Lung Transplant
A lung transplant, or ‘pulmonary transplant’, is a surgical process of replacing a non-functioning or diseased lung(s) with the healthy ones of a donor. The donor can either be deceased or living, depending on the type of transplant needed for the patient. Read More
Top Doctors For Lung Transplant Treatments
Top Hospitals For Lung Transplant Treatments
Lung Transplant
What is a lung transplant?
A lung transplant, or ‘pulmonary transplant’, is a surgical process of replacing a non-functioning or diseased lung(s) with the healthy ones of a donor. The donor can either be deceased or living, depending on the type of transplant needed for the patient. Lung transplantation can be done for people of all ages, infants, children, and adults up to 65years old. Transplantation of the lung can be either unilateral or bilateral.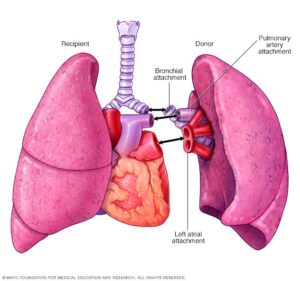
What are the types of Lung transplants?
Types of Lung Transplant Procedures Picture Courtesy: Myupchar
Picture Courtesy: Myupchar
- Unilateral (Single) Lung Transplant; the transplant of one lung.
- Bilateral (double) transplant- transplantation of both the lungsBilateral sequential Lung Transplant- Transplantation of both the lungs, but one lung at a time. It is also called a bilateral single transplant.
- Heart-Lung Transplant; the transplant of both lungs and the heart but from a single donor.
Lung Transplant Preparation and Procedures
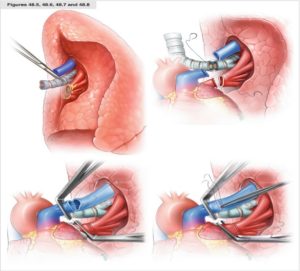 Picture Courtesy: Springer
Before the surgery, as a part of the pre-operative assessment, a patient should undergo a couple of medical tests to ensure that patient is fit for the procedure or not. These tests include blood tests, heart function tests, CT scans of the lungs, pulmonary function tests, angiogram (a type of test that checks the blood flow in the lung’s blood vessels), psychological and social evaluation, etc. [6]. Once the pre-op assessment has been done and the patient is fit for the procedure, the patient will be placed on a waiting list to get a matching donor.
This is why your life expectancy should not be less than a year. Your duration on the waiting list will depend on:
Picture Courtesy: Springer
Before the surgery, as a part of the pre-operative assessment, a patient should undergo a couple of medical tests to ensure that patient is fit for the procedure or not. These tests include blood tests, heart function tests, CT scans of the lungs, pulmonary function tests, angiogram (a type of test that checks the blood flow in the lung’s blood vessels), psychological and social evaluation, etc. [6]. Once the pre-op assessment has been done and the patient is fit for the procedure, the patient will be placed on a waiting list to get a matching donor.
This is why your life expectancy should not be less than a year. Your duration on the waiting list will depend on:
- Availability of a matching lung
- Blood group and genotype
- The size of the donor’s lung
- The geographic distance between donor and recipient
- The severity of the patient’s condition
- The patient has to consult the surgeon.
- The surgeon will counsel the patient regarding the approach to the surgery, risk factors related to procedures, post-operative measurements, duration of stay in the hospital, etc.
- Undergo laboratory and imaging tests to ascertain the state.
- Do not eat or drink anything.
- Take an antimicrobial shower.
- Run a basic testing
- Sign consent forms for the surgery
- See the anesthesiologist.
- Get prepped in the surgery room.
- Once prepped in the operation room, the steps follow accordingly:
- The doctor will insert an IV line on the arm, wrist, or neck area to provide iv fluids or give pain killers or antibiotics. An anesthetist will administer general anesthesia (patient remains unconscious throughout the procedure). A tube will be inserted into the patient’s windpipe and is connected to the breathing machine (ventilator), which helps to breathe. A urinary catheter is placed in the bladder to drain urine and empty the bladder. The patient’s heart rate, blood pressure, and breathing will be monitored carefully throughout the procedure [6].
- The patient will be placed on a heart-lung machine to help the patient pump and oxygenate the blood.
- A large incision will be made on the chest, and through this incision, the old lungs will be removed and replaced by the new lungs.
- The donor (new) lung(s) will be connected to the recipient’s airway and blood vessels. In case of a bilateral sequential transplant, the lungs will be attached one at a time.
- The incision will be closed and sutured back in place when the new lung begins working properly.
- One or more tubes will be placed in the chest to remove the fluids, blood, air from the chest and allow the donor’s lung to expand completely.
- To recover, the patient will be moved to the Intensive Care Unit (ICU).
Lung Transplant Recovery
Post-surgery the patient will be kept in ICU for close monitoring and care. Lung transplantation recovery is a steady but progressive healing process. Patients are taken off the ventilator within 24 hours of the surgery’s completion, provided there are no other complications noticed and constant surveillance is done. On waking up, the pain from the incision will be taken care of by giving pain killers through the epidural catheter. The patient is placed on immunosuppressive medications to prevent the newly transplanted lung from rejecting the patient’s immunity system. Patients at this time are advised to eat healthily. They are advised to do some deep breathing exercises, which will help them recover early from anesthesia and improve their breathing ability of the lungs. The physiotherapist will teach them to follow some exercises that will help in regaining the body’s strength. The doctor prescribes a couple of tests and frequently monitors the state of the heart and lungs. Avoid stress and exertion on the heart and lungs and get enough hours of rest. After an average of 14 to 21 days of stability, the patient will be discharged. Still, the patient is advised to take complete rest for another 3-4 weeks before returning to his daily routine activities. Here are a few of the instructions patient needs to follow strictly after going home. Take medications as prescribed.- Maintain recommended breathing exercises.
- Eat healthy diets.
- Regularly visit the doctor for follow-up.
- Patients should not neglect even a minor symptom. Post-operative blood tests and other tests should be done regularly, and consult the doctor for further care. Avoid people with infections.
What are the possible complications of a lung transplant?
The major complication of a lung transplant is when the immune system begins to think donor lung as an antigen and attacks. This is called ‘organ rejection. However, ‘immunosuppressants’ have aided in lessening this risk. Other complications may include:- Blocked blood vessels leading to the new lung(s)
- Airways blockage
- Bronchiolitis Obliterans Syndrome is another type of rejection that occurs during 1st month after the transplant.
- Post-transplantation lymphoproliferative disorder [6].
- Severe pulmonary edema (fluid in the lung)
- Blood clots
- Bleeding
- Infection
- The patient should have a life expectancy of 1-2 years without a transplant.
- If older than 65 years, the patient should have no other life-threatening disease for a lung transplant to be considered.
- The patient should have been cancer-free for at least 5 months.
- The patient should have no record of alcohol and drug abuse.
- Patient should be free of any infection and systematic diseases.
- The patient should have stopped smoking for more than 6 months.
Causes
The causes for lung transplants are often related to diseases and conditions that damage the lungs making them unable to function normally. When there is damage to your lungs, your ability to breathe in order to survive becomes limited, and slowly you can lose your life. In such cases where they can no longer be helped with medications, therapies, and breathing devices can no longer help, and the situation becomes life-threatening, a lung transparent is required to save the patient's life.
Lung transplantation has therefore been considered as optimal therapy for multiple causes of end-stage pulmonary disease. Some of these severe end-stage diseases include:
- Bronchopulmonary dysplasia
- Chronic obstructive pulmonary disease (COPD); Emphysema, Chronic bronchitis, etc.
- Idiopathic pulmonary fibrosis
- Pulmonary fibrosis; scarring of the lungs.
- Idiopathic pulmonary arterial hypertension/Pulmonary hypertension; high blood pressure in the lungs
- Interstitial lung disease (ILD)
- Cystic fibrosis
- Histiocytosis
- Bronchiectasis
- Lymphangioleiomyomatosis
- An inoperable tumor in the lung
- Coronary artery disease, where a procedure to restore blood flow to a blocked or narrowed artery in the heart, in addition to a lung transplant. A heart-lung transplant is needed in these cases.
FAQ
1. How long do I have to stay on a waiting list to get a donor?
The duration of waiting to get a donor cannot be determined by anyone. For chronic pulmonary diseases that need immediacy, it may take lesser time. However, it could range anywhere from a few days to several years.
2. What is the average age for a lung transplant?
The average age ranges from 2 to 65 years.
3. How long can a patient live after a lung transplant?
One cannot estimate the exact duration after a lung transplant because the life expectancy post-transplantation varies from person to person. According to the British transplantation society, it is estimated that around 9 out 10 people survive for at least a year after the transplantation. About 5 out of 10 people survive for at least 5 years. There have also been reports that patients after lung transplant live for more than 20years.
4. What is a double lung transplant from vaping?
Vaping is the act of smoking e-cigarettes. They are highly inflammatory and dangerous for the lungs. Over time, the accumulation of smoke in the lungs damages them beyond repair, causing a need for a double-lung transplant.
5. How do I get rid of lung transplant incision scars?
Although the scar can be an ugly reminder of what the patient has been through, it takes time to clear off. It will fade away with time. Just moisturize and keep it clean of every infection.
6. Are lung transplants dangerous?
Every surgery has its risks. A lung transplant is considered a complex surgery with pros and cons. The primary risk factor for this surgery is organ rejection. Other significant risk factors include bleeding, blockage of the airway, accumulation of fluid in the lung, etc. [2].
7. Is lung transplant a cure for cystic fibrosis?
Cystic fibrosis is a genetic disease that causes the accumulation of mucus in the lungs. Over some time, it causes recurrent inflammation and infection of the lungs, which results in permanent damage to the lungs. Lung transplantation can be a treatment option for cystic fibrosis [3].
8. can lung transplant patients drink alcohol?
Lung transplant patients are always advised to follow a healthy lifestyle and avoid drinking alcohol and smoking to prevent post-operative complications.
9. What is a breathing lung transplant?
‘Breathing lung’ technology is an experimental lung transplant organ-preservation system. The organ care system helps the donor’s lungs function outside the body while the lungs are being transported. The OCS helps to maintain lung health by keeping them in an environment similar to inside the body (warm and nourished by blood and oxygen) [4].
References
- https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/lung-transplant
- https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/lung-transplant
- https://www.healthline.com/health/cystic-fibrosis-lung-transplant
- https://www.uclahealth.org/transplants/lung/breathing-lung-transplant
- https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/lung-transplant
- https://www.myupchar.com/en/surgery/lung-transplant
- https://www.nhs.uk/conditions/lung-transplant/risks/

































