Chronic Gastrointestinal Bleeding
Usually, gastrointestinal (GI) bleeding can either occur in the upper or sometimes in the lower gastrointestinal tract. The causes of it are as follows: Read More
Top Doctors For Chronic Gastrointestinal Bleeding Treatments
Top Hospitals For Chronic Gastrointestinal Bleeding Treatments
Chronic Gastrointestinal Bleeding
Table of contents
What is gastrointestinal bleeding?
The human digestive or gastrointestinal tract includes the esophagus, stomach, small and large intestine, rectum, and anus. Bleeding from any of these areas can result in severe gastrointestinal bleeding. If bleeding occurs in the esophagus, stomach, or duodenum is considered upper gastrointestinal (GI) bleeding. While bleeding from the rest of the small intestine, large intestine, rectum, and anus is lower GI bleeding. The amount of bleeding varies from person to person and depends on the patient’s condition. It can be mild or severe.
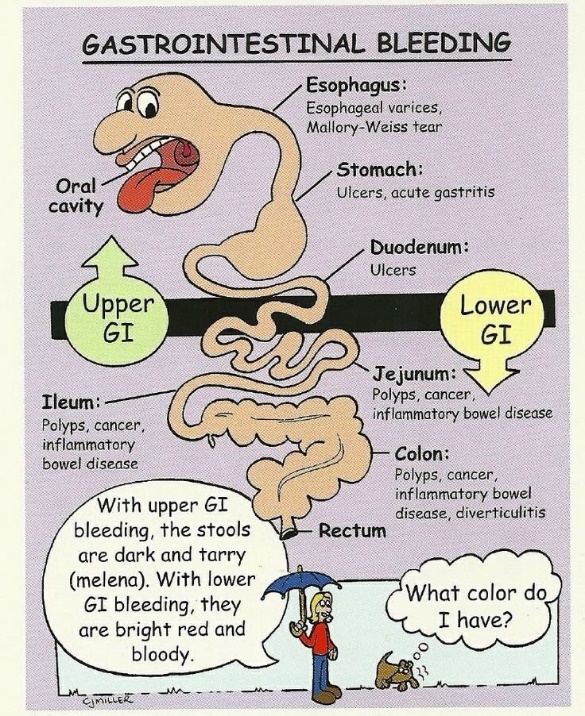
Causes
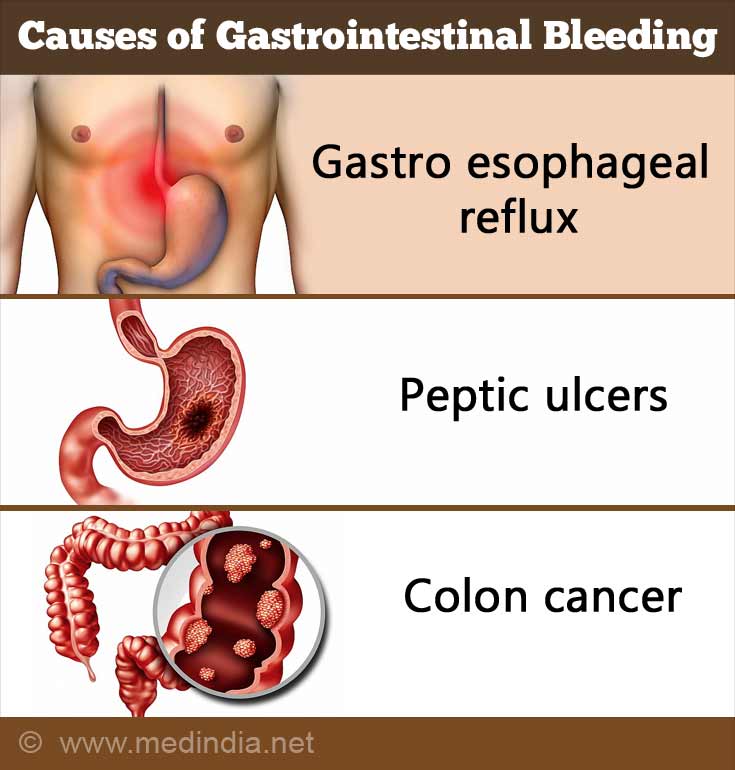
Usually, gastrointestinal (GI) bleeding can either occur in the upper or sometimes in the lower gastrointestinal tract. The causes of it are as follows:
Upper GI bleeding causes:
- Peptic ulcer: Most common cause of GI bleeding in the upper area is peptic ulcer. These ulcers are sores that develop on the stomach lining and the upper portion of the small intestine. The acid in the stomach is either from bacteria or the usage of anti-inflammatory drugs, and the lining of the stomach is damaged. It leads to the formation of sores.
- The lining of the tube which connects the throat to the esophagus getting torn
- Enlarged or sometimes abnormal veins in the esophageal varices
- Esophagitis
Lower GI bleeding causes:
- Tumors can weaken the digestive tract lining and cause GI bleeding
- Colon polyps can cause bleeding
- Hemorrhoids
- Anal fissures
- Diverticular disease
- IBD or Inflammatory Bowel Disease
- Proctitis
Symptoms
Chronic GI bleeding can be hidden or overt and usually depends on the bleed location. The symptoms of overt bleeding or chronic gastrointestinal (GI) bleeding are as follows:
- Vomiting blood that looks red or sometimes dark brown. It resembles coffee ground emesis in texture
- Black tarry stool (bright red blood in stool/blood in poop)
- Rectal bleeding which is usually seen in the stool.
Symptoms of occult bleeding are as follows:
- Lightheadedness
- Difficulty in breathing
- Fainting
- Chest pain
- Abdominal pain
Symptoms of a shock, especially when the bleeding starts and progresses fastly, the patient almost could get into shock. The signs of internal bleeding are as follows:
- Blood pressure drops
- Urinating in small amounts or not at all
- Rapid pulse
- Unconsciousness
How is chronic gastrointestinal bleeding diagnosed and treated?
Chronic Gastrointestinal Bleeding usually involves the following diagnosis and treatment procedures:
Prior to the treatment
Prior to the treatment, the diagnostic tests include:
- Physical examination and medical history– To diagnose GI bleeding, the doctor will examine the patient thoroughly and review and record the patient’s medical history. They include the history of bleeding in the past, the history of medications taken daily, lifestyle habitus, etc.
- Laboratory investigations– To confirm the disease, the doctor will advise the patient to undergo a couple of tests, including a complete blood count, liver function test, bleeding time and clotting time, and platelet count.
- RBC nuclear scan– During this examination, the doctor injects a harmless radioactive tracer into the patient’s body to track the red blood cells.
- Stool test- This test helps us determine the cause of occult bleeding.
- Nasogastric lavage- During this test, a thin tube is passed from the nose into the stomach to remove the stomach content. This test will help us determine the source of bleeding.
- Upper endoscopy– During this procedure, a thin, flexible tube and a camera are inserted into the upper part of the digestive tract to find the exact location of the bleeding.
- Capsule endoscopy
- Colonoscopy– It helps us to examine the large intestine and rectum.
- Flexible Sigmoidoscopy– It helps us examine the last part of the large intestine and rectum.
- Angiography– During this procedure, a contrast dye is injected into an artery, and a series of x-rays are taken to find the bleeding blood vessels and treat them.
- Investigational scans- They include ultrasonography and CT scan of the abdomen.
- Biopsy– During this examination, a small sample is taken from the bleeding area and later sent for pathological study. This study helps us to confirm and diagnose cancer.
During the Treatment:
Patients with mild chronic gastrointestinal bleeding generally do not require any treatment. In most cases, it heals on its own by adopting a healthy lifestyle and following a strict diet. While in a few cases, the patients can be treated using the following options.
- Medications: initially, the patients diagnosed with upper GI bleeding will be advised to take PPIs (proton pump inhibitors). It helps in suppressing the acid production in the stomach. The doctor might advise blood transfusion and I fluids for patients who had severe bleeding and were diagnosed with anemia due to GI bleeding.
- Surgery: In severe cases, the doctor might advise the patient to undergo invasive and non-invasive procedures to stop the bleeding. They include:
a) Endoscopy
b) Colonoscopy
c) Laparoscopy
During these procedures, a thin tube and a camera are passed into the gastrointestinal tract to find the cause and location of bleeding. The doctor might inject medications into the bleeding site to seal the bleeding area, use a clip or balloon, or cryotherapy to stop the bleeding, remove the polyp, etc.
Prognosis, Post-Treatment, and Recovery:
- Blood-thinning medications that include aspirin and other nonsteroidal anti-inflammatory medications will need to stop.
- The doctor will ask about regular checkups that include blood tests, as well as other tests like stool tests.
- Apart from that, the doctor will ask the patient to limit the use of nonsteroidal anti-inflammatory drugs (NSAIDs)
- Recovery of a patient with chronic gastrointestinal problems usually takes some time.
- Avoid alcohol consumption and smoking
What are the complications associated with chronic gastrointestinal bleeding?
A few of the complications of chronic gastrointestinal bleed in stools are as follows:
- Anemia
- Respiratory distress
- Infection
- Heart attack
- Shock
- Death
FAQ
The blood in the stools looks like bright red streaks, or it could look like blood mixed in with it. Blood in the stool is very dark and tarry. At times, the patient can even have stool blood that is not visible.
Black tarry stools usually indicate that the patient has injuries in the upper gastrointestinal tract, or in certain cases, it indicates bleeding.
Melena usually is a black tarry stool that occurs as a result of upper GI or gastrointestinal bleeding.
Constipation, hemorrhoids, and bowel syndrome that is irritable are a few disorders of gastrointestinal issues.
It is usually used to treat diarrhea as well as symptoms that are associated with indigestion.
The GI bleeding can be prevented by following these measures:
a) Limit or avoid taking alcohol
b) Limit the use of NSAIDs drugs
c) Quit smoking
d) Maintain a healthy lifestyle
e) Avoid food items that trigger the cause
f) Eat a high-fiber diet
g) Checking for infections like H. pylori.
h) Have a regular follow-up with the doctor.
The risk factors of gastrointestinal bleeding are:
a) Patients who are on anticoagulants
b) Using too much of NSAIDs drugs
c) Alcoholic abuse
d) Eating disorders, vomiting excessively
e) Traumatic injury
The intensity of GI bleeding varies from mild to severe. If diagnosed and treated early, the GI bleeding has a good prognosis. Whereas if left untreated, it can lead to life-threatening conditions, including death.
They include:
a) Acute- sudden, severe bleeding is seen.
b) Chronic- the GI bleed persists over a long period (on and off).
c) Occult bleeding is not evident since it is microscopic. The signs of blood loss can be revealed only through laboratory investigations.
d) Overt-visible signs of GI bleed are seen, which include blood in vomit and black tarry stools (melena).
e) Obscure- when standard endoscopy procedure does not reveal a source of GI bleeding.
Early diagnosis and early treatment of GI bleeding have a good prognosis. Most of the patients recover completely. The patient may require a few weeks to months to recover completely. Leading a healthy lifestyle and eating healthy can result in fewer chances of recurrence of GI bleeding.



























































































