Embryo Genetic Testing
Embryo genetic testing is an umbrella term that houses two procedures that can be done on an embryo before they are transferred to the uterus. These procedures are pre-implantation genetic screening (PGS) and pre-implantation genetic diagnosis (PGD); they are both screening tests that can be performed on embryos that were generated using in vitro fertilization (IVF). Read More
Top Doctors For Embryo Genetic Testing Treatments
Top Hospitals For Embryo Genetic Testing Treatments
Embryo Genetic Testing
Table of contents
- What is Embryo Genetic Testing?
- What is pre-implantation genetic screening (PGS)?
- Why do couples request pre-implantation genetic screening?
- What is pre-implantation genetic diagnosis?
- Why do couples request for pre-implantation genetic diagnosis?
- How is embryo genetic testing in IVF done?
- What are the risks associated with embryo genetic testing?
- Ethical issues of embryo genetic testing
What is Embryo Genetic Testing?
Embryo genetic testing is an umbrella term that houses two procedures that can be done on an embryo before they are transferred to the uterus. These procedures are pre-implantation genetic screening (PGS) and pre-implantation genetic diagnosis (PGD); they are both screening tests that can be performed on embryos that were generated using in vitro fertilization (IVF). The procedures are done to genetically screen them and ensure that they are top quality before they are transferred to the uterus for implantation.
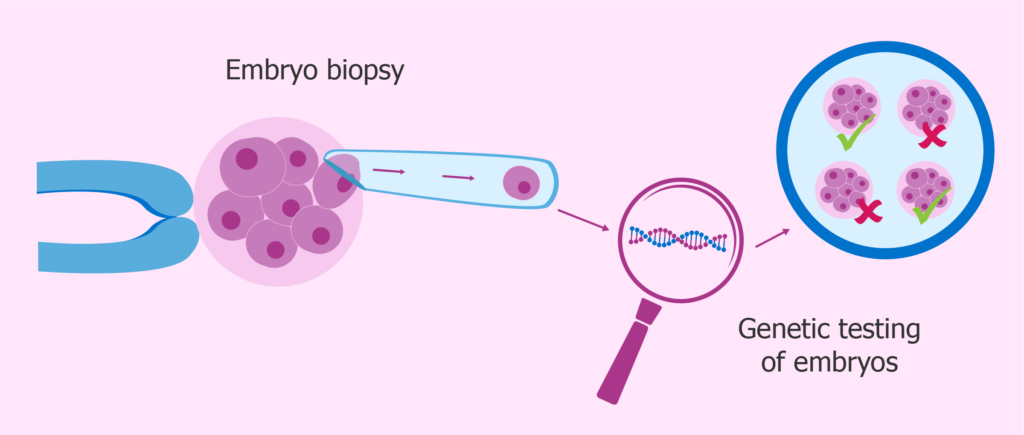
What is pre-implantation genetic screening (PGS)?
This is a test used to determine if an embryo contains cells with the normal number of chromosomes (46). The test is carried out on the 5th day of growth of an embryo, usually in the blastocyst stage. A few cells from the embryo are sent to the lab, where the number of chromosomes within each cell is counted. Embryos that possess the normal number of cells are euploid while those with abnormal cell numbers are aneuploid. The purpose of this screening is to avoid transferring an abnormal embryo into the uterus.
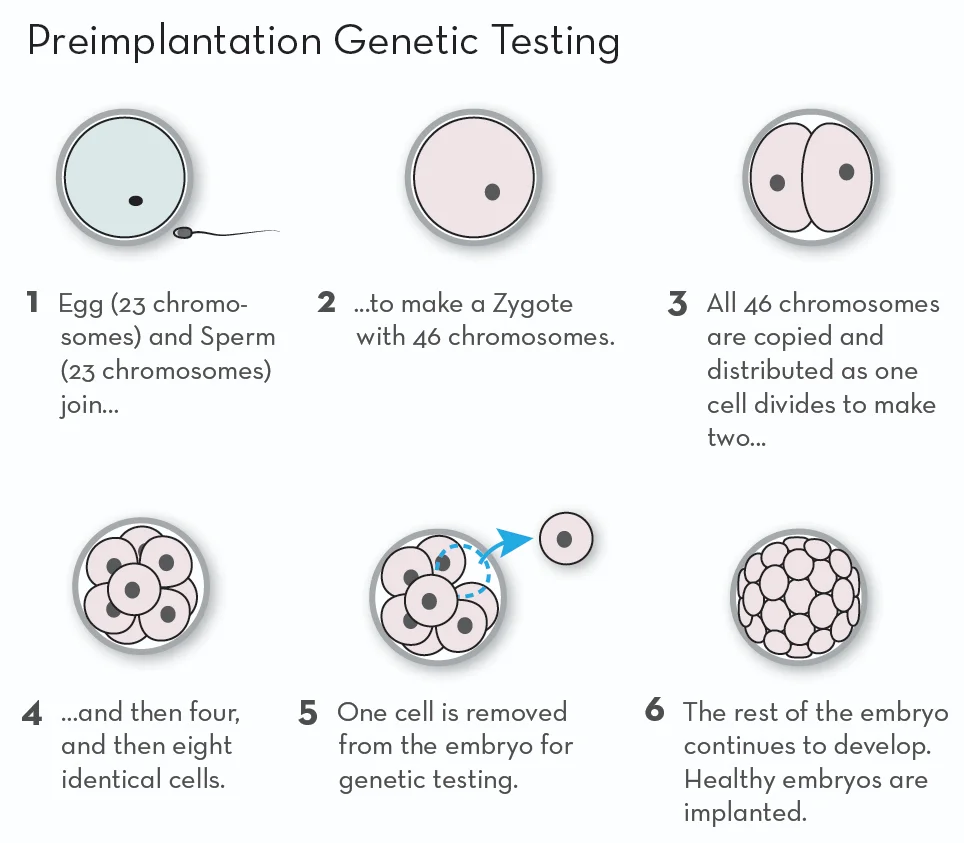
Why do couples request pre-implantation genetic screening?
One of the main reasons for requesting the screening of an embryo before a transfer is to ensure that the embryo transfer results in a viable pregnancy. The genetic screening can ensure that the selected embryo possesses an adequate number of chromosomes. This, in turn, reduces the chances of a failed IVF cycle that results in a miscarriage.
All couples are at risk of having abnormal embryos. The risk increases significantly, however, as the woman gets older. An abnormal embryo, when transferred, fails to implant, and even when it does implant, it can cause a miscarriage, fetal death, a stillbirth, or a baby with abnormalities. Couples may also choose to carry out pre-implantation genetic screening when there is severe male factor infertility, a huge number of embryos, older age, or recurrent failures of the IVF cycles.
The use of PGS has grown in popularity because of couples that want to transfer a normal embryo and avoid problems associated with an abnormal embryo. It is estimated that PGS is used in about 35% of all IVF cases, with the number expected to reach 50% of all IVF cycles.
What is pre-implantation genetic diagnosis?
Pre-implantation genetic diagnosis is a test that is used to examine the genetic information of cells in an embryo. A biopsy of an embryo removes about 8 cells from an embryo that is at the blastocyst stage (5 days old). The removed cells are then sent to the lab for examination. Meanwhile, the embryo is usually frozen and stored, to be implanted after the testing. PGD can b used to identify about 2000 inherited single-gene disorders and is about 98% accurate in recognizing affected and unaffected embryos.
Why do couples request for pre-implantation genetic diagnosis?
Pre-implantation genetic diagnosis is used by couples that have a serious heritable disease and are afraid of passing it to their offspring. The diagnosis searches for markers that indicate the presence of a specific disease, like single gene disorders which include sickle cell anemia. A genetic diagnosis can also be done when there is a family history of sex-linked disorders like Duchenne muscular dystrophy. In some cases, parents may use genetic diagnosis to find matching stem cells for their other kids that may need stem cell transplants.

How is embryo genetic testing in IVF done?
The steps in both PGD and PGS are similar up to a point; the first step is embryo biopsy. The second step is the analysis of the cells collected by biopsy in a laboratory. In both forms of testing, the biopsy is carried out at the blastocyst stage (day 5 or day 6 of the embryo culture) of development. The blastocyst is made up of two cells, the inner cell mass (ICM) that goes on to form the fetus and the trophectoderm (TE) that allows the placenta to develop. The biopsy removes 3-8 cells from the trophectoderm which is then taken to a laboratory for genetic testing. The inner cell mass that will eventually develop into the baby is not touched.
The result of the testing or screening is usually available within 7-10 days after the biopsy. The embryo is frozen immediately after the biopsy to wait for the result of the screening, after the results confirm it to be a top-quality embryo, it is thawed and transferred to the uterus of the woman.
What are the risks associated with embryo genetic testing?
There are no documented health risks currently associated with children born after embryo genetic screening beyond the already known hazards that face the mother and child through IVF. The entire process of embryo genetic testing however results in a small risk of damage which may lead to the embryo that fails to implant in the uterus. Around 5% of the embryos that are screened during embryo genetic testing will be lost due to that damage. Another major risk of embryo genetic testing is the inaccuracies in some of the test results. This is because the test is not 100% accurate, which is why it is also recommended that the woman should also undergo typical prenatal testing when she is pregnant.
Ethical issues of embryo genetic testing
With the evolution of embryo genetic testing technology, it might become a common practice to select particular genetic traits to pass to a child through embryo selection and screening. Originally, the technology was developed just to increase the number of successful IVF births, but advances will ensure that it will be used in the future by parents to look for traits that they would desire to pass on to their offspring, while also selecting particular traits that they do not want to be passed on. This puts embryo genetic testing in the moral ground of eugenics, which is a past scientific practice that attempted to improve the human population through selective breeding for desired characteristics. Experts foresee that this could become an issue for clinics that offer the service and especially for patients that will have to decide on whether they will use it or not.



































