patientinfo/insulinoma.htm

























































