Type 1 Diabetes In Children
Type 1 diabetes in children is a medical disorder characterized by the inability of the child’s body to no longer produce a vital hormone known as insulin. Every child needs the insulin hormone to survive, so the missing insulin will need to be replaced with injections or an insulin pump. Type 1 diabetes in children is also known as juvenile diabetes or insulin-dependent diabetes. Read More
Top Doctors For Type 1 Diabetes In Children Treatments
Top Hospitals For Type 1 Diabetes In Children Treatments
Type 1 Diabetes In Children
Table of contents
What is Type 1 Diabetes in Children?
Type 1 diabetes in children is a medical disorder characterized by the inability of the child’s body to no longer produce a vital hormone known as insulin. Every child needs the insulin hormone to survive, so the missing insulin will need to be replaced with injections or an insulin pump. Type 1 diabetes in children is also known as juvenile diabetes or insulin-dependent diabetes.
Diagnosing and managing type 1 diabetes in children can be overwhelming, particularly in the beginning. All of a sudden, the parents and the child, irrespective of age, will have to learn how to give injections, count carbohydrates, and monitor blood sugar levels.
Unfortunately, there’s no cure for type 1 diabetes in children. However, it can be managed, and the several advances that have been made in blood sugar monitoring and insulin delivery have helped improve blood sugar management and improve quality of life for children with type 1 diabetes.

Understanding Type 1 Diabetes
It should be known that type 1 diabetes is an autoimmune disorder. It develops when the pancreas can no longer produce insulin due to attacks from the immune system on the cells that produce insulin, which leads to their destruction. Insulin is an essential hormone in the body, and it’s needed to let glucose (blood sugar) move from the bloodstream into the body’s cells, which can be used for energy or stored for later use.
In the absence of insulin, glucose cannot enter the body cells to do its work, and as a result, it continues to stay in the bloodstream. This leads to high blood sugar levels, which in turn leads to diabetes.
What is the classification of type 1 diabetes in children?
Type 1 diabetes in children can be in various forms, which give rise to different classes of the disease. The is outlined as follows
- Preclinical β-cell autoimmunity,
- The onset of clinical diabetes,
- Transient remission, and
- Established diabetes.
Causes
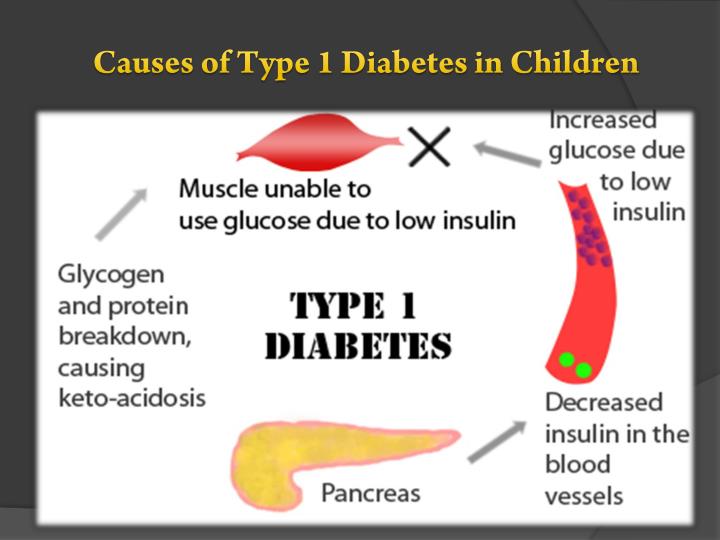
The actual causes of type 1 diabetes in children and in general are unknown. What is known is that it is an autoimmune disease. That is, the body’s immune system, which usually protects the body against foreign bodies such as harmful bacteria and viruses, mistakenly attacks and destroys the insulin-producing cells in the pancreas. This process could be aided by genetics and environmental factors.
Once the pancreas’s insulin-producing cells are destroyed, the child’s body produces little or no insulin, which performs the critical job of moving blood sugar from the bloodstream to the necessary body cells. Without sufficient insulin, the sugar produced builds up in the child’s bloodstream and can cause life-threatening complications if left untreated.
Symptoms
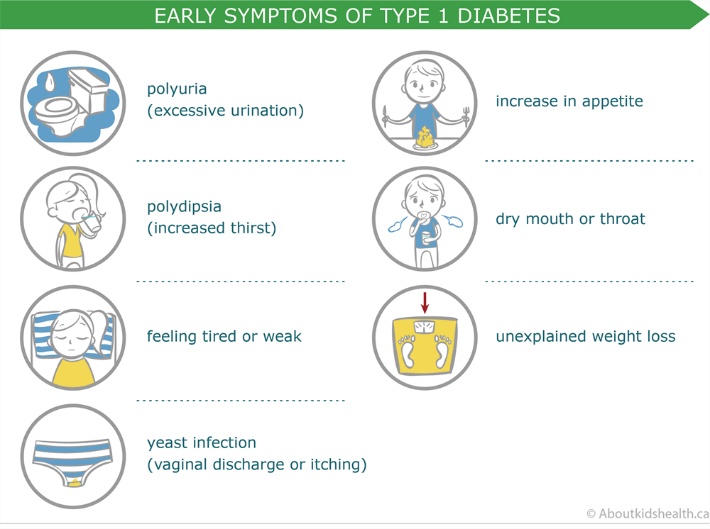
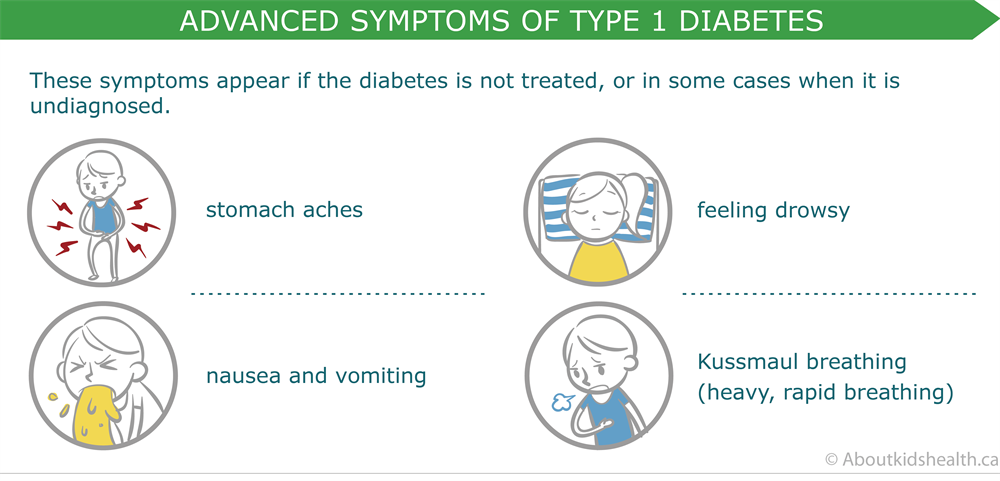
The symptoms of type 1 diabetes in children usually develop quickly and may include
- An increased thirst
- Frequent urination and possible bed-wetting in a toilet-trained child
- Extreme hunger
- Vision changes from clear to blurry.
- Sudden and unexplained weight loss
- Fatigue and tiredness
- Behavioral changes such as irritability, restlessness, or moodiness.
- A fruity-smelling breath.
- Poor wound healing.
- Abdominal pain.
How is juvenile diabetes diagnosed?

In order to diagnose juvenile diabetes, a child must have fulfilled the general diagnostic criteria for diabetes, which require the identification of any of the following signs and symptoms of type 1 diabetes in children like polyuria, polydipsia, and poor weight gain with regular or minimally changed feeding pattern.
Some of the following investigations are carried out to diagnose juvenile diabetes. They are listed below:
- Random blood sugar level analysis: This requires no fasting. The blood sample can be drawn at any time during the day, and blood glucose levels can be measured. If the blood glucose levels estimate at a value ≥ 200 mg/dL (or 11.1 mmol/L) and the symptoms of type 1 diabetes in children are present, diabetes may be confirmed.
- A fasting blood sugar level analysis: This requires overnight fasting for 8 hours. If the blood glucose levels estimate at a value ≥ 126 mg/dL (or 7.0 mmol/L), and the symptoms of type 1 diabetes in children are already seen, then diabetes is confirmed.
- Measurement of glycated hemoglobin (A1C) in the blood: That is, measuring the hemoglobin that has glucose attached to it. If the results show a value ≥ 6.5%, then a diagnosis of juvenile diabetes may be confirmed.
After diagnosing juvenile diabetes, it may be necessary to conduct other tests to differentiate the type of juvenile diabetes diagnosed.
- A screening for islet (insulin-producing) cell antibodies and glutamate decarboxylase antibodies may be conducted. The presence of islet autoantibodies shows the body has an immune system response to the islet cells in the pancreas that produce insulin. While these autoantibodies are not necessarily among the causes of type 1 diabetes in children, they have been identified to be a positive marker for the condition.
- Urinalysis test for the detection of ketones which are more common in type I diabetes, is done.
- A renal function analysis is to know the kidney’s health status, rule out renal failure, and achieve a baseline state before the commencement of treatment.
- An oral glucose tolerance test to distinguish type I diabetes from maturity-onset diabetes of the young and hyperglycemia.
How is type 1 diabetes in children treated?
The most vital intervention in managing and treating type 1 juvenile diabetes is the option of insulin therapy since there is no longer an endogenous production of insulin. These commercial insulins are of different types (rapid-acting, long-acting, immediate-acting, and regular, short-acting insulin), and they differ in how swiftly they work and how lasting their effects are. The doctor will, however, guide the parents on the right combination of insulin for their child.
However, insulin therapy is best administeredin conjunction with other supportive measures to maximize the impact of the exogenous insulin with minimum doses. Such measures include:
- Diabetic Education and counseling of the parents or caregivers of the child to ensure strict adherence to insulin and to circumvent the psychological effects of any behavioral changes.
- Intake of low-fat, high-fiber food and dietary modifications.
- Regular exercises help avoid the development of insulin resistance and trigger weight loss.
Regular glucose monitoring:
This helps to detect an onset of complications, which helps to make an early intervention.
FAQ
Nothing is presently known about how to prevent type 1 diabetes in children.
While there’s nothing the parents can do to prevent type 1 diabetes in their child, however, one can prevent their child from its complications by:
1) Helping them maintain good blood sugar control as much as possible.
2) Teaching their child the importance of eating a healthy diet and engaging in regular physical activity.
3) Paying regular visits to their child’s diabetes doctor and conducting a yearly eye examination beginning after the initial diabetes diagnosis. 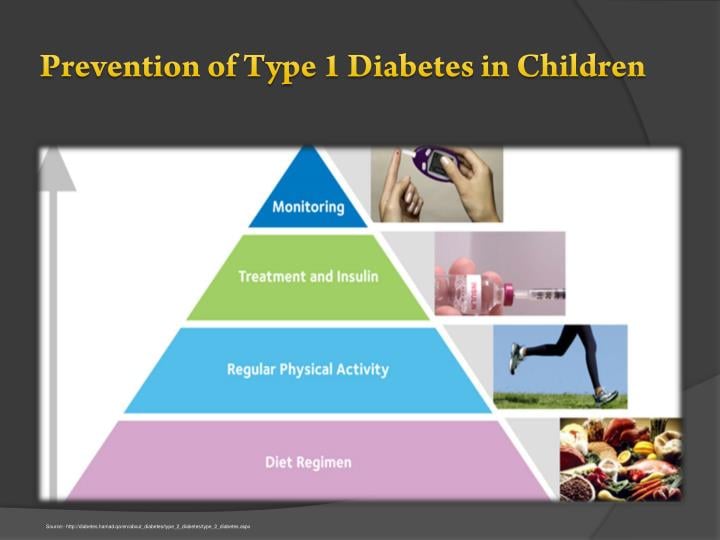
Picture Courtesy: slideserve
Diet is essential for any person with diabetes, particularly juvenile diabetes. Therefore, children with juvenile diabetes must eat a balanced and healthy diet high in complex carbohydrates and fiber.
However, a dietician will provide the parents with the necessary advice on their child’s diet. 
Picture Courtesy: healthybabies
Exercise is the second most important factor in managing diabetes. It is highly recommended that children with diabetes exercise daily, as this also help governs how much they can eat. However, parents or caregivers should also know that physical activity lowers blood sugar levels.
Type 1 diabetes poses a severe danger due to the sudden, extreme swings it causes in blood sugar. Therefore, the child must get a physical examination done as soon as possible when they notice any of the symptoms of juvenile diabetes to begin treatment immediately.
Some of the risk factors for type 1 diabetes in children may be
1) Family history: children with either or both of their parent or siblings with type 1 diabetes has a somewhat increased risk of developing juvenile diabetes.
2) Genetics: possession of specific genes are risk factors for type 1 diabetes in children.
3) Race: juvenile diabetes is more common among white children of non-Hispanic descent than among children of other races.
4) Certain viruses: Exposure to certain viruses may trigger the autoimmune attack and subsequent destruction of the insulin-producing cells.
A 30-year study carried out by the University of Pittsburgh, published in 2012, noted that children with juvenile diabetes born after 1965 had a life expectancy of 69 years.
Juvenile diabetes can affect the major organs in the body and, as a result, leads to certain complications.
1) Heart and blood vessel disease: juvenile diabetes puts the child at risk of developing medical conditions such as high blood pressure, narrowed blood vessels, heart disease, and stroke later in life.
2) Kidney damage: Juvenile diabetes can damage the numerous tiny blood vessel clusters that filter waste from the blood.
3) Eye damage. Diabetes can damage the retina’s blood vessels, which is likely to lead to vision problems.
4) Foot problems: They include ulcers and infections that can lead to gangrene.
5) Oral health problems
6) Stroke
Type 1 diabetes is an autoimmune condition in which the immune system attacks cells in the pancreas that produce insulin. A higher risk of developing type 1 diabetes is due to familial history.

























































