Can Cervical Cancer Be Sexually Transmitted?
An overview
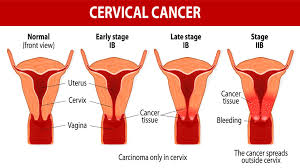
Cervical cancer is a type of cancer that grows in the cells of the cervix (the lower part of the uterus that connects to the vagina and to the upper region of the uterus or womb) and spreads to other parts of the body. The cancerous growth from the cervix then causes the cells in the body to grow rapidly and out of control.
Being a woman is the main factor that exposes to the risk of cervical cancer, especially in women above age 30. However, it commonly occurs in women that have been infected with the Human Papillomavirus, HPV, a sexually transmitted infection and the leading cause of most cervical cancer. HPV is contacted by at least 40% of sexually active women, at least once in their lifetime.
Exposure to HPV triggers an immune system response which prevents the virus from doing any harm. However, in a small percentage of women, the virus can survive some years, thereby causing the cervical cells to become cancerous.
Hence, a significant means to reduce the chances and prevent cervical cancer is to constantly carry out screening tests to detect and quickly treat HPV. The HPV vaccine is also recommended for protection.
Types of cervical cancer
There are several types of cervical cancer, and the type of cervical cancer one has determined the prognosis and the type of cervical treatment given.
However, the major types of cervical cancer are two – Adenocarcinomas and Squamous cell carcinomas. Sometimes these two types of cervical cancer can occur in one person.
Adenocarcinoma. This type of cervical cancer originates from the column-shaped glandular cells that line the cervical canal. This type of cervical cancer occurs in about 20% of all cervical cancer cases.
Squamous cell carcinoma. This type of cervical cancer develops in the flat, thin cells (squamous cells) that line the outer part of the cervix, which projects into the birth canal (that is, the vagina). Most types of cervical cancers are squamous cell carcinomas, and it accounts for about 80% of all cervical cancer cases.
At times, both cells are involved in cervical cancer and very rarely does cancer occur outside these cells in the cervix.
Causes
Cervical cancer begins when healthy cells in the cervix start to develop changes (that is mutates) in their DNA, which is responsible for giving instructions to cells on what to do.
Healthy and normal cells grow and multiply at a fixed rate and die at a given time. The mutations that occur in these cells interfere with the DNA’s message and tell the cells to grow and multiply irregularly and out of control, and not to die. The absence of death leads to an accumulation of abnormal cells, which in turn leads to the formation of a tumour. These cancerous cells break off from a tumour and then begin the invasion of nearby tissues to spread elsewhere in the body.
While it isn’t clear what causes cervical cancer, it’s certain that (high risk) HPV (such as HPV 16, HPV 18, HPV 31, HPV 33 and HPV 35) plays a huge role. Also, while HPV is very common, most people living with the virus never develop cancer.
Other factors, such as environment or lifestyle choices also contribute to the development of cervical cancer.
Cancer cervical symptoms
Cervical cancer symptoms are completely absent in the early stages of the condition. Cervical cancer symptoms begin to appear when cancer becomes more advanced.
Probable cervical cancer symptoms that may appear include –
- Vaginal bleeding may occur after intercourse, between menstrual periods or after attaining menopause.
- Increased vaginal discharge, which may be watery, bloody, heavy and foul-smelling.
- Pelvic pain.
- Pain during intercourse.
- Weight loss, fatigue, loss of appetite;
- Vaginal discomfort; and
- Swelling in a leg or both of the lower extremities.
Risk factors for cervical cancer
The risk factors for cervical cancer include:
- Multiple sexual partners: The more sexual partners a woman has and/or the more sexual partner her sexual partner has, the higher the chances of acquiring HPV, which can lead to cervical cancer.
- Early sexual activity: Starting to have sex at an early age increases the risk of contracting HPV.
- Other sexually transmitted infections (STIs): Having other STIs, such as chlamydia, syphilis, gonorrhoea and HIV/AIDS increases the risk of contracting HPV also.
- A weakened immune system: A weak immune system, the chances of developing cervical cancer is highly increased, especially when you have been confirmed to HPV.
- Smoking: It has been established that smoking is associated with squamous cell cervical cancer.
- Exposure to miscarriage prevention drug: If in the 1950s your mother took the drug known as diethylstilboestrol (DES) while pregnant, you may be at an increased risk of a certain type of cervical cancer known as clear cell adenocarcinoma.
Other likely risk factors for cervical cancer maybe
- Sexual intercourse with a man whose partner has cervical cancer.
- Over three full-term pregnancies, or a full-term pregnancy before the age of 17.
- A family history of cervical cancer could also put one at high risk
- Long term use (that is, above 5 years) of oral contraceptives.
- Chlamydia infection.
Cervical Cancer Treatment
There are different types of cervical cancer treatment available. While some cervical cancer treatment method have been standardized, other cervical cancer treatment procedure are still being tested.
To begin with, cervical cancer treatment depends on a number of factors, which include:
- The type of cervical cancer that has been diagnosed.
- The age of the patient.
- The stage of cancer.
- The patient’s wish to have children.
Available cervical cancer treatment options include:
- Surgery
- Targeted therapy
- Immunotherapy
- Radiation therapy
- Chemotherapy
FAQs
How can I prevent cervical cancer?
- Carry out routine Pap tests: This helps detects precancerous conditions of a cervix. Carrying out this test routinely helps to monitor the situation of things and know when to commence treatment in order to prevent cervical cancer. It is advisable to begin carrying out routine pap tests at age 21 and to repeat them often.
- Practice safe sex: You can reduce your risk of cervical cancer by taking measures to prevent sexually transmitted infections and limiting the number of sexual partners you have.
- Don’t smoke: Smoking is a major risk factor for cervical cancer. If you smoke, talk to your doctor about tactics to help you quit. If you don’t smoke, well don’t start.
Is there a vaccine to prevent cervical cancer?
According to the World Health Organisation, there are presently 3 vaccines that have been prequalified for use to prevent cervical cancer. They all protect against both HPV 16 and 18, which have been identified to cause at least 70% of cervical cancers. The third vaccine offers protection against five additional types of oncogenic HPV, which cause a further 20% of cervical cancers.
The WHO considers the three vaccines equally protective to prevent cervical cancer.
Who should get vaccinated?
Anyone between the age 11 and 26 years can and should be vaccinated. Vaccination is not recommended for anyone older than 26 years old.
How common is cervical cancer?
Annually about 500,000 new cases of cervical cancer are diagnosed globally, and there are about 300,000 cervical cancer-related deaths per year. There is a projection that more than one million new cases of cervical cancer will occur per year by 2050.
Can cervical cancer treatment be done during pregnancy?
Cervical cancer treatment during pregnancy depends on the phase of the pregnancy, and also the type and stage of cervical cancer. Usually, cervical cancer treatment is delayed until after birth.
Are all types of cervical cancer sexually transmitted?
Almost all squamous cervical cancers are a result of a common sexually transmitted infection known as human papillomavirus (HPV). This does not, however, mean that a woman that has been diagnosed with cervical cancer is sexually promiscuous.
The information provided in this blog is for educational purposes only and should not be considered as medical advice. It is not intended to replace professional medical consultation, diagnosis, or treatment. Always consult with a qualified healthcare provider before making any decisions regarding your health. Read more