Medullary Carcinoma
Medullary Carcinoma is a unique and somewhat less-aggressive type of infiltrating ductal carcinoma. It is named according to its appearance, which resembles the tissues of the ‘Medulla oblongata’ … Read More
Top Doctors For Medullary Carcinoma Treatments
Top Hospitals For Medullary Carcinoma Treatments
Medullary Carcinoma
Table of contents
What is medullary carcinoma?
Medullary Carcinoma is a unique and less aggressive type of infiltrating ductal carcinoma. It is named according to its appearance, which resembles the tissues of the “Medulla oblongata” region of the brain stem. Medullary carcinoma is a term used to refer to several different tumors of epithelial origin. The term’ medulla’ is a general anatomic descriptor for the mid-layer of numerous organ tissues. A medullary tumor, therefore, arises from the “mid-layer tissues” of relevant organs. Also, the term medullary carcinoma is most commonly used to refer to:
- Medullary thyroid cancer, and
- Medullary carcinoma of the breast.
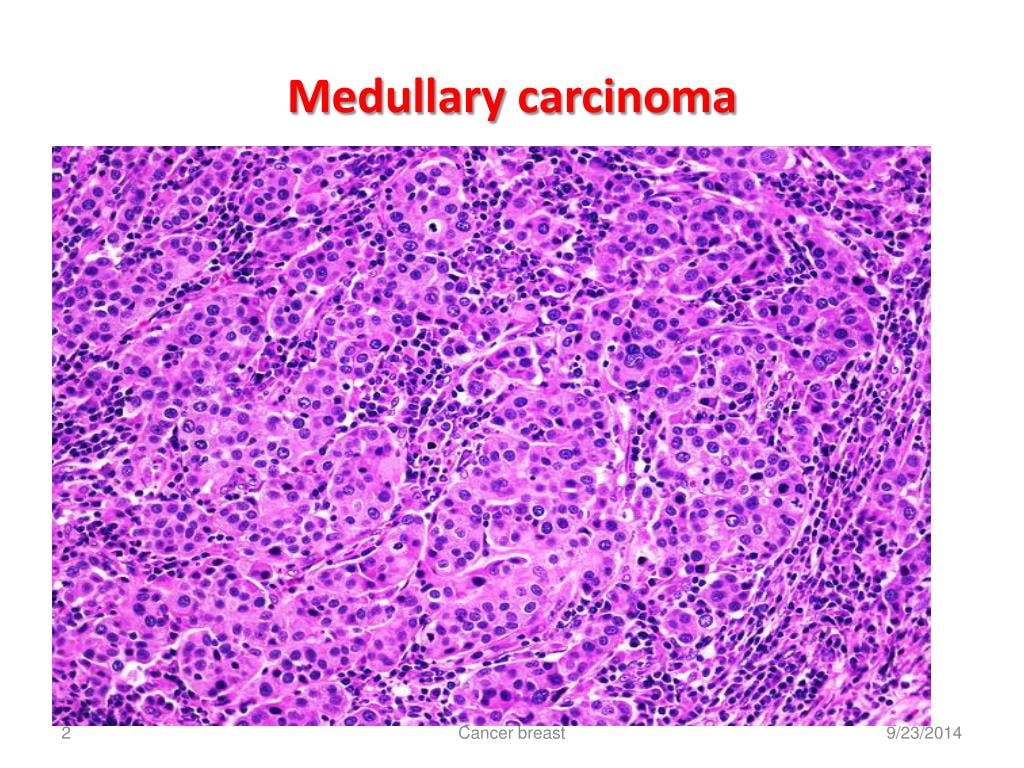
What is medullary carcinoma breast?
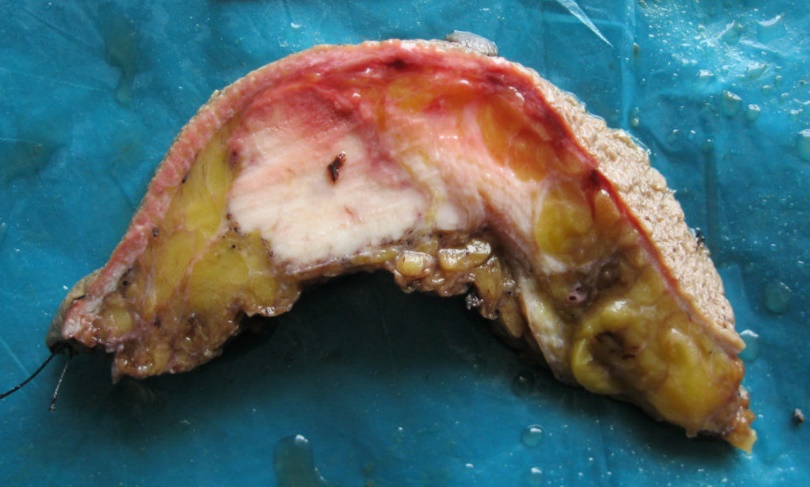
Medullary carcinoma breast is a very rare subtype of invasive ductal carcinoma (that originates from the milk duct and spreads beyond it), accounting for about 3 to 5% of all breast cancer cases. Being a medullary carcinoma, the tumor is soft and fleshy and resembles the part of the brain known as the medulla. Medullary carcinoma breast may occur at any age. But usually affects women in their late 40s and early 50s and is more common in women with the BRCA1 mutation. The affected breast cells appear high-grade but behave low-grade. They look aggressive and like highly abnormal cancer cells but don’t act like one. Medullary carcinoma breast grows slowly and doesn’t spread to the lymph nodes. Thus, it’s easier to treat than other breast cancer forms.
What is thyroid medullary carcinoma?
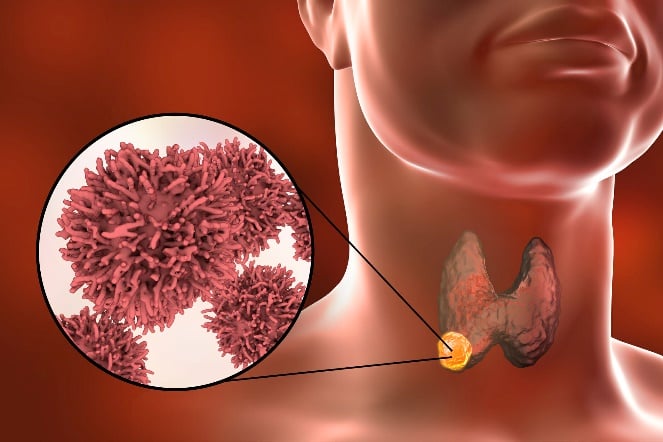
Thyroid medullary carcinoma is a form of thyroid gland cancer, unlike other thyroid gland cancers (which originate from the follicular cells); it originates in the parafollicular cells (C cells) of the thyroid that synthesizes a hormone known as calcitonin. About 90% of these tumors release calcitonin. About 80 to 90% of thyroid medullary carcinoma are sporadic and are seen in adults. The rest can be seen in children with genetic syndromes known as multiple endocrine neoplasias, popularly known as MEN syndrome. Thyroid medullary carcinoma accounts for about 5% of all thyroid cancer cases.
Causes
- Thyroid medullary carcinoma: Its occurrence is rare, and the cause is unknown (idiopathic).
- Medullary carcinoma breast: It occurs when a woman experiences changes in the genetic makeup of cells in her breast. Thereby causing the uncontrollable growth of the cells. The exact reasons for mutations are unknown, nor are they related to the breast’s medullary carcinoma.
- It is not known what causes medullary carcinoma (MTC). MTC is very rare.
- It can occur in children and adults.
- MTC is not as common as other forms of thyroid cancer. It’s less likely that radiation therapy to the neck was used to treat other cancers in childhood.
Symptoms
For medullary carcinoma breast, symptoms may go unnoticed in the early stages. Over time, a lump grows large enough to be felt during a self-breast examination. However, the following symptoms may occur later on:
- Breast swelling or tenderness.
- Redness, scaling or dimpling of the breast skin or nipple.
- Unusual nipple discharge and pain.
A lump or nodule develops in the thyroid for thyroid medullary carcinoma, which may not cause any symptoms. Symptoms usually appear only in advanced stages, and they include;
- Pain in the neck, jaw, or ear.
- Difficulty with breathing or swallowing.
- Hoarseness, if cancer overruns the nerve that controls vocal cords.
- Neck lump.
- The most common sign is a single lump at the front of your neck.
- Neck pain.
- Hoarseness.
- Coughing
- Trouble swallowing (Dysphagia).
- Shortness of breath (dyspnea).
Diagnosis
Medullary thyroid cancer (MTC) is usually diagnosed on physical examination as a solitary neck nodule, and early spread to regional lymph nodes is common. The following tests are done to identify the exact nature of cancer:
- Ultrasonography of the thyroid gland and surrounding lymph nodes
- Fine Needle Aspiration (FNA) of the tumor or lymph nodes.
- In the case of inherited forms of MTC, DNA testing for RET gene can be a beneficial diagnostic tool.
Diagnosis of medullary carcinoma of the breast can be done by:
- Physical examination: During the physical examination, the doctor will examine the breast thoroughly and look for any lump or mass in the breast. The doctor will advise the patient to undergo a few tests to confirm the diagnosis.
- Investigation scans include: ultrasonography of the breasts, x-ray mammograms, and MRI scans (magnetic resonance imaging)
- Biopsy of the lump: During this procedure, a small tissue sample is taken from the tumor and sent for pathological evaluation.
FAQ
Medullary carcinoma breast responds better to breast cancer treatment than the other forms of invasive ductal carcinomas. Early detection and prompt treatment make prognosis and survival rates highly favorable.
A 2016 study observed the survival rates for regular and atypical medullary carcinoma breast cancer among 3,688 people. The findings reported a 5-year survival rate of 89 to 92% and a 10-year survival rate of 85 to 87%.
The factors that increase the risk of thyroid medullary carcinoma are;
a) A family history of thyroid medullary carcinoma.
b) Family history of multiple endocrine neoplasias, MEN.
c) A history of mucosal neuromas, pancreatic endocrine tumors or hyperparathyroidism.
Thyroid medullary carcinoma are two forms;
a) Sporadic thyroid medullary carcinoma, which is non-hereditary. Most thyroid medullary carcinoma is of a sporadic nature and mainly affects older adults.
b) Hereditary thyroid medullary carcinoma. That is, it runs in families.
So, yes, it can be inherited.
The 5- and 10- year thyroid medullary carcinoma survival rate is 65 to 89% and 71 to 87%, respectively
The risk factors for medullary carcinoma of the thyroid are:
1) Inherited (hereditary) thyroid carcinoma- MEN 2A, MEN 2B,
2) Sporadic cause
3) Abnormality in RET gene
4) Gender- females>males (3:2)
5) Age- between 40-60years of age
6) Hormonal imbalance
The risk factors for medullary carcinoma of the breast are:
1) Abnormality in gene mutation of BRCA1 gene
2) Hereditary cause
3) Patient with a history of breast cancer
4) Age- between 45-52 years of age
The treatment options for medullary carcinoma of the thyroid are:
1) Total Thyroidectomy– During this procedure, the thyroid gland is removed completely. It is considered the first-line treatment for this condition.
2) Radiation therapy– During this procedure, an external beam of radiation is used to kill the cancer cells.
3) Tyrosine kinase inhibitors- They are a group of anti-cancer drugs used to treat the condition
4) Chemotherapy
5) Radioactive iodine
The treatment options for medullary carcinoma of the breast are:
1) Surgery- They include total mastectomy (removal of the complete breast along with nipple), breast-conserving surgery, also known as wide local excision or lumpectomy (where only the tumor and some portions of healthy tissues are removed)
2) Sentinel lymph node excision
3) Chemotherapy
4) Radiation therapy
5) Hormonal therapy– During this therapy, they block or stop the effect of estrogen on the cancer cells.
6) Targeted therapy- During this therapy, a group of drugs blocks the growth of cancer cells. This therapy is less likely used in this condition.
7) Biphosphonates- They are a group of drugs that can reduce the risk of the spread of cancer in postmenopausal women.

































































































