Portal Hypertension
“Portal hypertension” refers to the rise in the blood pressure within a system of vein cells. This system of cells is called the “portal venous system”. In this condition, a collection of cells from the stomach, intestine, pancreas, and spleen fuse into the portal vein, which then branches into smaller vessels and runs into the […] Read More
Top Doctors For Portal Hypertension Treatments
Top Hospitals For Portal Hypertension Treatments
Portal Hypertension
Table of contents
What is portal hypertension?
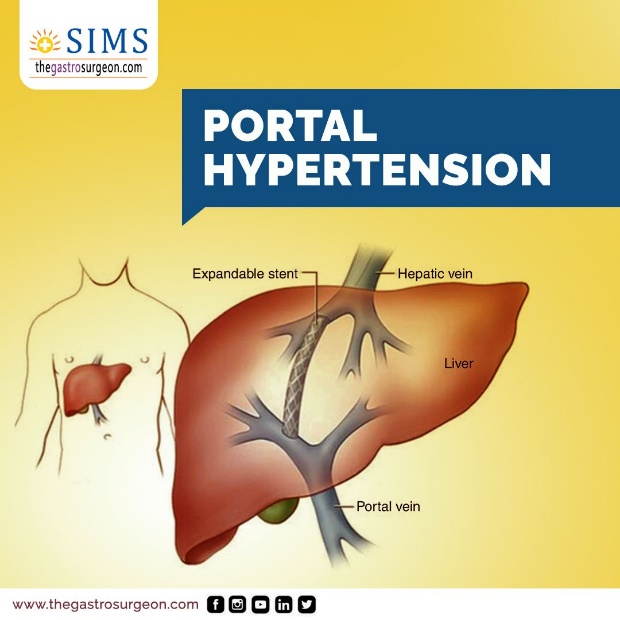
“Portal hypertension” refers to the rise in the blood pressure within a system of vein cells. This system of cells is called the “portal venous system .” In this condition, a collection of cells from the stomach, intestine, pancreas, and spleen fuse into the portal vein, which then branches into smaller vessels and runs into the liver. The liver becomes blocked, resulting in improper blood flow. This can lead to high pressure in the portal system, causing the development of large swollen veins. The enlarged veins called “varices” can rupture and bleed, resulting in severe health complications.
Causes
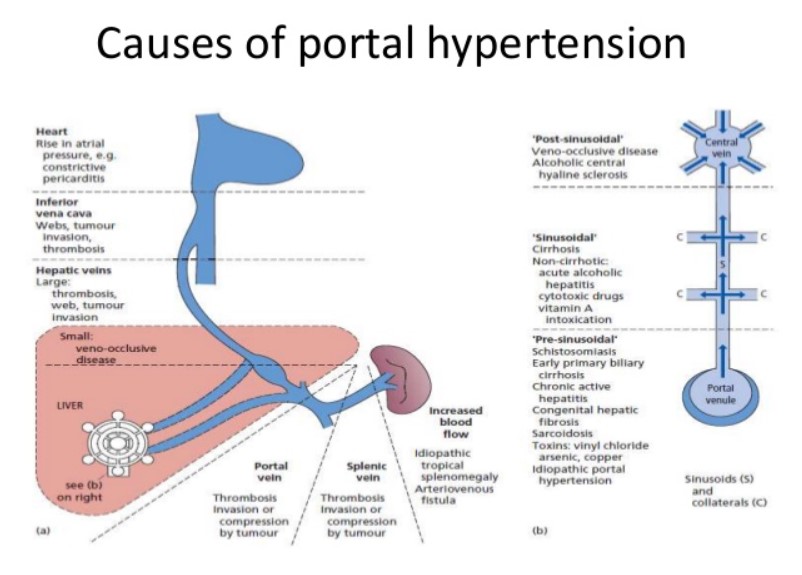
The most common cause of portal hypertension is cirrhosis of the liver, which is the scarring that accompanies the healing of the liver from an injury.
Other causes may include:
- Blood clots
- Blockages in the veins convey blood from the liver to the heart.
- Schistosomiasis; is a parasitic infection.
- Focal nodular hyperplasia.
Sometimes, the cause is unknown, and this is referred to as Non-cirrhotic or Idiopathic Portal Hypertension, a term for portal hypertension with no known cause.
Symptoms
The symptoms of this sickness include:
- Gastrointestinal bleeding due to rupture and hemorrhage of varices, indicated by:
- Bloody stools.
- Vomiting of blood.
- 2. Ascites, which is abdominal swelling caused by the accumulation of fluids
- Infections may begin to arise because the level of white blood cells becomes reduced.
- Reduced blood clotting due to the reduced level of red blood cells.
- Encephalopathy; altered brain function, which may lead to confusion and forgetfulness.
How is portal hypertension diagnosed?
The doctor will go through the patient’s medical history and perform a physical examination on the abdomen and anus to check the presence of ascites, dilated veins, or varices.
Other tests include:
- Imagery tests such as CT scans or MRI scans of the liver, X-rays like angiograms and ultrasounds, and endoscopic tests can determine the extent and severity of the patient’s condition.
- Complete blood count
- Liver function test– to check the parameters of the liver function
- Coagulation tests
- Kidney function tests, arterial blood gas (ABG), and Ph measurements
- Hemodynamic measurement of portal pressure
How is portal hypertension treated?
The treatment for this condition depends on the severity of the symptoms and how well the liver is functioning. Handling the causes of portal hypertension can also be a way of treating the condition. Treatment and control may include:
Medications
Non-selective beta-blockers such as nadolol or propranolol can be used to stop variceal bleeding. They can be used alone as a form of first-aid or combined with endoscopic therapy. Also, drugs like lactulose can be used to treat encephalopathy cases like confusion and other mental changes.
Esophageal Variceal Binding
This procedure is used as a first aid to prevent a first variceal hemorrhage, especially in patients who cannot take beta-blockers.
Endoscopic Treatment
This is a first-line treatment for variceal bleeding, which consists of banding or sclerotherapy. Banding is the use of surgical rubber bands to block off blood vessels and stop them from bleeding. Sclerotherapy is the procedure where a blood clotting solution is injected into the bleeding varices to stop them from bleeding.
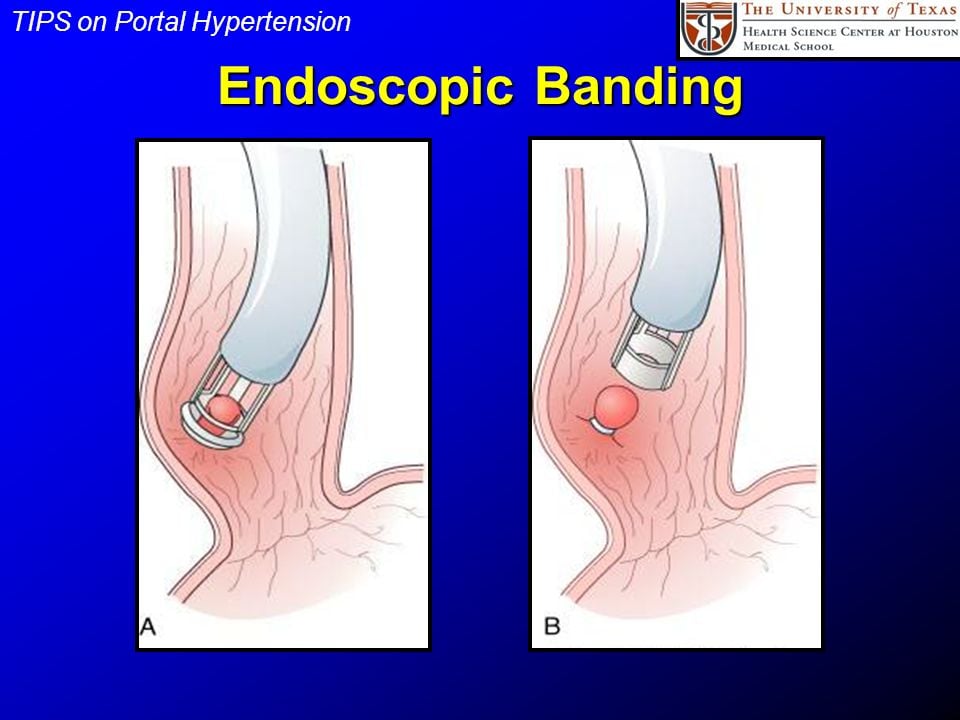
Surgery
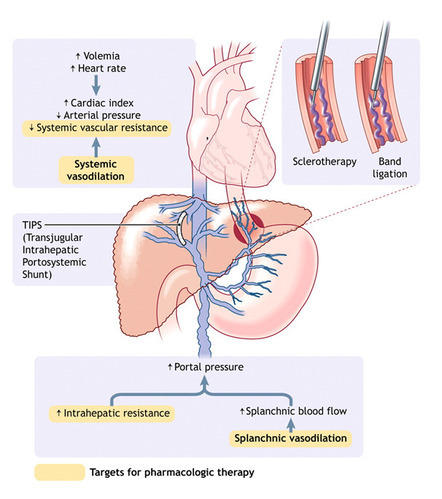
Often used when drug and endoscopic therapy fails. Surgical procedures to successfully control and reduce the pressure in the veins may be required. These decompression methods may include
- Shunting, which is the diversion of blood flow in the body. It includes:
- Transjugular Intrahepatic Portosystemic Shunt (TIPS) involves rerouting blood flow in the liver by connecting the hepatic veins with the portal veins using a tubular stent device.
- Distal Splenorenal Shunt (DSRS) is a procedure that links the veins from the spleen to those of the left kidney, thereby reducing the pressure in the varices and controlling bleeding.
- Devascularization; is a surgical procedure that removes the bleeding varices and is often done when a TIPS or DSRS is not successful.
- Liver transplant- is done in patients with end-stage liver disease. Liver transplantation is considered the ultimate shunt procedure because it relieves portal hypertension, prevents variceal rebleeding, and reduces ascites (fluid accumulation in the abdominal cavity) and encephalopathy by restoring normal liver function.
- Paracentesis is the removal of accumulated fluid in the abdomen.
How is the recovery of patients with portal hypertension?
The recovery rate depends on the severity of the complications and the individual. However, the patient needs to attend all follow-up appointments as scheduled, especially after a surgical procedure, to ensure that the parts implanted, like the stunts or liver, are functioning correctly.
What are the complications of portal hypertension?
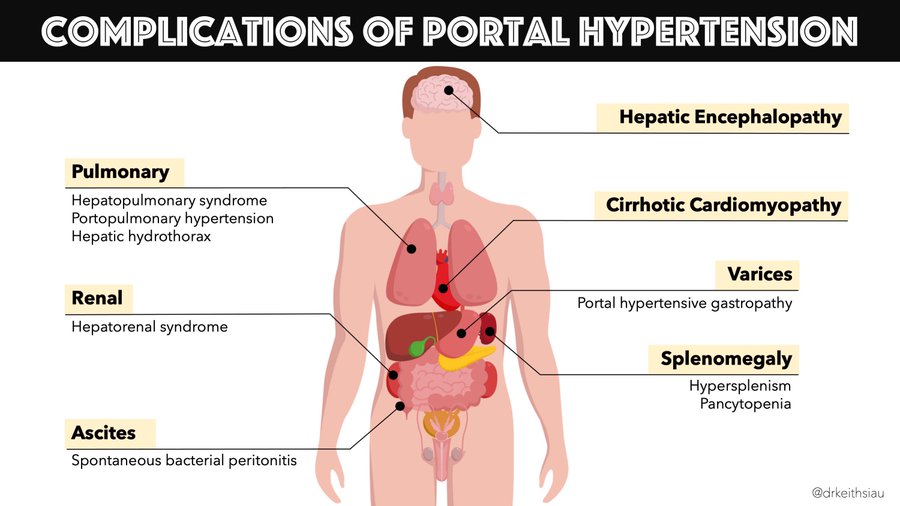
Portal hypertension can lead to:
- High blood pressure
- Ascites (excessive fluid in the abdominal cavity)
- Abdominal varices associated with portal hypertension
- Liver damage
- Heart failure
- Brain damage
- Hepatic encephalopathy (impairment in neuropsychiatric function associated with portal hypertension)
- Death
Can portal hypertension be prevented?
Maintain good nutritional habits and keep a healthy lifestyle.
- Reduce the intake of alcohol.
- Avoid smoking and the use of street drugs.
- Avoid self-medication; consult with the doctor first before embarking on any medication. Wrong medications can make liver diseases worse.
- Dietary guidelines given by the health provider, such as having a low-sodium diet, and reducing the protein intake, should be strictly adhered to.
- Consult a dietician for a healthy meal plan.
FAQ
A Gastroenterologist or Hepatobiliary surgeon should be consulted.
In the case of a surgical procedure such as a surgical stunt or a transplant, the patient can consult an Interventional Radiologist or a Surgeon.
No, it does not. Portal hypertension can be managed or cured non-surgically, but this depends on how severe the symptoms are and the cause of the condition.
In most cases, yes. Severe bleeding from various sites may cause severe complications, so it has to be checked and controlled.
No, it does not. Instead, portal hypertension is the result of structural changes within the liver that results in increased resistance to blood flow and increased pressure within the vessels.
Yes, it can, but this is a very rare case.
Portal hypertension with no known cause is called Idiopathic Portal Hypertension.
This complication in patients with liver disease or cirrhosis and ascites can be an advanced complication in portal hypertensive patients. It is the failure of the kidney due to reduced blood supply in the vessels supplying them.
This is a disorder in which blood clots develop in hepatic veins, causing an increment of pressure in the portal circulation. This can result in portal hypertension.
The complications associated with TIPS are:
a) Shunt narrowing or blockage
b) Signs of blockage include increased ascites and rebleeding
c) Acute liver failure
d) Hepatic encephalopathy
e) Dysfunction of TIPS
Normal portal pressure is generally considered to be between 5-10mmhg. However, complications may arise once the portal pressure rises to 12mmhg or greater, such as ascites and varices.
Varices mean veins become enlarged or swollen. While in esophageal varices, the enlarged veins occur on the esophagus lining. Portal hypertension leads to an increase in pressure inside the veins in the lower esophagus and stomach. These veins are not designed for higher pressure; hence, they begin to expand, resulting in varices.



























































































