Diabetic Retinopathy
What is a Retina and what is Diabetic Retinopathy? The retina is a layer of tissue found in the back of the eye that receives light and visual information information and transmits it to the brain. Diabetic Retinopathy, is an eye condition that causes changes to the blood vessels in the part of the eye […] Read More
Top Doctors For Diabetic Retinopathy Treatments
Top Hospitals For Diabetic Retinopathy Treatments
Diabetic Retinopathy
What are the symptoms of Diabetic Retinopathy?
The symptoms of diabetic retinopathy are: There are no early symptoms or warnings of the onset of this disease. However, in later stages the following symptoms can manifest:- Spots or dark strings floating in your vision (floaters)
- Blurred or non-focused vision
- Dark or empty areas in vision
- Loss of central vision
- Night blindness
- Color blindness [2]
- Eye pain
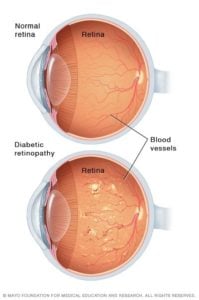 Picture Courtesy: Mayo Clinic
Picture Courtesy: Mayo Clinic
Causes of Diabetic Retinopathy
As the very name indicates, when the blood sugar increases, this leads to the blockage of the blood vessels that feed the retina. Ultimately the blood supply is cut off. To circumvent this, the blood vessel tries to grow new blood vessels, which is usually not successful, and the blood vessels leak. This leads to blurrness, finally leading to blindness. Macular edema and swelling are the most common cause of loss of vision in diabetic retinopathy [3]. Types of Diabetic Retinopathy: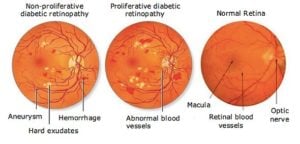 Picture Courtesy: Retinamd
Early Diabetic Retinopathy: It is also called non-proliferative diabetic retinopathy (NPDR) — In this case, the new blood vessels are not formed. . When someone has NPDR, the walls of the blood vessels feeding the retina weaken. Due to this, tiny bulges called microaneurysms protrude from the walls of the smaller vessels, at times leaking fluid and blood into the retina. Larger retinal vessels begins to dilate and become irregular in diameter. NPDR can progress from mild to severe as more blood vessels become blocked.
Retinal blood vessel damage also leads to a buildup of fluid (edema) in the center portion (macula) of the retina. Macular edema decreases vision, and immediate treatment is required to prevent permanent vision loss.
Advanced Diabetic Retinopathy. Once the Diabetic Retinopathy progresses to a severe type, it is called Proliferative Diabetic Retinopathy (PDR). In this type, the damaged blood vessels feeding the Retina cease to transport blood. This causes the growth of new, abnormal blood vessels in the retina. These new blood vessels are fragile and can leak into the clear, jellylike substance that fills the center of the eye (vitreous fluid).
The scar tissue from the growth of new blood vessels is likely to cause the retina to detach from the back of the eye. The new blood vessels interfere with the normal flow of fluid out of the eye, and pressure builds in the eyeball. This buildup damages the nerves that carry light and images from the eye to the brain (optic nerve), resulting in glaucoma.
Picture Courtesy: Retinamd
Early Diabetic Retinopathy: It is also called non-proliferative diabetic retinopathy (NPDR) — In this case, the new blood vessels are not formed. . When someone has NPDR, the walls of the blood vessels feeding the retina weaken. Due to this, tiny bulges called microaneurysms protrude from the walls of the smaller vessels, at times leaking fluid and blood into the retina. Larger retinal vessels begins to dilate and become irregular in diameter. NPDR can progress from mild to severe as more blood vessels become blocked.
Retinal blood vessel damage also leads to a buildup of fluid (edema) in the center portion (macula) of the retina. Macular edema decreases vision, and immediate treatment is required to prevent permanent vision loss.
Advanced Diabetic Retinopathy. Once the Diabetic Retinopathy progresses to a severe type, it is called Proliferative Diabetic Retinopathy (PDR). In this type, the damaged blood vessels feeding the Retina cease to transport blood. This causes the growth of new, abnormal blood vessels in the retina. These new blood vessels are fragile and can leak into the clear, jellylike substance that fills the center of the eye (vitreous fluid).
The scar tissue from the growth of new blood vessels is likely to cause the retina to detach from the back of the eye. The new blood vessels interfere with the normal flow of fluid out of the eye, and pressure builds in the eyeball. This buildup damages the nerves that carry light and images from the eye to the brain (optic nerve), resulting in glaucoma.
Diagnosis of Diabetic Retinopathy
A comprehensive eye exam can identify the start and progress of Diabetic retinopathy. The tests are mainly done on the Retina and the Macula. Normally, the patient’s family background and history are discussed to determine the history of diabetes, potential vision issues, and other general health issues that affect the vision. The following tests are done- HbA1c levels should be monitored regularly in long-term follow-up care of diabetes and diabetic retinopathy.
- Fluorescein angiography to evaluate abnormal blood vessel growth.
- Optical coherence Tomography (OCT)- It is done to determine the thickness of the retina and the presence of swelling within the retina [4].
- B-scan ultrasonography is used to evaluate the status of the retina
Treatment of Diabetic Retinopathy
The treatment of diabetic retinopathy varies depending on the extent of the progress of the disease. Mild and moderate diabetic retinopathy does not require immediate treatment. However, the patient will be closely monitored by the ophthalmologist in order to assess when the patient might require treatment. The aim of the treatment is to stop or reverse the progress of the disease. Some of the common treatment methods include:- Surgery to remove and replace the gel-like fluid in the back of the eye.
- Laser treatment (Photocoagulation) is used to seal the leaking blood vessel. During this procedure, the leak from the abnormal blood vessels is treated with laser burns.
- Panretinal photocoagulation: During this procedure, the scatter laser beam can shrink the abnormal blood vessels.
- Vitrectomy: During this procedure, a tiny incision is made in the eye in order to remove blood from the middle of the eye as well as scar tissue that’s present in the retina [5].
- Injection of medication inside the eye to stop the formation of abnormal blood vessels. A few of the medications which are advised are – Triamcinolone, Bevacizumab, Ranibizumab.
- Ovine Hyaluronidase Therapy. Helps in clearing severe vitreous hemorrhage [6].
Prevention of Diabetic Retinopathy
Usually, prevention is better than cure. Patients with diabetic conditions should take extra care in controlling the level of sugar in the body by diet control and take prescribed medicines regularly. A pregnant patient who is diagnosed with gestational diabetes should visit an ophthalmologist and get a thorough eye check done during their first trimester. Some other prevention tips are controlling the blood pressure, cholesterol levels, exercising regularly and avoiding alcohol or other drugs, and stop smoking.FAQ
What other problems diabetic retinopathy can cause?
Diabetic retinopathy can cause diabetic macular edema, neovascular glaucoma and retinal detachment.
What is the outlook for people diagnosed with diabetic retinopathy?
Early diagnosis and early treatment result in a good outcome. With timely treatment, we can delay diabetic retinopathy progression and can prevent loss of vision. The best way to prevent the progression of the disease is to control the blood sugar level and follow the medications advised regularly [7].
What are the risk factors for diabetic retinopathy?
The risk factors for diabetic retinopathy are- uncontrolled blood sugar levels, gestational diabetic patients (diabetes during pregnancy), hypertension, hyperlipidemia.
What percentage of diabetes get diabetic retinopathy?
After 15years of a patient being diabetic, 98% of those with Type 1 diabetes and 78% of those with Type 2 diabetes have some degree of retinal damage [8].










































































































