Kidney Transplant
What is a kidney, and what is the kidney’s main function? A kidney is a bean-shaped organ located on each side of the spine below the ribcage in the abdomen. They are two in number. The kidney majorly filters and removes waste, minerals, and fluid from the blood by producing urine. What is a Kidney […] Read More
Top Doctors For Kidney Transplant Treatments
Top Hospitals For Kidney Transplant Treatments
Kidney Transplant
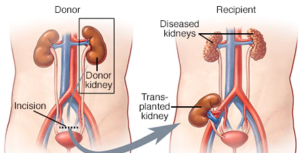
What is a Kidney transplant?
A kidney transplant is a surgical procedure where we transplant a healthy kidney from a living or a deceased donor into a person whose kidneys are no longer functioning properly [1]. Kidney transplantation is a technique of implanting a kidney from one person to another with end-stage kidney disease or kidney failure. Options for Kidney Failure Patients1. Peritoneal Dialysis is of two types:
-
-
- Continuous Ambulatory Peritoneal Dialysis (CAPD) where the patient can do the exchanges three to four times daily.
- Continuous Cycling Peritoneal Dialysis (CCPD) where a machine (cycler) automatically does the exchanges while the patient is asleep. If the the kidney function decreases further, the patient may need to perform additional exchanges during the day.
-
2. Hemodialysis: Here, blood flows through a machine (dialyzer or artificial kidney) that has a filter. Hemodialysis access can be through an arteriovenous fistula, a graft, or a catheter. This process is done for several hours about three times a week. It can be done at a dialysis center.
3. Kidney Transplant
Why do we need Kidney Transplant? Whenever kidneys fail to function properly, i.e., they do not completely expel toxic substances from the body leading to the accumulation of waste materials in the body. When these accumulations reach harmful levels, they will result in end-stage renal failure, a life-threatening condition. In such cases, the doctor advises dialysis, which has to be done twice or thrice a week for the rest of the patient’s life. Dialysis imposes severe limitations on lifestyle and travel. Whereas after a successful kidney transplant, the patient can lead nearly a normal life with some mandatory precautions. What are the benefits of a kidney transplant? Kidney transplant is associated with:-
-
- Better quality of life
- Lower risk of death (extended life)
- Fewer dietary restrictions
- Lower overall treatment cost
- Better travel options.
- More energy
- Stopping dialysis
-
-
-
- Advanced age equal to or greater than 80
- Severe heart disease
- Active or recently treated cancer
- Dementia or poorly controlled mental illness
- Alcohol or drug abuse
- Recurrent infections that are not treated effectively.
- Severe pulmonary disease
- Uncontrolled psychiatric disorders
- Inability to cover expenses of kidney transplant and subsequent care.
-
-
-
- Deceased Donor Kidney Transplant: a donated kidney from a recently deceased person is used
- Living Donor Kidney Transplant – related or unrelated: Kidney from a living donor is used for the procedure.
- Kidney paired donation/swap: For instance, kidney from donor A that does not match with patient A is used for patient B who is a match. Then, kidney from donor B is used for patient A if it is a match. Thus, increasing the chance of benefitting from a living donor transplantation.
-
Process of Kidney Transplant:
Kidney transplantation requires a multidisciplinary approach from a team of several specialists, namely:-
-
- Nephrologist
- Surgeon/Nurse practitioner
- Pharmacist
- Dietitian
- Specialty physicians (cardiology, hematology, pulmonology, etc.)
- Transplant administrator
- Transplant clinic coordinator
- Quality coordinator, etc.
-
-
-
- Urine Test – Urinalysis, microalbumin, urine creatinine, albumin-creatinine ratio
- Blood Test – CBC, renal function test, electrolytes, lipid profile, uric acid, coagulation profile, viral markers, etc.
- Abdominal Ultrasonography
- Uroflometry
- Cystoscopy and MCU
- CT imaging
- Colonoscopy and/or upper endoscopy
- Prostate exam
- Cardiac testing
- Mammogram/pap smear
- Dental clearance
- Isotope renogram for donor
-
-
-
- If the recipient’s blood type is A, Donor blood type must be A or O
- If the recipient’s blood type is B, Donor blood type must be B or O
- When the recipient’s blood type is O, Donor blood type must be O
- If the recipient’s blood type is AB, Donor blood type can be A, B, AB, or O
-
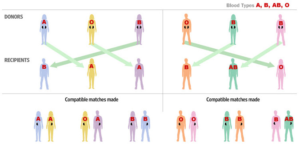 Picture courtesy: Organ India
Tissue Typing
The second test is a blood test for human leukocyte antigens (HLA), also called tissue typing. Antigens are markers found on many body cells that distinguish each individual as unique. Every person has 6 antigens, out of which 3 are inherited from their biological parents. Having a successful transplant is high when these antigens are matched with the donors. HLA matching is done by mixing a small amount of the recipient blood with the donor’s blood [9].
The best chance of working for many years exists with perfect match transplants. Most perfect match kidney transplants come from siblings.
Although tissue typing is done despite partial or absent HLA match with some degree of “mismatch” between the recipient and donor (please see our section on Bone Marrow Transplant).
Picture courtesy: Organ India
Tissue Typing
The second test is a blood test for human leukocyte antigens (HLA), also called tissue typing. Antigens are markers found on many body cells that distinguish each individual as unique. Every person has 6 antigens, out of which 3 are inherited from their biological parents. Having a successful transplant is high when these antigens are matched with the donors. HLA matching is done by mixing a small amount of the recipient blood with the donor’s blood [9].
The best chance of working for many years exists with perfect match transplants. Most perfect match kidney transplants come from siblings.
Although tissue typing is done despite partial or absent HLA match with some degree of “mismatch” between the recipient and donor (please see our section on Bone Marrow Transplant).
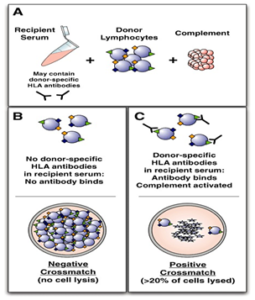 Picture Courtesy: Medcraveonline
Crossmatch
Our body makes substances called antibodies that destroy foreign materials. These antibodies are activated when our body is exposed to an infection, during pregnancy, blood transfusion, or after transplants. During any of these above processes, our antibodies consider them as foreign particles, attack them, and kill. If there are any antibodies present on the donor’s kidney, the recipient’s immune system may destroy the kidney. For this reason, when a donor’s kidney is available, a crossmatch test is done to ensure the recipient does not have preformed antibodies to the donor.
The crossmatch test involves mixing the recipient’s blood with cells from the donor. A negative crossmatch result indicates that the recipient does not have antibodies to the donor and that they are eligible to receive this kidney. Cross matches are performed several times during preparation for a living donor transplant, and a final crossmatch is performed within 48 hours before this type of transplant. – Serology testing is also done for viruses, such as HIV (human immunodeficiency virus), hepatitis, and CMV (cytomegalovirus), to select the proper preventive medications after transplant. There is extensive screening against these viruses in any potential donor to assist in preventing the spread of disease to the recipient.
Precautions for Donor
Picture Courtesy: Medcraveonline
Crossmatch
Our body makes substances called antibodies that destroy foreign materials. These antibodies are activated when our body is exposed to an infection, during pregnancy, blood transfusion, or after transplants. During any of these above processes, our antibodies consider them as foreign particles, attack them, and kill. If there are any antibodies present on the donor’s kidney, the recipient’s immune system may destroy the kidney. For this reason, when a donor’s kidney is available, a crossmatch test is done to ensure the recipient does not have preformed antibodies to the donor.
The crossmatch test involves mixing the recipient’s blood with cells from the donor. A negative crossmatch result indicates that the recipient does not have antibodies to the donor and that they are eligible to receive this kidney. Cross matches are performed several times during preparation for a living donor transplant, and a final crossmatch is performed within 48 hours before this type of transplant. – Serology testing is also done for viruses, such as HIV (human immunodeficiency virus), hepatitis, and CMV (cytomegalovirus), to select the proper preventive medications after transplant. There is extensive screening against these viruses in any potential donor to assist in preventing the spread of disease to the recipient.
Precautions for Donor
-
-
- Maintain the diet and exercise guidelines
- No smoking
- Take the prescribed medications
- Keep all appointments with the healthcare/transplant team
- Carry out healthy activities and remember to relax
-
What are the side effects of Kidney Transplant?
Kidney transplant is the most sought-after organ transplant treatment availed by patients worldwide. Reportedly, more than 40 percent of Kidney transplant operations had taken place in 2014. Many patients proclaim they have been living happily after that without any other health issues. Still, post-surgery, one could be prone to some side effects, which, if neglected, could be life-threatening. There 2 types of side effects:• Life-threatening side effects
• Minor and common side effects
Life-threatening side effects: Fever reaches above 101 degrees Fahrenheit temperature. Doctors suggest monitoring the body’s temperature everyday post-treatment. Beyond 101 or at the limit calls for caution. A transplant treatment includes immunosuppressant medications, which can take a toll on an individual’s immune system, making one prone to severe illnesses like cancer. Kidney transplants before the 1950s resulted in patient’s death due to negligence of high body temperature. Increase in weight: Many patients post the treatment reported an increase in body weight of 5 to 7 pounds in less than 4 days. The main reason for this aftereffect is the intake of Prednisone, an immunosuppressant drug given to transplant patients, affecting blood sugar levels. Disruption in Urine Output and change in the pattern: A disruption in urine output, change in pattern, color change in the urine are symptoms that could indicate the presence of the BK Virus. If left unchecked, it could lead to tissue damage, so do not forget to report erratic urine patterns to the doctor. High Blood Pressure: A person with extraordinarily high or low blood pressure is prone to many other health risks, especially after a Kidney Transplant. One can expect their blood pressure levels to rise, and 80-90 percent of patients have experienced similar effects. This is due to the excessive medication prescribed. Therefore, ensure blood pressure levels are monitored closely and within the average level. Tooth Pain: Before undergoing a transplant, a patient would undergo dental checks. These medicines would lead to the growth of excessive gums (formation of patches in between teeth). Hence post-transplant, do not forget to consult the dentist once a month and see if the patient is free of dental complications. Vascular thrombosis and stenosis Delayed graft function Ureteral obstruction [4]. Minor and Common Side Effects: Excessive Hair Growth and Hair Loss: Hormonal changes are some of the resultant effects of the anti-rejection medication given post Kidney Transplant. These hormones could encourage excessive hair growth in the chest and other body parts and loss of hair from the head. But it is said to be under control after the medicine is completed. Acne: Intake of Prednisone medicine could trigger acne formation on the face, chest, shoulders, and other body parts. It tends to fade away after the medicines. A permanent scar could arise from rubbing the acne excessively. Doctors suggest washing with cold water. Exposure to Sun: A kidney transplant patient is more vulnerable to burning sensations when exposed to the sun. Prednisone makes one’s skin more prone to sensitivity. Such issues do not arise after the medication.Symptoms
Early stages of kidney failure usually show no symptoms. When the disease progresses, there are many signs observed, such as:
-
-
- Swelling of the hands, feet and face (edema)
- Headaches (due to high blood pressure)
- Seizures, pale skin color (due to low iron)
- Coffee-colored urine
- Bad breath that cannot be freshened by brushing your teeth
- Fatigue
- Itchy skin
- Need to urinate often, especially at night
- Decreased mental sharpness
- Problems with sleep
- Erectile dysfunction in men
- Nausea
- Twitching in the muscles and cramps
- Shortness of breath if fluid accumulates in the lungs
- Chest pain, especially when fluid builds up around the lining of the heart
-
Causes
Common causes of end-stage kidney disease include:
-
-
- Chronic Diabetes
- Chronic glomerulonephritis (scars in the kidney’s tiny filters)
- Polycystic kidney disease
- Uncontrolled high blood pressure
- High blood sugar (diabetes)
- High blood pressure
- Hardening of the arteries
- Obesity
- Older age untreated strep infections
- Chronic kidney infections
- Bad diarrhea
- Kidney stones
- Long-term use of non steroidal nonsteroidal anti-inflammatory drugs (NSAIDs)
-
FAQ
What is Life Expectancy after Kidney Transplant?
A patient received a kidney in 1973 and is still alive (perhaps it was a perfect match as her mother was her donor). However, if the patient has a kidney transplant and if there is no rejection, the patient can live easily above 10 years.
The success of kidney transplantation technology has grown such that 1-year graft survival now exceeds almost 95%
Who is eligible for a kidney transplant?
Patients diagnosed with end-stage renal failure or those with chronic kidney disease stage 4 with the progressive disease should be assessed for a kidney transplant [8].
Why is a kidney transplant better than dialysis?
A kidney transplant is considered a treatment of choice for many end-stage renal failure patients. A successful kidney transplant can improve the quality of life and reduce the risk of dying. People who undergo transplant doesn’t require dialysis. In contrast, patients on dialysis have to undergo dialysis procedures two to three times a week throughout their lives [6].
Can kidney transplant patients get the covid vaccine?
Kidney transplant patients can take the covid vaccine but should wait for 3 months after transplantation [7].
What happens when a kidney transplant fails?
The doctor will suggest dialysis or consider second transplantation. If the patient decides to discontinue treatment, the doctor will suggest certain medications to help relieve symptoms. The decision will generally depend on the patient’s current health condition, ability to withstand the surgery and expectations for maintaining a certain quality of life [5].
References
- https://www.mayoclinic.org/tests-procedures/kidney-transplant/about/pac-20384777
- https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/kidney-transplant
- https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/kidney-transplant
- https://emedicine.medscape.com/article/430128-technique#c6
- https://www.mayoclinic.org/tests-procedures/kidney-transplant/about/pac-20384777
- https://www.uptodate.com/contents/dialysis-or-kidney-transplantation-which-is-right-for-me-beyond-the-basics#:~:text=Advantages%20%E2%80%94%20Kidney%20transplantation%20is%20the,require%20hours%20of%20dialysis%20treatment.
- https://www.vcuhealth.org/news/covid-19/covid-19-vaccines-and-transplant-patients-is-it-safe#:~:text=New%20transplant%20recipients%20should%20delay,one%20month%20after%20their%20transplant.
- https://teachmesurgery.com/transplant-surgery/organ-transplantation/renal/.
- https://www.healthline.com/health/kidney-transplant#donor-matching

For more answered questions by Dr. Krishna Mohan R, Senior consultant urologist & transplant surgeon at Miart – Metromed Institute of Advanced Urology and Renal Transplant, click this link for a video to our webinar with him.
































