Mesenteric Ischemia
“Mesentery” is used to describe the substance found in the abdomen that helps holds the intestine in place to the abdominal wall. It contains blood vessels that supply the intestine. Ischemia is said to happen when blood flow is limited or affected due to a blockage in the blood vessels of a particular area. What […] Read More
Top Doctors For Mesenteric Ischemia Treatments
Top Hospitals For Mesenteric Ischemia Treatments
Mesenteric Ischemia
Table of contents
- What is Mesenteric Ischemia?
- What are the types of Mesenteric Ischemia?
- Causes
- What are the risk factors for Mesenteric Ischemia?
- Symptoms
- How is Mesenteric Ischemia diagnosed?
- How is Mesenteric Ischemia treated?
- What are the complications of Mesenteric Ischemia?
- Can Mesenteric Ischemia be prevented?
- FAQ
What is Mesenteric Ischemia?
Mesenteric Ischemia, also called ‘Bowel Infarction’, is the narrowing or blockage of arteries supplying the intestine, resulting in restricted blood flow to the intestine, which could lead to damage in the intestine as oxygen intake is also affected.
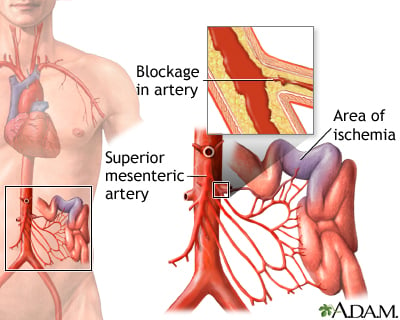
“Mesentery” describes the substance found in the abdomen that helps hold the intestine in place to the abdominal wall. It contains blood vessels that supply the intestine. Ischemia is said to happen when blood flow is limited or affected due to a blockage in the blood vessels of a particular area.
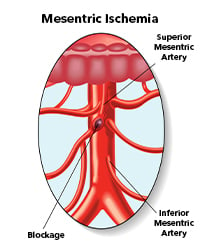
What are the types of Mesenteric Ischemia?
It can be classified into:
- Acute Mesenteric Ischemia
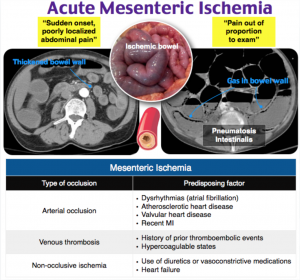
It is characterized by a sudden interruption of blood flow to the different parts of the small intestine, which could lead to inflammatory changes, ischemia, cellular damage and death, and sometimes intestinal necrosis. Here, symptoms could occur promptly without any indication, resulting in serious health complications and even death. Therefore, it is mainly treated with surgery.
- Chronic Mesenteric Ischemia
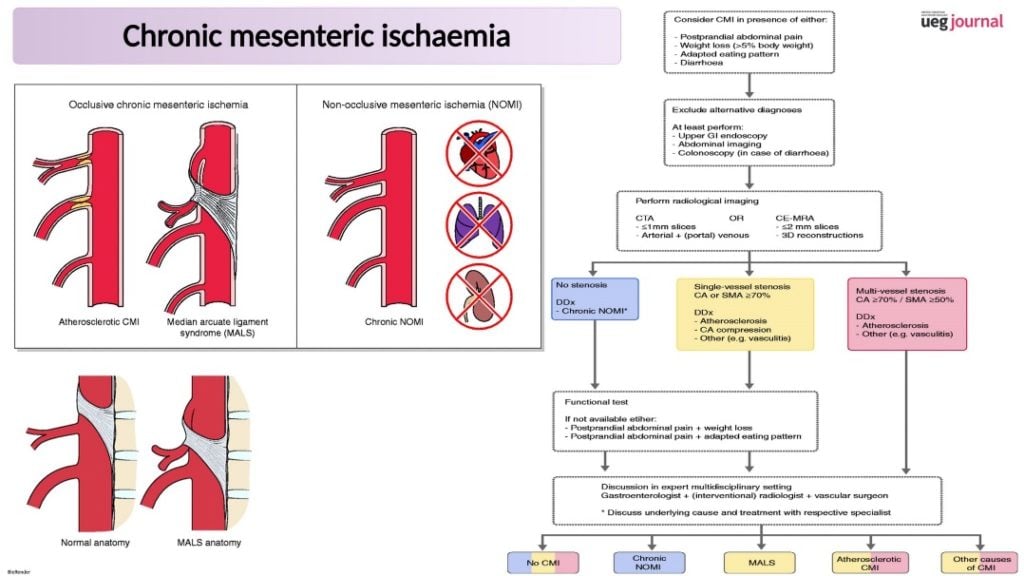
Chronic Mesenteric Ischemia is progressive and builds up slowly. It could happen due to a blockage in the small intestine’s major arteries. When left untreated, it could progress to being acute. It can be treated using angioplasty.
Causes
It is caused by slow or insufficient blood flow to the small intestine. However, acute Mesenteric Ischemia could also result from a blood clot in the Mesenteric artery, which could originate from the heart. At the same time, chronic is caused by the assimilation of plaque that narrows the blood vessels.
Some other causes include:
- Aortic dissection; a tear in the aorta’s inner layer.
- Coagulation disorders
- Congestive heart failure
- Low blood pressure
- Blockage or occlusion of veins in the bowel
- Fibromuscular dysplasia and arthritis that is disorders of the blood.
What are the risk factors for Mesenteric Ischemia?

Certain factors can lead to Mesenteric Ischemia. They include:
- Age; usually people older than 60.
- High cholesterol, hypertension (increase in blood pressure)
- Coronary heart diseases
- People who smoke a lot
- History of trauma, kidney failure, decompression sickness
- Use of cocaine
- Blood that quickly clots.
Symptoms
The symptoms can be acute or chronic:
Acute Mesenteric Ischemia
They include:
- Abrupt and severe abdominal pain
- Urgent need to have a bowel movement
- Fever
- Nausea and vomiting
Chronic Mesenteric Ischemia
- Abdominal pain begins about 30 minutes after eating and worsens over an hour.
- Pain, which goes away within one to three hours.
- Weight loss.
- Flatulence.
If the pain becomes severe and abrupt abdominal pain persists, they need to see the doctor immediately.
How is Mesenteric Ischemia diagnosed?
It can be diagnosed through:
- A blood test to check for intestinal ischemia.
- Imaging tests such as computerized tomography scans and X-rays are used to get images of the intestine.
- Stool culture
- Imaging studies include an x-ray scan of the abdomen, a CT scan, and an MRI scan.
- A mesenteric arteriogram is considered the golden standard of investigation in diagnosing acute mesenteric ischemia. During this procedure, a contrast dye is injected into the blood vessels, and x-ray images are obtained to identify any narrowing or blockage in the arteries.
- Endoscopy or colonoscopy is done. This involves inserting a lighted, flexible tube with a camera on its tip into the mouth or rectum. An image of the gastrointestinal tract is viewed. The stomach and upper part of the small intestine are examined in endoscopy or, if inserted through the rectum (colonoscopy), then the colon is viewed.
- Open or exploratory surgery is done. During this procedure, intraoperative florescence dye is used to delineate those areas of the bowel that need resection.
How is Mesenteric Ischemia treated?
For Acute Mesenteric Ischemia, treatment involves:
- Surgery is mainly recommended to remove blood clots (embolectomy), bypass an artery blockage (revascularization), and remove the damaged intestine.
- Clot-busting medications are also used to dissolve clots and dilate blood vessels.
- The artery may be kept open with a stent.
Treatment for Chronic Mesenteric Ischemia includes:
- Angioplasty surgery or therapy.
- Medications such as anticoagulants (warfarin) reduce blood clot risk.
- Also, the artery may be kept open with a stent.
- Trans-aortic Endarterectomy, a process of removing the plaque blocking the artery, can be done.
Recovery
When treatments are done early enough to stop complications from arising, recovery can take 4 to 8 weeks. However, the doctor may resist the activities, and the patient will have to follow up regularly with the doctor. Make sure to rest frequently, eat healthily, reduce cholesterol intake, quit smoking, and exercise often.
What are the complications of Mesenteric Ischemia?
The complications that can arise if the condition is not treated on time can include:
- Sepsis: a condition where the body overreacts to chemicals released to fight infections, leading to multiple organ failures.
- Acute-on-chronic form of the condition.
- Bleeding
- Heart attack or stroke
- Parts of the bowel begin to die, leading to irreversible intestinal damage.
- Death in extreme cases.
Can Mesenteric Ischemia be prevented?
One can prevent this condition by:
- Avoiding smoking
- Healthy feeding
- Regular exercises
- Reduce meals with high cholesterol
- Avoiding stress that might lead to high blood pressure.
FAQ
Mesenteric ischemia could be acute or chronic.
The acute form is characterized by sudden symptoms, resulting in a severe health crisis, even death. In contrast, the chronic form develops gradually over time and rapidly progresses to an acute crisis without warning.
Mesenteric artery stenosis is insufficient blood flow to the small intestine, causing intestinal ischemia.
The condition occurs when one or more of the mesenteric arteries becomes narrows or blocked. When this happens, severe abdominal pain is felt, and over some time, the blockage may worsen, resulting in the death of some tissues in the intestine due to a lack of enough blood flow.
Yes, due to the sudden and sometimes complete blockage of the superior mesenteric artery. It can accompany nausea and vomiting and should be treated as a medical emergency.
Anyone can be affected but it is predominantly found among:
a) The elderly
b) Hypertensive people
c) Obese people
d) Recent surgery
e) History of peripheral vascular disease
f) Hyperlipidemia
g) Smokers, tobacco usage etc.
It is a rare condition. The estimated number of cases is around 1 to 2 for every 1000 cases.
It is a condition that can be treated or entirely cured if diagnosed or treated early.



























































































