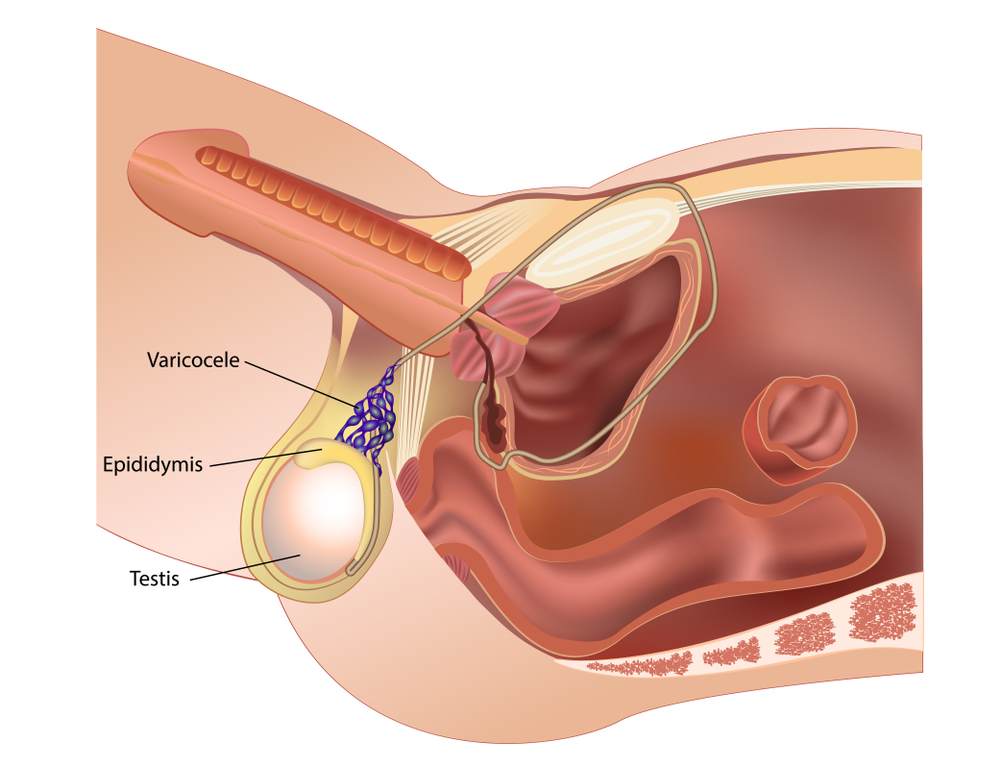
Varicocele and Male Infertility in Canada: Best Treatment Options
Testicular and scrotal varicose veins are known as varicocele. In other words, it is an enlargement of the veins within the scrotum. It can cause major issues like pain, fertility problems, or even testicular atrophy. Blood pooling in the veins instead of effectively leaving the scrotum leads to a varicocele. Veins contain a one-way valve that acts to allow the flow of blood from the testicles and scrotum back to the heart. The failure of these valves leads to the formation of a varicocele. They usually form at puberty and develop over time. While they can cause issues, they usually do not result in any symptoms or complications. They usually affect about 15% of men between the ages of 15 and 25 years. Knowledge about varicocele and male infertility in Canada will be helpful in choosing the best treatment options.
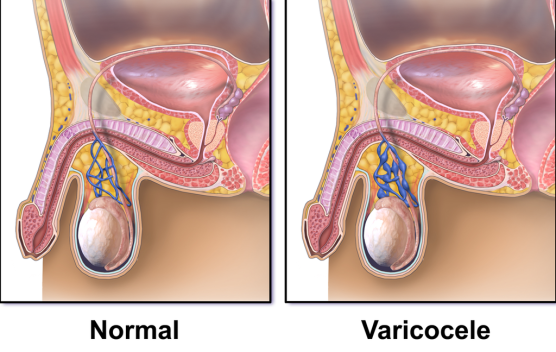
What are the symptoms of a varicocele?
A varicocele is usually found on the left side of the scrotum, and while they rarely cause pain, when there is pain it is usually worse when standing. Some other possible signs and symptoms include:
- Infertility
- Pain
- Mass in the scrotum
- Different sized testicles
While varicoceles usually go unnoticed, the individual should see a doctor when they notice the following
- Swelling in the scrotum
- A lump
- Fertility issues
Any change in the size, shape or appearance of the testes
- Veins that are unusually large and twisted
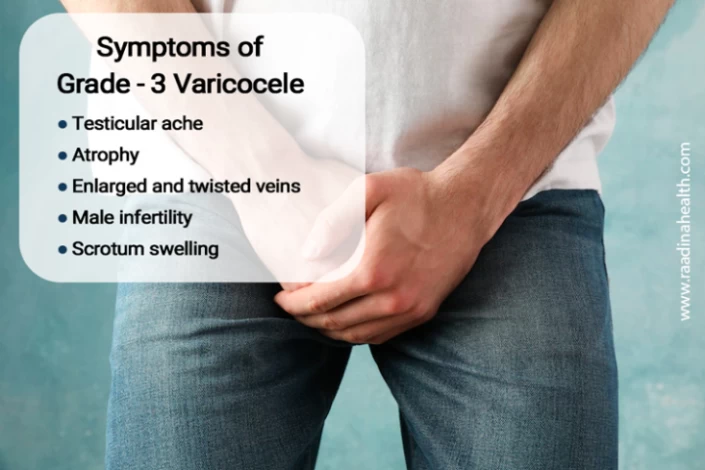
What are the complications of varicoceles?
Some of the complications that can result from varicoceles include:
- Infertility – This is the most severe complication that can result from the condition. It may occur due to the increased amount of blood in that area which increases the temperature of the testicles. About 35-44% of men with primary infertility have varicoceles; it also affects about 45-81% of men with secondary infertility. Men with varicoceles have also been found to have poorer-quality semen. Sperm production is most efficient at a temperature that is slightly lower than the body temperature.
- Hormonal imbalance – When the cells react to the increased pressure, a hormonal change can occur. There may be slightly lower or normal levels of testosterone and higher levels of luteinizing hormones.
- Testicular shrinkage – A varicocele can lead to testicular atrophy or shrinkage. If the sperm-producing tubules that make up the bulk of the testicle are damaged, it can lead to the testicles becoming smaller and softer.
What causes varicoceles?
One of the explanations for this condition is the failure of the valves in the veins that carry blood away from the testicles. The reason for this failure has not been properly established, but it is similar to the occurrence of varicoceles in the legs. The one-way valve has a malfunction, then the blood flow is disrupted, causing the blood to pool rather than move smoothly. This blood build-up causes the dilation of the veins. Varicoceles can be classified into the following types:
- Pressure types – This is where the spermatic vein fills up with blood, which then leads to a grade I varicocele
- Shunt type – In this type, a severe build-up causes damage to the spermatic vein and the surrounding veins. This causes a grade II or III varicocele
What are the risk factors?
There are no specific risk factors that are known to cause varicoceles; they most likely appear during puberty. While being taller is thought to increase the risks of it occurring, being overweight reduces the likelihood of occurrence. If varicoceles develop in a man over 40 years, it is usually due to a blockage in the larger abdominal area vein, which may be a result of a kidney tumour.
What is the diagnosis?
There are three grades of varicoceles; grade I is the smallest type and can only be felt by a doctor with a special technique called the Valsalva manoeuvre. A grade II is not visible but can be felt without the special technique. A grade III varicocele is visible. If the growth is large enough, they may feel like a soft bag of worms. A subclinical varicocele can only be detected by imaging tests; this could be through scrotal thermography or a Doppler reflux test. In this case, patients may benefit from health tourism, as the tests that are run can be achieved at a more economical and faster rate through overseas medical treatment.
Medical travel agencies or meditour agencies can help offer these types of medical tourism as a package which the patients can find more attractive than those seen in their home country. The Doppler reflux test which is also a type of ultrasound will also help to rule out or confirm other causes of the varicocele, like a tumour near or impinging on the spermatic vein. Other possible tests include semen analysis and a hormonal assay that can be done to detect high follicular stimulating hormone and low testosterone, especially if the doctor suspects a testicular dysfunction.
How can varicoceles be treated in Canada? Best Options
Treatment is not usually considered unless there is pain, low sperm count or infertility. In most cases, surgery is usually recommended. Three types of surgical techniques are possible. They include:
- Varicocelectomy – This is an open surgery that is performed under anaesthesia, local or general anaesthesia. The surgeon gains access to the area through the groin, the abdomen or the upper thigh. The surgeon then closes the affected veins, rerouting the blood through other healthier vessels. The procedure is aided by ultrasounds and surgical microscopes. There is minimal post-surgical pain, and the individual soon returns to their normal activities.
- Laparoscopic surgery – The access site is the abdomen, a small incision is made there, and surgical instruments are passed through the opening.
- Percutaneous embolization – A radiologist inserts a catheter into the body through the neck or groin. Instruments are passed through the tube, and the veins are blocked by scarring using chemicals or coils. This procedure is minimally invasive and can be done as an outpatient procedure. The recovery time is also short.
What are the risks of the surgery?
Some of the risks that can be seen in the surgery include:
- Artery damage
- Infection
- Abdominal pain
- Further testicular atrophy
- Bruising
- Swelling up of the area due to the buildup of fluids
In some cases, a renal vein thrombosis may occur; it can affect the kidney and will require further surgery. In some other instances, the veins that the blood was rerouted to may also enlarge. This will require further treatment.
The information provided in this blog is for educational purposes only and should not be considered as medical advice. It is not intended to replace professional medical consultation, diagnosis, or treatment. Always consult with a qualified healthcare provider before making any decisions regarding your health. Read more