Migraine Operation
A migraine is not just an ordinary headache, it is a common primary neurologic headache that causes painful headache attacks mostly in working-class adults. Migraines can be acute or chronic, and they usually come with symptoms like nausea, vomiting, photophobia, etc. Read More
Top Doctors For Migraine Operation Treatments
Top Hospitals For Migraine Operation Treatments
Migraine Operation
Table of contents
What is a Migraine?
You might be surprised to learn there is such a thing as a migraine operation. First, it is essential to know that not all headaches are migraines, and this brings to mind the question, “what is a migraine?”
A migraine is not just an ordinary headache, it is a common primary neurologic headache that causes painful headache attacks mostly in working-class adults. Migraines can be acute or chronic, and they usually come with symptoms like nausea, vomiting, photophobia, etc.

Generally, when an individual has been diagnosed with migraines, several treatment options are recommended. Such treatment options include prescribed medicine, dietary changes, and lifestyle changes. Surgery is usually recommended by healthcare professionals if the individual does not respond to other treatments.
Occurrence and Location of Migraines
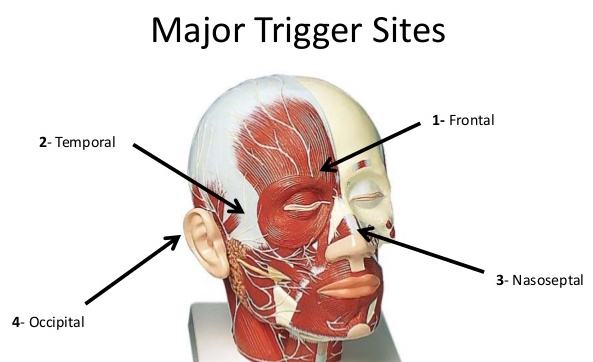
Migraines can occur due to the compression or irritation of the sensory nerves and vessels in an individual’s head at sites called trigger points. These trigger points can be activated by factors such as loud noise, hunger, or bright light.
Trigger Points of Migraines
The trigger point of one individual may vary from that of another depending on the symptoms experienced. An individual may also have more than one trigger point. Types of trigger points are:
- frontal region (on the forehead, above the eyebrows)
- occipital region (at the back of the head)
- temporal region (on the temple)
- rhinogenic region (inside the nose and runs to the back of the eyes)
A migraine operation is performed to mitigate or eliminate headaches’ occurrence, pain, and duration. An operation for migraine is targeted at releasing compression points of the sensory nerves and vessels, resulting in the reduction or a complete end to the migraines. This can be done by getting rid of very small sections of tissues or bones that may be compressing the nerves. Also, the nerves may be cut.
Requirements to be eligible for a migraine operation
The candidate must have:
- been diagnosed with migraines or occipital neuralgia,
- been unsuccessful with therapies such as behavioral and medications,
- realistic expectations, and
- good physical health.
Before a migraine surgery is conducted, the patient has to be examined by the surgeon during a consultation period. During the consultation, the following will be done.
- The patient’s medical history.
- A thorough physical examination focused on the symptoms of the migraines and the involvement of potential peripheral nerve pathology.
- Diagnostic testing is done to determine if peripheral nerve pathology is a cause of the migraines.
What to do before a migraine operation
- A medical evaluation is to be conducted
- Certain medications will be prescribed to be used by the patient
- If the patient smokes, they will be asked to quit smoking
- The patient is advised to stop taking anti-inflammatory drugs, aspirin, and herbal supplements.
Types of Migraine Operation
There are several types of migraine surgery depending on the area the surgeon is targeting.
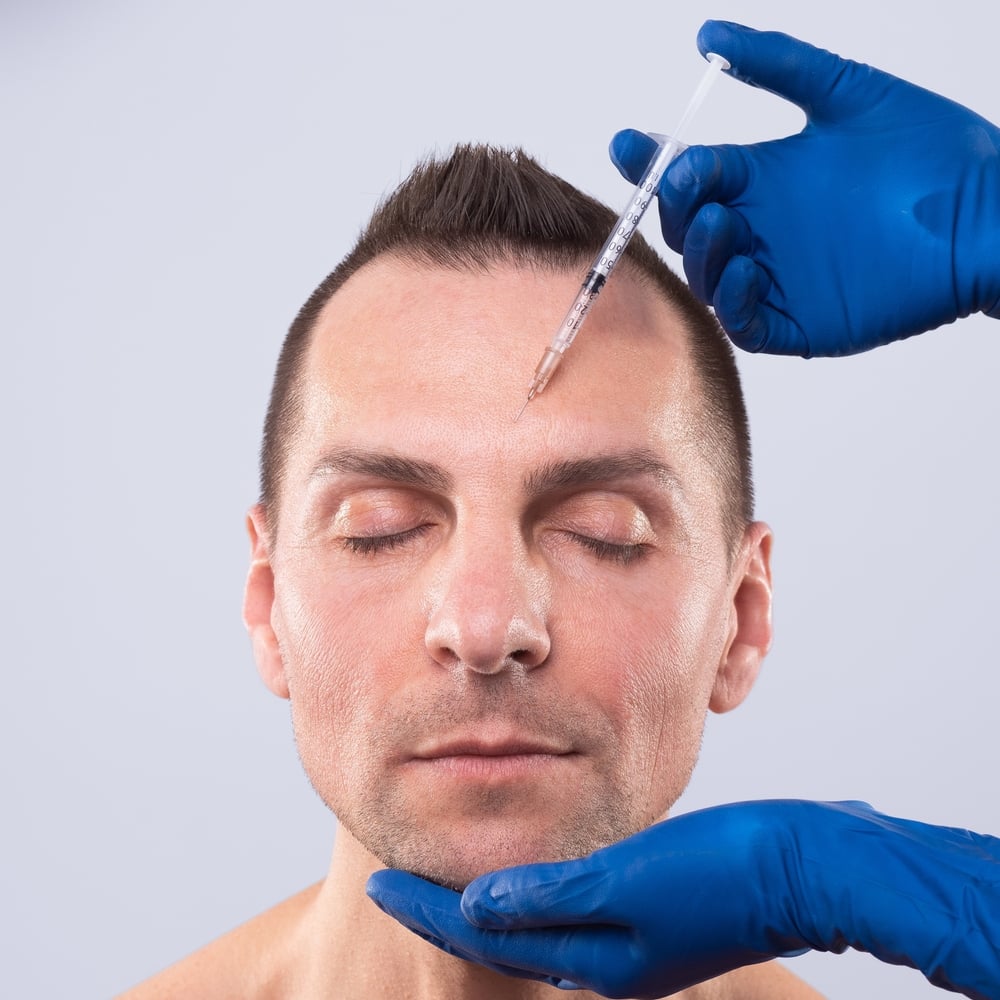
Botox for Migraines
Botox for migraines can be used as a form of treatment for migraines mostly in adults. This can not only be used to identify the trigger points but it can also be used to provide temporal relief. Thus, it is not a one-time treatment.
Peripheral Neurolysis
This is a procedure aimed at relieving pressure on the nerve. It is targeted at the nerves that cause migraines. It can be in the form of nerve decompression or nerve liberation.
The procedure involves removing from the face, neck, or head, a small fraction of the tissue or bone compressing the nerve. Afterward, the area is filled with fat to prevent future compression. The procedure could be done by completely removing the nerve covering its ends in muscles nearby.
Neuromodulation
This procedure explores the act of stimulating migraine-triggering nerves with electromagnetic pulses. To help treat migraines, external neuromodulating devices that pass electromagnetic pulses to the skin have been approved by the Food and Drug Administration (FDA). Although uncertain about how safe and effective it is, neuromodulators can be implanted beneath the skin to conduct a migraine operation. However, these devices are not for everyone.
Septoplasty
This is a procedure that involves surgically correcting a deviated septum. A deviated septum can be described as when the septum (the wall that separates the nostrils) tilts to one side, thereby resisting airflow. This can lead to migraines. The purpose of septoplasty is to adjust the septum in a way that opens up the airways and reliefs the individual of pain. However, a successful septoplasty does not guarantee that the individual is migraine-free.
Turbinectomy
A turbinectomy is a surgical procedure that involves removing the small bones (turbinates or conchae) located within the nose. The air that goes to the lungs is cleaned, humidified, and warmed by the turbinates in the nostrils. The severity and occurrence of migraines may decline after a turbinectomy but there is not enough substantial research to support this. In some cases, individuals still battle a relapse of migraines after the operation.
Migraine Operation Procedure
Before the start of the operation, the patient’s trigger point is first identified. Afterward, the surgeon will place the patient on anesthesia.
Next, the surgeon will make an incision at the trigger point’s location. The major trigger points have specific locations where a surgeon can decide to make an incision but for uncommon trigger points, the incision can be done at different areas. If the trigger point is located in the frontal region, the incision made will be done using either of the following.
- Endoscopic approach – It involves making 3-5 small incisions above the forehead, along the hairline.
- Open approach – The migraine operation will be done by incising the eyelid’s crease.
An endoscopic approach is performed at the temporal trigger point by making two small incisions in the temple’s hair-bearing part. If both the temporal and frontal regions are addressed simultaneously, then the surgeon will incise the crease of the upper eyelid.
When the trigger point is located at the occipital region, an incision is made across the back of the skull, horizontally or vertically. The scalp’s hair-bearing region is where both kinds of incisions are made.
At the rhinogenic region, the surgeon makes incisions on a more individualized level. The intranasal findings of the patient determine this. Finally, the surgeon will close the incision by using sutures, skin adhesives, tapes, or clips.
After the surgery
- The patient may either go or stay overnight at the hospital depending on the outcome.
- Likely, the patient may experience some normal discomfort.
- The doctor will prescribe appropriate medications to be taken post-operation.
- Specific instructions will be given to the patient to help with healing.
- Follow-up visits will be scheduled for checkups.
A reduction or complete elimination of migraines has been reported in about 70%-95% of patients who undergo a migraine operation. Improvement may be immediate, or it may take weeks or months before the effect occurs. However, there are cases where an individual may need to undergo another surgery to achieve optimal results.
Individuals may experience one of the following after surgery and are advised to see their doctor immediately.
- Pain at another location different from the trigger site operated on during surgery.
- Shortness of breath
- Chest pains, etc.
Side Effects of a Migraine Operation
A migraine operation may lead to one or more side effects. An individual needs to be enlightened about the risks associated with migraine surgery. Afterward, the individual will be asked to sign a consent form confirming that the procedure has been well understood. The side effects or risks associated with a migraine operation include:
- Infection
- Hematoma
- Persistent pain
- Risks of anesthesia
- Fluid accumulation
- Bleeding
- Itching
- Tingling
- Numbing feeling
- Skin discoloration
- Visible scarring
- Prolonged healing of incisions
In cases where a septoplasty or turbinectomy was performed, an individual could suffer from a damaged septum or a change in the sense of smell. An individual who underwent a neuromodulation transplant is at risk of having the wires o the neuromodulator break apart from the targeted nerve.
Summary
Finally, several neurologists and headache specialists are yet to confirm the migraine surgery success rate. This is because they consider it to be in its experimental stage. However, people who are considered to be eligible for a migraine operation should ensure they know how experienced their surgeon is. If done successfully, an individual will get relief from the migraines.
FAQ
The cost of a migraine operation can vary as it is determined by several factors. These factors include:
1) the experience of the surgeon,
2) geographic location,
3) the number of nerves being looked at, etc.
Migraine surgery can take 1 – 4 hours. However, this depends on the number of trigger points a patient has.




































![DR [PROF.] KARL MILLER](https://anavara.com/wp-content/uploads/2021/10/DR-PROF.-KARL-MILLER-244x300.jpg)